L5 S1 Disc Bulge Symptoms: Early Warning Signs You Shouldn’t Ignore

L5 S1 Disc Bulge Symptoms: Early Warning Signs You Shouldn’t Ignore Lower back pain is often dismissed as a minor issue, but when it starts radiating down your leg or causes numbness, it may point to something more serious like an L5 S1 disc bulge. Recognizing L5 S1 disc bulge symptoms early is crucial. Delayed diagnosis can lead to nerve damage, chronic pain, and longer recovery time. This guide will help you clearly identify symptoms, understand their severity, and know when to seek help. Direct Answer: L5 S1 Disc Bulge Symptoms L5 S1 disc bulge symptoms typically include lower back pain, sciatica (radiating leg pain), numbness, tingling, and muscle weakness. Symptoms often worsen with sitting, bending, or lifting and may improve with rest or posture correction. What is an L5 S1 Disc Bulge? The L5-S1 disc is located at the base of the spine, where the lumbar spine meets the sacrum. This area absorbs maximum stress from daily activities like walking, sitting, and lifting. A disc bulge occurs when: The outer layer weakens The disc protrudes outward It presses on nearby nerves (especially the sciatic nerve) This pressure leads to the most common L5 S1 disc bulge symptoms. Common L5 S1 Disc Bulge Symptoms 1. Lower Back Pain Persistent or intermittent pain in the lower back Can range from dull ache to sharp discomfort Often worsens after long sitting or standing Sciatica (Radiating Leg Pain) One of the most defining L5 S1 disc bulge symptoms. Pain travels from lower back → buttock → leg → foot Usually affects one side of the body Can feel like burning, shooting, or electric pain Numbness and Tingling “Pins and needles” sensation in the leg or foot Indicates nerve involvement May come and go or become constant Muscle Weakness Weakness in legs or feet Difficulty lifting the foot (foot drop in severe cases) Trouble walking or climbing stairs Pain While Sitting or Bending Sitting increases disc pressure Bending forward may worsen symptoms Long desk hours can aggravate condition Early vs Severe Symptoms (Comparison Table) Stage Symptoms Early Mild back pain, stiffness, occasional discomfort Moderate Radiating pain, numbness, tingling Severe Muscle weakness, persistent sciatica, reduced mobility Understanding the progression helps identify L5 S1 disc bulge symptoms before they worsen. Why L5 S1 Disc Bulge Symptoms Occur The symptoms are primarily caused by nerve compression. Main Reasons: Disc pressing on sciatic nerve Inflammation around spinal nerves Reduced disc cushioning This explains why L5 S1 disc bulge symptoms often involve both back and leg pain. Factors That Can Worsen Symptoms Certain habits can intensify L5 S1 disc bulge symptoms: Prolonged sitting (especially desk jobs) Poor posture Heavy lifting Sudden twisting movements Lack of physical activity Benefits of Early Symptom Recognition Identifying L5 S1 disc bulge symptoms early can: Prevent nerve damage Reduce recovery time Avoid surgery Improve treatment outcomes Maintain mobility Limitations & Diagnostic Challenges While symptoms are helpful, they are not always definitive: Similar symptoms may occur in sciatica or muscle strain Pain intensity doesn’t always reflect severity Imaging (MRI) may be required for confirmation Some patients may have minimal symptoms despite disc bulge Real-World Example Case 1: A 29-year-old notices mild lower back pain → ignores it → develops leg pain within weeks Case 2: A 40-year-old identifies early symptoms → starts physiotherapy → prevents progression This shows how awareness of L5 S1 disc bulge symptoms can change outcomes significantly. Step-by-Step: What To Do If You Notice Symptoms Step 1: Monitor Your Pain Track location, intensity, and triggers Step 2: Modify Activities Avoid prolonged sitting and heavy lifting Step 3: Start Basic Care Use ice/heat and gentle stretching Step 4: Consult a Specialist Get clinical evaluation and imaging if needed Step 5: Begin Treatment Follow physiotherapy and medical advice When to See a Doctor Immediately Seek urgent medical attention if you notice: Severe weakness in legs Loss of bladder or bowel control Persistent numbness Unbearable pain These could indicate serious nerve compression. Frequently Asked Questions What are the first L5 S1 disc bulge symptoms? Early L5 S1 disc bulge symptoms include mild lower back pain, stiffness, and discomfort after sitting. Does L5 S1 disc bulge always cause leg pain? Not always, but leg pain (sciatica) is a common symptom when nerves are compressed. Can symptoms come and go? Yes, L5 S1 disc bulge symptoms can fluctuate depending on activity and posture. Are symptoms worse at night? They can worsen due to poor sleeping posture or prolonged inactivity. Early L5 S1 disc bulge symptoms include mild lower back pain, stiffness, and discomfort after sitting. Not always, but leg pain (sciatica) is a common symptom when nerves are compressed. Yes, L5 S1 disc bulge symptoms can fluctuate depending on activity and posture. They can worsen due to poor sleeping posture or prolonged inactivity. Conclusion: Don’t Ignore L5 S1 Disc Bulge Symptoms Recognizing L5 S1 disc bulge symptoms early can prevent long-term complications and speed up recovery. What starts as mild back pain can quickly progress into nerve-related issues if left untreated. The key is awareness and timely action. If you’re experiencing persistent pain, tingling, or weakness, don’t ignore it.
