What causes a Herniated Disc and how is it treated?
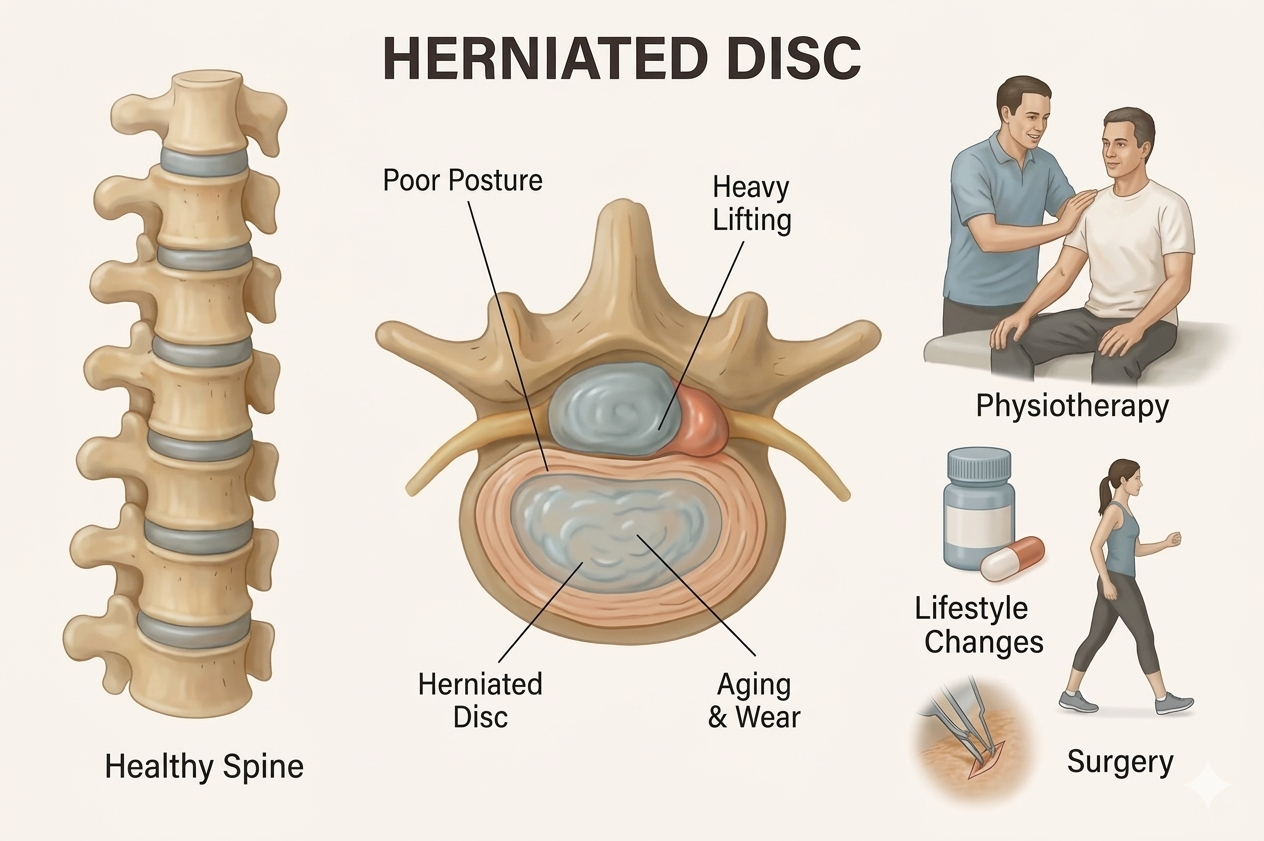
Why Herniated Discs Are So Common Today
Back pain is one of the most widespread health problems worldwide, and a leading cause of missed work. Among its many causes, one condition stands out as both common and often misunderstood — the herniated disc (also known as a slipped or ruptured disc).
A herniated disc occurs when the soft, gel-like center of a spinal disc pushes out through a tear in its tough outer layer. This can irritate or compress nearby spinal nerves, leading to pain, numbness, tingling, or weakness in the back, neck, arms, or legs.