L5 S1 Disc Bulge Treatment: Complete Guide to Relief & Recovery

L5 S1 Disc Bulge Treatment: Complete Guide to Relief & Recovery Lower back pain that shoots down your leg, numbness, or difficulty sitting for long hours can often be traced back to one common issue, the L5 S1 disc bulge. Because this disc bears maximum body weight and movement stress, it’s highly vulnerable to injury. If you’ve been diagnosed recently, the most important question is: What is the best L5 S1 disc bulge treatment? The good news is that most cases can be treated successfully without surgery, if addressed early and managed correctly. Understanding common L5 S1 disc bulge symptoms early can help you start treatment before the condition worsens. Direct Answer: L5 S1 Disc Bulge Treatment L5 S1 disc bulge treatment typically involves a combination of rest, physiotherapy, pain management, and lifestyle changes. In most cases, symptoms improve within weeks. Severe cases with nerve compression may require injections or surgery, but these are less common. Knowing the expected L5 S1 disc bulge recovery time can help set realistic expectations. What is an L5 S1 Disc Bulge? The L5-S1 disc sits at the base of your spine and absorbs shock during movements like walking, bending, and lifting. A disc bulge occurs when: The outer disc weakens The inner material pushes outward Nearby nerves (like the sciatic nerve) may get compressed This is why symptoms often include sciatica, leg pain, or tingling sensations. L5 S1 Disc Bulge Treatment Options 1. Conservative Treatment (First-Line Approach) Most doctors recommend non-surgical L5 S1 disc bulge treatment initially. a. Rest & Activity Modification Avoid heavy lifting Limit prolonged sitting Continue light movement (avoid complete bed rest) b. Medications NSAIDs (to reduce inflammation) Muscle relaxants (for spasms) Nerve pain medications (if needed) c. Physiotherapy This is the most important part of L5 S1 disc bulge treatment. Includes: Core strengthening exercises Stretching routines Posture correction techniques McKenzie exercises (commonly recommended) 2. Advanced Non-Surgical Treatments If pain persists beyond a few weeks: a. Epidural Steroid Injections Reduce inflammation around nerves Provide temporary but significant relief b. Chiropractic Care May help in selected cases Should be done cautiously under expert supervision 3. Surgical Treatment (Last Resort) Surgery is considered only when: Severe nerve compression Loss of bladder/bowel control Persistent pain beyond 3–6 months Common Procedures: Microdiscectomy Laminectomy Even in these cases, surgery is highly targeted and minimally invasive. Comparison Table: Treatment Options Treatment Type When Used Effectiveness Recovery Rest & Medication Early stage Moderate 2–4 weeks Physiotherapy Most cases High 4–12 weeks Injections Persistent pain High (short-term) Few weeks Surgery Severe cases Very high 6–12 weeks Benefits of Early L5 S1 Disc Bulge Treatment Starting L5 S1 disc bulge treatment early offers clear advantages: Faster pain relief Reduced nerve damage risk Avoidance of surgery Improved mobility and function Lower recurrence rates Limitations & Challenges No treatment is perfect, and it’s important to be realistic: Pain relief may take time Some exercises may initially increase discomfort Recurrence is possible without lifestyle changes Not all patients respond equally to the same treatment Real-World Example Case A: A 30-year-old IT professional starts physiotherapy within 10 days → significant improvement in 5 weeks Case B: A 42-year-old delays treatment → requires injections after 3 months This highlights why early L5 S1 disc bulge treatment is critical. Step-by-Step Treatment Plan Step 1: Diagnosis Clinical evaluation MRI if required Step 2: Pain Control Medications Ice/heat therapy Step 3: Start Physiotherapy Guided exercises Posture correction Step 4: Lifestyle Adjustment Ergonomic workspace Avoid prolonged sitting Step 5: Follow-Up Monitor progress Adjust treatment plan Tools & Support for Recovery Lumbar support belts Ergonomic chairs Standing desks Posture correction apps Spine tools checkup Frequently Asked Questions What is the best L5 S1 disc bulge treatment? The best L5 S1 disc bulge treatment includes physiotherapy, posture correction, and pain management. Surgery is rarely required. Can L5 S1 disc bulge heal without surgery Yes, most cases improve with conservative treatment within weeks to months. Is bed rest good for disc bulge? Short rest is helpful, but prolonged bed rest can delay recovery. How long does treatment take? Typical recovery takes 4–12 weeks with proper L5 S1 disc bulge treatment. What exercises should I avoid? Avoid heavy lifting, high-impact workouts, and deep bending movements. Can I work with a disc bulge? Yes, with ergonomic adjustments and limited sitting time. When should I see a doctor? If pain persists, worsens, or causes numbness/weakness. The best L5 S1 disc bulge treatment includes physiotherapy, posture correction, and pain management. Surgery is rarely required. Yes, most cases improve with conservative treatment within weeks to months. Short rest is helpful, but prolonged bed rest can delay recovery. Typical recovery takes 4–12 weeks with proper L5 S1 disc bulge treatment. Avoid heavy lifting, high-impact workouts, and deep bending movements. Yes, with ergonomic adjustments and limited sitting time. If pain persists, worsens, or causes numbness/weakness. Conclusion: Choosing the Right L5 S1 Disc Bulge Treatment The right L5 S1 disc bulge treatment can make a significant difference in your recovery journey. Most people improve without surgery, but only if they take early action. Ignoring symptoms, poor posture, and delayed treatment can prolong pain and complications. A structured approach that includes physiotherapy, lifestyle changes, and medical guidance is key.
L5 S1 Disc Bulge Recovery Time: How Long Does It Really Take?

L5 S1 Disc Bulge Recovery Time: How Long Does It Really Take? Lower back pain that radiates down your leg, often seen in L5 S1 disc bulge symptoms can be alarming, especially when diagnosed as an L5 S1 disc bulge. One of the first questions most people ask is: “How long will it take to recover?” The truth is, L5 S1 disc bulge recovery time varies depending on severity, lifestyle, and treatment approach. While some recover within weeks, others may take months if the condition is not managed properly. Starting the right L5 S1 disc bulge treatment early plays a crucial role in speeding up recovery. This guide breaks down realistic timelines, factors affecting healing, and what you can do to speed up recovery safely. Direct Answer: L5 S1 Disc Bulge Recovery Time The average L5 S1 disc bulge recovery time ranges from 4 to 12 weeks with proper treatment such as rest, physiotherapy, and medication. In more severe cases, recovery may take 3 to 6 months, especially if nerve compression or chronic symptoms are present. What is an L5 S1 Disc Bulge? The L5-S1 disc is located between the last lumbar vertebra (L5) and the first sacral vertebra (S1). It bears significant body weight and movement stress, making it highly prone to injury. A disc bulge occurs when the outer layer of the disc weakens and pushes outward, sometimes pressing on nearby nerves like the sciatic nerve. This often leads to common L5 S1 disc bulge symptoms such as leg pain, numbness, and tingling. L5 S1 Disc Bulge Recovery Time: Detailed Timeline Understanding the phases of healing can give clarity on L5 S1 disc bulge recovery time. 1. Acute Phase (0–2 Weeks) Intense pain and inflammation Difficulty sitting, bending, or walking Focus: Rest, pain relief, avoiding strain 2. Subacute Phase (2–6 Weeks) Gradual reduction in pain Improved mobility Start physiotherapy and light exercises 3. Recovery Phase (6–12 Weeks) Significant symptom relief Return to daily activities Strengthening exercises become essential 4. Chronic Phase (3–6 Months) For severe or untreated cases Persistent discomfort or nerve symptoms May require advanced treatment It’s important to avoid movements listed in L5 S1 exercises during this stage. Factors That Affect L5 S1 Disc Bulge Recovery Time Not everyone heals at the same pace. These factors influence L5 S1 disc bulge recovery time: 1. Severity of the Bulge Mild bulge: Faster recovery Severe bulge with nerve compression: Longer duration 2. Age and Overall Health Younger individuals recover faster Chronic conditions can slow healing 3. Lifestyle Habits Sitting for long hours delays recovery Poor posture worsens symptoms 4. Treatment Approach Early physiotherapy speeds up healing Ignoring symptoms prolongs recovery Similar recovery strategies are also used in L4-L5 disc bulge treatment without surgery. Symptoms That Indicate Recovery Progress Signs that your L5 S1 disc bulge recovery time is on track: Reduced lower back pain Less leg pain (sciatica) Improved flexibility Better posture tolerance Treatment Options to Reduce Recovery Time Conservative Treatment (First Line) Physiotherapy Anti-inflammatory medications Heat/ice therapy Activity modification Advanced Treatments (If Needed) Epidural steroid injections Chiropractic care (with caution) Surgery (rare cases) Comparison: Fast vs Delayed Recovery Factor Faster Recovery Delayed Recovery Activity Active rehab Bed rest only Posture Correct posture Poor posture Treatment Early physiotherapy Delayed treatment Lifestyle Healthy weight Sedentary lifestyle Real-World Example Case 1: A 32-year-old office worker starts physiotherapy within 1 week → recovers in 6 weeks Case 2: A 45-year-old ignores symptoms for 2 months → recovery takes 4–5 months This shows how early action directly impacts L5 S1 disc bulge recovery time. Step-by-Step Recovery Plan Step 1: Initial Rest (First Few Days) Avoid heavy lifting and prolonged sitting Step 2: Pain Management Use prescribed medication and ice packs Step 3: Start Physiotherapy Focus on core strengthening and flexibility Step 4: Gradual Activity Resume walking and light daily activities Step 5: Long-Term Prevention Maintain posture, weight, and exercise routine Frequently Asked Questions How long does an L5 S1 disc bulge take to heal? The average L5 S1 disc bulge recovery time is 4 to 12 weeks, but severe cases may take up to 6 months. Can an L5 S1 disc bulge heal completely? Yes, many cases heal with conservative treatment, though lifestyle changes are necessary to prevent recurrence. Is walking good for L5 S1 disc bulge? Yes, walking improves blood flow and supports recovery when done in moderation. When should I consider surgery? Surgery is considered only if there is severe nerve compression or no improvement after months of treatment. Can I sit with an L5 S1 disc bulge? Limit sitting time and use proper lumbar support to avoid worsening symptoms. What worsens a disc bulge? Poor posture, heavy lifting, and prolonged sitting can delay recovery. The average L5 S1 disc bulge recovery time is 4 to 12 weeks, but severe cases may take up to 6 months. Yes, many cases heal with conservative treatment, though lifestyle changes are necessary to prevent recurrence. Yes, walking improves blood flow and supports recovery when done in moderation. Surgery is considered only if there is severe nerve compression or no improvement after months of treatment. Limit sitting time and use proper lumbar support to avoid worsening symptoms. Poor posture, heavy lifting, and prolonged sitting can delay recovery. Conclusion: Managing L5 S1 Disc Bulge Recovery Time Effectively Understanding your L5 S1 disc bulge recovery time helps set realistic expectations and avoid panic. Most cases improve within weeks—but only with the right approach. Delaying treatment or ignoring symptoms can extend recovery significantly. Early physiotherapy, proper posture, and guided care make a huge difference. If symptoms persist, consulting experienced professionals such as top spine surgeons in Mumbai can help guide the next steps.