According to the National Institutes of Health (NIH), herniated discs are most common in people aged 30 to 50, but they can occur at any age depending on lifestyle and risk factors. With the rise of sedentary desk jobs, long screen hours, and poor posture habits, cases of spinal disc problems are increasing, especially in countries like India.
This blog explains the condition in detail:
- What a herniated disc is
- What causes it
- Symptoms and risk factors
- How doctors diagnose it
- Treatment options (both non-surgical and surgical)
- Recovery and long-term prevention
All information here is strictly factual, based on trusted medical organizations like the World Health Organization (WHO), Mayo Clinic, Cleveland Clinic, and peer-reviewed studies.
Understanding the Spine and Spinal Discs
To understand how and why discs herniate, it helps to first look at the spine’s structure.
- The human spine is made up of 33 vertebrae stacked on top of each other.
- Between most of these bones lie intervertebral discs, which act like cushions or shock absorbers.
- Each disc has two parts:
-Nucleus pulposus: A soft, gel-like center that provides flexibility and cushioning.
-Annulus fibrosus: A tough, fibrous outer ring that keeps the nucleus in place.
These discs allow the spine to bend, twist, and absorb everyday forces from walking, lifting, or even sitting.
A herniated disc happens when part of the nucleus pulposus pushes through a crack in the annulus fibrosus. This protrusion can:
- Compress spinal nerves
- Cause local inflammation
- Lead to symptoms ranging from mild discomfort to severe pain and weakness
What Causes a Herniated Disc?
1. Age-Related Degeneration
The most common cause is natural aging. As people grow older:
- Discs lose water content, becoming less flexible.
- The annulus fibrosus weakens, making tears more likely.
- Even minor stresses (bending, twisting, coughing) can trigger herniation.
This process is called degenerative disc disease, and it explains why herniated discs are common after age 30.
2. Repetitive Strain and Poor Posture
Modern desk jobs put enormous stress on spinal discs. Prolonged sitting increases lumbar disc pressure by 40% compared to standing (Nachemson’s biomechanical study, 1970s). Poor posture — slouching, hunching, forward head tilt — makes it worse.
Over time, this continuous strain weakens discs, setting the stage for herniation.
3. Heavy Lifting or Sudden Strain
Lifting heavy objects incorrectly (bending at the waist instead of the knees) is a major cause. The sudden load on the lumbar spine can tear the annulus and push the nucleus outward.
4. Obesity
Excess body weight adds constant pressure on the lumbar spine. According to the Mayo Clinic, obesity is a significant risk factor for disc herniation, especially in the lower back.
5. Sedentary Lifestyle
Lack of physical activity weakens the core and back muscles that support the spine. Weak support means more stress falls on the discs, making them vulnerable.
6. Smoking
Studies in Spine Journal show smoking reduces oxygen supply to discs, accelerating degeneration and slowing healing.
7. Genetics
Some people inherit weaker disc structures, making them prone to herniation earlier in life.
8. Occupational Risks
Jobs involving repetitive lifting, twisting, driving, or vibration (e.g., truck driving, construction work) increase risk. On the other hand, long hours of office work without movement also contribute to disc damage.
9. Pregnancy
During pregnancy, hormonal changes loosen ligaments, while added weight and posture shifts increase spinal stress, raising the risk of disc problems.
Symptoms: How to Recognize a Herniated Disc
Not everyone with a herniated disc has symptoms. But when nerves are compressed, typical signs include:
1. Pain
- Lumbar herniation (lower back): Pain radiates to buttocks, thighs, and legs (sciatica).
- Cervical herniation (neck): Pain spreads to shoulders, arms, and hands.
2. Numbness or Tingling
Affected nerves may cause sensations of pins and needles in arms, hands, legs, or feet.
3. Muscle Weakness
Compression reduces nerve signals, making it hard to lift objects, grip firmly, or walk steadily.
4. Worsening with Movement
Symptoms often worsen when sitting, bending, or coughing, and may improve when lying down.