मणक्यातील गॅप लक्षणे

मणक्यातील गॅप लक्षणे मणक्यातील गॅप लक्षणे: कधी डॉक्टरांकडे जावे आणि योग्य उपचार काय आहेत? मणक्यातील गॅप लक्षणे ही अनेक लोकांमध्ये दिसणारी पण अनेकदा दुर्लक्षित राहणारी समस्या आहे. मणक्याच्या हाडांमधील डिस्क किंवा अंतर कमी झाल्यास मणक्यावर ताण येतो आणि नसांवर दबाव पडू शकतो. यामुळे मानदुखी, कंबरदुखी, पाठदुखी किंवा पाय सुन्न होणे यांसारख्या समस्या निर्माण होऊ शकतात. आजकाल दीर्घकाळ बसून काम करणे, चुकीचा पोश्चर, जड वजन उचलणे किंवा वयानुसार होणारी झीज यामुळे ही समस्या अधिक प्रमाणात दिसते. सुरुवातीच्या टप्प्यात योग्य काळजी घेतल्यास वेदना कमी होऊ शकतात आणि गंभीर समस्या टाळता येऊ शकतात. या लेखात आपण मणक्यातील गॅपची लक्षणे, डॉक्टरांकडे कधी जावे, तपासणी, उपचार आणि पुनर्वसन याबद्दल माहिती पाहणार आहोत. मणक्यातील गॅपची सुरुवातीची लक्षणे मणक्यातील गॅपची लक्षणे सुरुवातीला हलकी असू शकतात. पण वेळेवर लक्ष न दिल्यास वेदना वाढू शकतात. सामान्य लक्षणे: मान, पाठ किंवा कंबर दुखणे सकाळी उठल्यावर stiffness जाणवणे पाय किंवा हातामध्ये झिणझिण्या येणे बसताना किंवा वाकताना वेदना वाढणे चालताना किंवा उभे राहताना त्रास मान किंवा कंबर हलवताना कटकट आवाज जाणवणे मांसपेशींमध्ये कमजोरी काही लोकांमध्ये वेदना हळूहळू वाढतात आणि दैनंदिन कामांवर परिणाम होऊ लागतो. ही लक्षणे दिसल्यास मानदुखीची सुरुवातीची लक्षणे तपासा ही लक्षणे दिसल्यास त्वरित डॉक्टरांचा सल्ला घ्या काही परिस्थितींमध्ये त्वरित स्पाईन स्पेशालिस्टचा सल्ला घेणे आवश्यक असते. खालील लक्षणे गंभीर असू शकतात: पाय किंवा हात पूर्णपणे सुन्न होणे चालताना संतुलन बिघडणे मांसपेशींमध्ये कमजोरी वाढणे सतत २–३ आठवडे वेदना राहणे पाठीमध्ये तीव्र वेदना होणे बसणे किंवा उभे राहणे कठीण होणे अशा लक्षणांकडे दुर्लक्ष केल्यास समस्या वाढू शकते, त्यामुळे वेळेवर तपासणी करणे महत्त्वाचे आहे. मणक्यातील गॅपची तपासणी कशी केली जाते? योग्य निदानासाठी डॉक्टर काही तपासण्या सुचवू शकतात. शारीरिक तपासणी: डॉक्टर मणक्याची हालचाल, वेदना आणि स्नायूंची ताकद तपासतात. एक्स-रे: मणक्याच्या हाडांमधील अंतर कमी झाले आहे का हे तपासण्यासाठी एक्स-रे केला जातो. MRI स्कॅन: डिस्कची अवस्था, नसांवर दबाव आणि मऊ पेशींची स्थिती तपासण्यासाठी MRI उपयोगी असतो. नर्व टेस्ट: हात किंवा पायामध्ये सुन्नपणा किंवा कमजोरी आहे का हे तपासण्यासाठी नर्व टेस्ट केली जाते. मणक्यातील गॅपचे आधुनिक उपचार मणक्यातील गॅपच्या उपचारांमध्ये वेदनेची तीव्रता आणि समस्या किती गंभीर आहे यानुसार उपचार ठरवले जातात. 1. औषधोपचार: हलकी ते मध्यम वेदना कमी करण्यासाठी वेदनाशामक औषधे दिली जातात. सूज आणि स्नायूंचा ताण कमी करण्यासाठीही काही औषधे वापरली जाऊ शकतात. 2. फिजिओथेरपी: फिजिओथेरपी हा मणक्याच्या समस्यांसाठी अत्यंत महत्त्वाचा उपचार आहे. योग्य व्यायामामुळे मणक्याभोवतीचे स्नायू मजबूत होतात आणि वेदना कमी होतात. 3. स्पाईन इंजेक्शन: काही प्रकरणांमध्ये सूज कमी करण्यासाठी किंवा नसांवरील दबाव कमी करण्यासाठी विशेष इंजेक्शन उपचार दिले जाऊ शकतात. 4. सर्जरी: जर औषधे आणि फिजिओथेरपीने आराम मिळत नसेल किंवा नसांवर गंभीर दबाव असेल तर सर्जरीचा पर्याय विचारात घेतला जाऊ शकतो. आधुनिक तंत्रज्ञानामुळे आजकाल मिनिमली इन्वेसिव सर्जरीद्वारे कमी वेळेत उपचार करता येतात. जर औषधोपचार व फिजिओथेरपीने आराम मिळत नसेल तर L4-L5 डिस्क बूल्ज उपचार] (l4-l5-disc-bulge-treatment) कडे लक्ष द्या. फिजिओथेरपी आणि व्यायाम योग्य व्यायाम केल्यास मणक्याची लवचिकता आणि ताकद वाढते. उपयुक्त व्यायाम: हलके स्ट्रेचिंग मान आणि खांद्यांचे व्यायाम कंबर मजबूत करणारे व्यायाम योगासह मानसंबंधी योगा सत्र देखील फायद्याचे ठरतात. चालणे आणि हलकी हालचाल हे व्यायाम तज्ज्ञांच्या मार्गदर्शनाखाली करणे सुरक्षित असते. या व्यायामासोबत तुम्ही सर्वसामान्य सर्पिकल स्पॉन्डिलोसिस व्यायाम देखील करू शकता. मणक्याचे आरोग्य सुधारण्यासाठी काही सवयी दैनंदिन जीवनातील काही सवयी बदलल्यास मणक्यावरचा ताण कमी करता येतो. दीर्घकाळ बसणे टाळा योग्य पोश्चर ठेवून बसा नियमित चालणे किंवा व्यायाम करा जड वजन उचलताना योग्य पद्धत वापरा वजन नियंत्रणात ठेवा योग्य गादी आणि उशी वापरा या सवयींमुळे मणक्याच्या समस्या टाळण्यास मदत होऊ शकते. योग्य पोश्चरसह स्पाइन फ्रेंडली डायट अवलंबल्यास फायदा होतो. मणक्यातील गॅपमधून बरे होण्यासाठी किती वेळ लागतो? उपचाराचा कालावधी समस्या किती गंभीर आहे यावर अवलंबून असतो. हलक्या समस्यांमध्ये काही आठवड्यांत आराम मिळू शकतो फिजिओथेरपी केल्यास पुनर्वसन लवकर होऊ शकते गंभीर प्रकरणांमध्ये अधिक वेळ लागू शकतो योग्य उपचार आणि नियमित व्यायाम केल्यास बहुतेक रुग्णांना चांगला आराम मिळतो. मणक्यातील गॅप लक्षणे: वारंवार विचारले जाणारे प्रश्न मणक्याची झीज भरून काढण्यासाठी काय उपाय आहेत? मणक्याची झीज पूर्णपणे भरून काढणे शक्य नसले तरी योग्य उपचारांमुळे वेदना कमी करता येतात. फिजिओथेरपी, नियमित व्यायाम, योग्य पोश्चर आणि डॉक्टरांनी दिलेली औषधे यामुळे मणक्याची ताकद वाढते आणि समस्या नियंत्रणात ठेवता येते. मानेच्या मणक्यातील गॅपची लक्षणे काय आहेत? मानेच्या मणक्यातील गॅप असल्यास मानदुखी, खांद्यामध्ये वेदना, हातामध्ये झिणझिण्या किंवा मुंग्या येणे, मान हलवताना त्रास आणि stiffness जाणवू शकतो. काही वेळा हातामध्ये कमजोरीही जाणवू शकते. मणक्यात गॅप कशामुळे होतो? मणक्यातील गॅप प्रामुख्याने वयानुसार होणारी झीज, चुकीचा पोश्चर, दीर्घकाळ बसून काम करणे, जड वजन उचलणे किंवा मणक्याला झालेल्या दुखापतीमुळे निर्माण होतो. मानदुखीपासून मुक्त होण्यासाठी कोणते घरगुती उपाय आहेत? मानदुखी कमी करण्यासाठी गरम पाण्याची पट्टी लावणे, हलके स्ट्रेचिंग करणे, योग्य पोश्चर ठेवणे आणि दीर्घकाळ मोबाईल किंवा संगणक वापरणे टाळणे उपयुक्त ठरू शकते. मुंग्या होऊ नये म्हणून काय करावे? हात किंवा पायामध्ये मुंग्या येत असल्यास नियमित व्यायाम, रक्ताभिसरण सुधारण्यासाठी चालणे, योग्य पोश्चर ठेवणे आणि दीर्घकाळ एकाच स्थितीत बसणे टाळणे महत्त्वाचे आहे. समस्या सतत राहिल्यास डॉक्टरांचा सल्ला घ्यावा. मान दुखण्याची कारणे काय आहेत? मान दुखण्याची कारणे अनेक असू शकतात जसे की चुकीचा पोश्चर, दीर्घकाळ मोबाईल किंवा संगणक वापरणे, स्नायूंचा ताण, मणक्याची झीज किंवा मानेच्या मणक्यातील गॅप. मणक्याच्या आजारासाठी काय करावे? मणक्याच्या आजारासाठी योग्य निदान करणे अत्यंत महत्त्वाचे आहे. डॉक्टरांचा सल्ला घेणे, फिजिओथेरपी, व्यायाम आणि जीवनशैलीमध्ये बदल केल्यास मणक्याच्या समस्या नियंत्रणात ठेवता येतात. मणक्याची झीज पूर्णपणे भरून काढणे शक्य नसले तरी योग्य उपचारांमुळे वेदना कमी करता येतात. फिजिओथेरपी, नियमित व्यायाम, योग्य पोश्चर आणि डॉक्टरांनी दिलेली औषधे यामुळे मणक्याची ताकद वाढते आणि समस्या नियंत्रणात ठेवता येते. मानेच्या मणक्यातील गॅप असल्यास मानदुखी, खांद्यामध्ये वेदना, हातामध्ये झिणझिण्या किंवा मुंग्या येणे, मान हलवताना त्रास आणि stiffness जाणवू शकतो. काही वेळा हातामध्ये कमजोरीही जाणवू शकते. मणक्यातील गॅप प्रामुख्याने वयानुसार होणारी झीज, चुकीचा पोश्चर, दीर्घकाळ बसून काम करणे, जड वजन उचलणे किंवा मणक्याला झालेल्या दुखापतीमुळे निर्माण होतो. मानदुखी कमी करण्यासाठी गरम पाण्याची पट्टी लावणे, हलके स्ट्रेचिंग करणे, योग्य पोश्चर ठेवणे आणि दीर्घकाळ मोबाईल किंवा संगणक वापरणे टाळणे उपयुक्त ठरू शकते. हात किंवा पायामध्ये मुंग्या येत असल्यास नियमित व्यायाम, रक्ताभिसरण सुधारण्यासाठी चालणे, योग्य पोश्चर ठेवणे आणि दीर्घकाळ एकाच स्थितीत बसणे टाळणे महत्त्वाचे आहे. समस्या सतत राहिल्यास डॉक्टरांचा सल्ला घ्यावा. मान दुखण्याची कारणे अनेक असू शकतात जसे की चुकीचा पोश्चर, दीर्घकाळ मोबाईल किंवा संगणक वापरणे, स्नायूंचा ताण, मणक्याची झीज किंवा मानेच्या मणक्यातील गॅप. मणक्याच्या आजारासाठी योग्य निदान करणे अत्यंत महत्त्वाचे आहे. डॉक्टरांचा सल्ला घेणे, फिजिओथेरपी, व्यायाम आणि जीवनशैलीमध्ये बदल केल्यास मणक्याच्या समस्या नियंत्रणात ठेवता येतात. निष्कर्ष मणक्यातील गॅप लक्षणे सुरुवातीला हलकी असली तरी वेळेवर लक्ष न दिल्यास समस्या वाढू शकते. मानदुखी,
Can Cervical Spondylosis Cause Dizziness?

Can Cervical Spondylosis Cause Dizziness? If you’ve been experiencing unexplained dizziness alongside neck pain or stiffness, you may be wondering: can cervical spondylosis cause dizziness? The short answer is yes — and understanding why can help you take the right steps toward relief. This comprehensive guide explores the connection between cervical spondylosis and dizziness, its symptoms, causes, diagnosis, and treatment options. What Is Cervical Spondylosis? Cervical spondylosis is a degenerative condition of the cervical spine — the seven vertebrae that make up your neck. It is primarily caused by age-related wear and tear on the spinal discs, joints, and ligaments. Over time, the discs lose moisture and elasticity, bone spurs may develop, and the spaces between vertebrae can narrow, a condition known as cervical stenosis. According to medical estimates, more than 85% of people over the age of 60 show some degree of cervical spondylosis on imaging scans, though not all experience symptoms. Common symptoms of cervical spondylosis include: Chronic neck pain and stiffness Headaches originating at the base of the skull Tingling or numbness in the arms and hands Muscle weakness in the upper limbs Dizziness and balance problems Can Cervical Spondylosis Cause Dizziness? The Science Behind It Yes, cervical spondylosis can cause dizziness, and this is more common than many people realize. The medical term often used for this phenomenon is cervicogenic dizziness (CGD) — dizziness that originates directly from the cervical spine rather than the inner ear or brain. Here’s how the mechanism works: Compression of Vertebral Arteries The vertebral arteries run through small openings (foramina transversaria) in the cervical vertebrae and supply blood to the brainstem and cerebellum — the parts of your brain responsible for balance and coordination. When bone spurs or degenerated discs compress these arteries, blood flow is reduced, triggering dizziness or vertigo. This condition is known as vertebrobasilar insufficiency. Irritation of Cervical Nerves The cervical spine houses a dense network of proprioceptive nerve receptors that send positional signals to the brain. When cervical spondylosis irritates these nerves — through inflammation, compression, or mechanical disruption — it sends faulty signals to the brain, creating a sensation of imbalance or spinning. Muscle Spasms and Trigger Points Tight, spasming neck muscles caused by cervical spondylosis can restrict blood flow and nerve signaling, contributing to cervicogenic dizziness. Trigger points in the suboccipital muscles at the base of the skull are frequently implicated in both headaches and dizziness. Sympathetic Nerve Irritation Irritation of the sympathetic nerve fibers in the cervical spine can affect the vascular tone of blood vessels in the inner ear, indirectly causing balance disturbances — a mechanism referred to as cervical sympathetic syndrome. Cervical Spondylosis Dizziness: Key Symptoms to Watch For If you’re asking whether cervical spondylosis is causing your dizziness, look for these associated symptoms that typically accompany cervicogenic dizziness: Symptom Description Neck-triggered dizziness Dizziness that worsens with neck movement or certain head positions Occipital headaches Pain at the back of the head, often radiating forward Nausea Accompanying the dizziness, especially during movement Visual disturbances Blurred vision or difficulty focusing Tinnitus Ringing in the ears Drop attacks Sudden falls without loss of consciousness (rare) Upper limb symptoms Tingling, numbness, or weakness in arms/hands A defining characteristic of cervicogenic dizziness is that it is positional — it often worsens when turning the head, looking up, or holding a fixed posture for a prolonged period. How Is Cervical Spondylosis-Related Dizziness Diagnosed? Diagnosing whether cervical spondylosis can be causing your dizziness requires a multi-step evaluation, as many conditions can present similarly (e.g., BPPV, Meniere’s disease, vestibular neuritis). Diagnostic Tools Include: Physical Examination Your doctor will assess your neck’s range of motion, check for tenderness, and perform neurological tests. The Spurling’s test (applying pressure to the top of the head while rotating the neck) can help identify nerve compression. Imaging Studies X-rays — reveal bone spurs, disc narrowing, and vertebral alignment MRI scans — show soft tissue compression of nerves and the spinal cord CT scans — provide detailed bone structure imaging Doppler Ultrasound Used to assess vertebral artery blood flow and detect compression or insufficiency. Vestibular Function Tests To rule out inner-ear causes of dizziness such as BPPV or Meniere’s disease. Dix-Hallpike Test Helps distinguish between cervicogenic dizziness and benign paroxysmal positional vertigo (BPPV). Treatment Options for Cervical Spondylosis-Induced Dizziness The good news: cervical spondylosis causing dizziness is treatable, and most patients achieve significant relief through conservative (non-surgical) approaches. Physical Therapy Targeted physiotherapy is the cornerstone of treatment for cervicogenic dizziness. A skilled therapist will work on: Cervical stabilization exercises Postural correction Vestibular rehabilitation therapy (VRT) Manual therapy and soft-tissue mobilization Strengthening deep neck flexor muscles Medications NSAIDs (ibuprofen, naproxen) — reduce inflammation and pain Muscle relaxants — relieve cervical muscle spasms Neuropathic agents (gabapentin, pregabalin) — address nerve-related symptoms Betahistine — sometimes prescribed when there is a vascular component to the dizziness Cervical Collar or Traction Short-term use of a soft cervical collar reduces neck movement and pressure. Cervical traction gently decompresses the spine and is often used in physical therapy settings. Lifestyle Modifications Ergonomic workstation setup to reduce neck strain Avoiding prolonged screen time without breaks Using a supportive, orthopedic pillow Quitting smoking (smoking accelerates disc degeneration) Staying well-hydrated to support disc health Interventional Procedures For moderate-to-severe cases: Cervical epidural steroid injections — reduce inflammation around compressed nerves Facet joint injections — target inflamed spinal joints Nerve blocks — provide targeted pain and symptom relief Surgery Surgery is considered only when conservative treatments fail and there is significant spinal cord or nerve compression. Procedures include anterior cervical discectomy and fusion (ACDF) or cervical laminoplasty, both of which aim to decompress the affected structures. Can Cervical Spondylosis Cause Dizziness That Is Permanent? This is a concern many patients have. In most cases, cervicogenic dizziness is not permanent when appropriately treated. However, if the underlying cervical spondylosis is left unmanaged for an extended period — particularly if there is significant vascular or cord compression — dizziness can become chronic. Early intervention dramatically improves outcomes and