Red Flags (Seek Immediate Medical Help):
- Loss of bladder or bowel control
- Severe weakness in legs
- Numbness in the inner thighs or around the anus (cauda equina syndrome — a medical emergency)
Diagnosis: How Doctors Confirm a Herniated Disc
Diagnosis combines medical history, physical exam, and imaging tests:
1. Physical Examination
- Checking reflexes, muscle strength, walking ability, and sensation.
- Straight leg raise test for lumbar herniation.
2. Imaging Tests
- MRI: Gold standard for identifying herniation and nerve compression.
- CT Scan: Helpful when MRI isn’t possible.
- X-ray: Rules out other spine problems but doesn’t show discs.
3. Nerve Tests
- Electromyography (EMG): Measures electrical activity of muscles.
- Nerve conduction studies: Show how well electrical signals travel.
Treatment: How Is a Herniated Disc Managed?
Most patients improve without surgery. The American Association of Neurological Surgeons (AANS) notes that 90% of herniated disc cases improve within 6 weeks with conservative treatment.
Non-Surgical Treatments
1. Rest and Activity Modification
- Avoid heavy lifting and bending.
- Bed rest is discouraged; light activity aids recovery.
2. Medications
- NSAIDs (ibuprofen, naproxen): Reduce pain and inflammation.
- Muscle relaxants: For spasms.
- Nerve pain drugs (gabapentin, pregabalin): For radiating pain.
- Corticosteroid injections: Provide temporary relief.
3. Physical Therapy
Supervised exercises help:
- Strengthen core muscles.
- Improve flexibility.
- Correct posture and body mechanics.
- Relieve nerve pressure.
4. Heat and Cold Therapy
Cold packs reduce inflammation; heat relieves stiffness.
5. Lifestyle Modifications
- Weight management.
- Quitting smoking.
- Ergonomic workstations.
- Regular stretching breaks.
Surgical Treatments
Surgery is considered if:
- Pain lasts >6–12 weeks despite conservative care.
- Severe weakness or nerve compression exists.
- Cauda equina syndrome develops (emergency).
1. Microdiscectomy
- Minimally invasive; removes herniated disc material pressing on nerves.
- High success rate for sciatica relief.
2. Laminectomy
- Removes part of the vertebra (lamina) to relieve pressure.
3. Artificial Disc Replacement
- Replaces damaged disc with an artificial one; used selectively.
4. Spinal Fusion
- Joins two vertebrae for stability; usually last resort.
Conservative vs. Surgical Treatment of Herniated Disc
Recovery and Rehabilitation
Recovery depends on severity and treatment method:
- Non-surgical patients: Most recover within 6 weeks–3 months.
- After microdiscectomy: Recovery in 4–6 weeks; light activity resumes earlier.
- Rehabilitation: Includes physiotherapy, strengthening, and posture training.
Important: Recovery doesn’t end with pain relief. Long-term prevention strategies are crucial to avoid recurrence.
At We Are Spine, the focus is on evidence-based diagnosis and treatment of spinal conditions, including herniated discs. The team emphasizes thorough clinical evaluation, advanced imaging when necessary, and a patient-first approach to selecting treatment—whether conservative management or surgical intervention. The goal is always to relieve pain, restore mobility, and help patients return to their daily lives safely.
Prevention: Protecting Your Spine
- Exercise Regularly
- Core strengthening (planks, bridges).
- Low-impact aerobics (walking, swimming, cycling).
- Maintain Healthy Weight
- Reduces spinal load.
- Quit Smoking
- Improves disc nutrition.
- Practice Good Posture
- Sit with feet flat, back supported, and screen at eye level.
- Lift Safely
- Bend knees, keep load close, avoid twisting.
- Take Breaks
- Avoid sitting >30–45 minutes at a stretch.
Conclusion: Understanding and Acting Early
A herniated disc can be painful and limiting, but it doesn’t have to define your life. Most cases improve with conservative treatments, and surgery is effective when truly needed.
The real key lies in prevention and awareness:
- Knowing the causes
- Recognizing early symptoms
- Maintaining a healthy lifestyle
- Practicing safe posture and regular exercise
Your spine supports you through every stage of life. Protecting it with mindful habits and timely medical care is one of the best investments you can make for long-term health.