Difference Between Spondylosis and Spondylitis
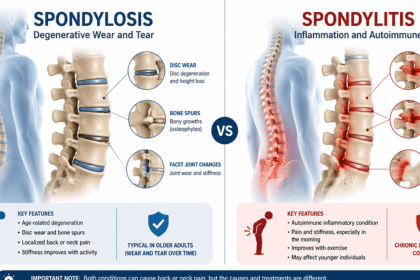
Difference Between Spondylosis and Spondylitis Back pain is one of the most common health complaints today, but not all spine conditions are the same. Many people confuse spondylosis with spondylitis, assuming they’re identical. This misunderstanding can delay proper treatment and worsen symptoms over time. While cervical spine issues like cervical spondylosis affect the neck, lumbar problems such as disc bulges impact the lower back. If you’ve ever wondered about the difference between spondylosis and spondylitis, this detailed guide will help you understand both conditions clearly, so you can make informed decisions about your spine health. The difference between spondylosis and spondylitis lies in their cause and nature. Spondylosis is a degenerative condition caused by age-related wear and tear of the spine, while spondylitis is an inflammatory condition, often autoimmune, that causes pain and stiffness in the spine. What is Spondylosis? Spondylosis refers to the gradual degeneration of the spine due to aging. It commonly affects the cervical (neck) and lumbar (lower back) regions. Key Characteristics of Spondylosis: Caused by wear and tear of discs and joints Common after age 40 Leads to disc degeneration, bone spurs, and stiffness Usually progresses slowly Common Types: Cervical spondylosis (neck) Lumbar spondylosis (lower back) Thoracic spondylosis (mid-back, less common) Symptoms: Chronic neck or back pain Stiffness, especially in the morning Reduced flexibility Nerve compression (in severe cases) What is Spondylitis? Spondylitis is a group of inflammatory diseases affecting the spine. The most common type is ankylosing spondylitis, an autoimmune condition. For those experiencing neck-related symptoms, guided routines like cervical spondylosis exercises can help improve flexibility and reduce stiffness. Key Characteristics of Spondylitis: Caused by inflammation and immune system dysfunction Often starts in younger adults (20–40 years) Can lead to fusion of spinal bones (ankylosis) Systemic condition (can affect eyes, heart, joints) Symptoms: Persistent lower back pain Morning stiffness lasting more than 30 minutes Pain improves with activity (not rest) Fatigue and inflammation If you notice early warning signs such as stiffness or recurring pain, it’s important to understand the early signs of cervical spondylosis before the condition progresses. Difference Between Spondylosis and Spondylitis (Detailed Comparison Table) Feature Spondylosis Spondylitis Nature Degenerative Inflammatory Cause Aging, wear and tear Autoimmune response Age Group Usually 40+ Often 20–40 Progression Slow degeneration Progressive inflammation Pain Pattern Worse with activity Improves with activity Affected Areas Spine discs and joints Spine + other body systems Severity Mild to severe Can become disabling Treatment Physiotherapy, lifestyle Medication + long-term care This table simplifies the difference between spondylosis and spondylitis, helping patients and caregivers identify symptoms early. Key Causes: Spondylosis vs Spondylitis Causes of Spondylosis: Aging and disc dehydration Poor posture Sedentary lifestyle Repetitive strain Obesity Causes of Spondylitis: Genetic factors (HLA-B27 gene) Immune system dysfunction Chronic inflammation Understanding the difference between spondylosis and spondylitis at the root level helps in choosing the right treatment approach. Symptoms Comparison: How to Tell the Difference Spondylosis Symptoms: Pain worsens with movement Localized discomfort Occasional nerve pain Spondylitis Symptoms: Pain improves with exercise Morning stiffness Inflammation in other joints Eye inflammation (uveitis) Diagnosis: How Doctors Differentiate Between the Two Correct diagnosis is crucial when evaluating the difference between spondylosis and spondylitis. For Spondylosis: X-rays (disc degeneration) MRI (nerve compression) Physical examination For Spondylitis: Blood tests (HLA-B27 marker) MRI for inflammation Inflammatory markers (CRP, ESR) Treatment Options for Spondylosis And Spondylitis Spondylosis Treatment: Physiotherapy Pain relievers Posture correction Lifestyle changes Surgery (in severe cases) Spondylitis Treatment: Anti-inflammatory drugs (NSAIDs) Biologic medications Regular exercise Long-term disease management In many cases, combining physiotherapy with practices like yoga for cervical spondylosis can significantly improve mobility and reduce long-term discomfort. Many patients also look for long-term solutions, including guides on how to cure cervical spondylosis permanently, which focus on sustained lifestyle and therapy-based recovery. Real-World Example Consider two patients: Patient A (Age 50): Experiences neck stiffness and pain after long working hours. Diagnosis: Cervical spondylosis. Patient B (Age 28): Has severe morning stiffness that improves after exercise. Diagnosis: Ankylosing spondylitis. This real-life contrast highlights the practical difference between spondylosis and spondylitis. Step-by-Step: What To Do If You Have Back Pain Track your symptoms (timing, intensity, triggers) Check pain patterns (activity vs rest) Consult a spine specialist Get imaging or blood tests if advised Follow a personalized treatment plan Tools & Platforms for Spine Health Posture correction apps (e.g. Spine Health Assessment tools) Wearable fitness trackers Ergonomic chairs and standing desks Physiotherapy programs Conclusion: Understanding the Difference Between Spondylosis and Spondylitis Understanding the difference between spondylosis and spondylitis is essential for accurate diagnosis and effective treatment. While one is a natural part of aging, the other is a serious inflammatory condition that requires long-term care. Ignoring symptoms or self-diagnosing can lead to complications. If you’re experiencing persistent back pain, stiffness, or unusual symptoms, it’s important to seek expert guidance. Early intervention can protect your spine and improve your quality of life. If needed, consult a qualified spine specialist to get a personalized treatment plan tailored to your condition. Frequently Asked Questions What is the main difference between spondylosis and spondylitis? The main difference between spondylosis and spondylitis is that spondylosis is age-related degeneration, while spondylitis is an inflammatory autoimmune condition affecting the spine. Is spondylitis more serious than spondylosis? Yes, spondylitis can be more serious because it is progressive and may lead to spinal fusion if untreated, whereas spondylosis is typically manageable with lifestyle changes. Can spondylosis turn into spondylitis? No, these are separate conditions. The difference between spondylosis and spondylitis lies in their causes, degenerative vs inflammatory, so one does not turn into the other. What is the best treatment for spondylosis? Treatment includes physiotherapy, posture correction, and pain management depending on severity. Can exercise help both conditions? Yes, exercise is beneficial, but it plays a more critical role in managing spondylitis. Which doctor should I consult? You can also explore options with experienced specialists such as the top spine surgeons in Mumbai for advanced diagnosis and treatment. The main difference between spondylosis and spondylitis is that spondylosis is age-related
Spine Specialist in Thane: Your Guide to Expert Care

Spine Specialist in Thane: Your Guide to Expert Care Do you or your loved one experience chronic back pain, neck pain, or spinal disorders? Getting the proper spine specialist in Thane or choosing the right Spine Clinic can be the key to a successful journey towards recovery. can be the key to a successful journey towards recovery. Spine health is vital for overall health, and early intervention helps in avoiding complications. In this guide, we are going to discuss everything you need to know about spine specialists in Thane, their specialty, and how to select the finest care for your spine health. Understanding Spine Specialists: Who Are They? A spine specialist is a medical practitioner qualified to diagnose, treat, and manage different spinal disorders. The professionals may be orthopaedic surgeons, neurosurgeons, physiotherapists, or pain management physicians who specialize in spine issues. They employ advanced medical technology to address ailments such as: Herniated discs Sciatica Scoliosis Spinal stenosis Chronic back and neck pain Spinal injuries and fractures Degenerative disc disease Why You Need a Spine Specialist Spinal problems can drastically affect your daily life, hindering mobility, posture, and overall well-being. A specialist physician will offer a thorough diagnosis, customized treatment protocols, and, if required, surgical procedures. Early visits to a spine specialist ensure that you: Accurate diagnosis through imaging and clinical evaluation Minimally invasive treatment options Effective pain management Faster recovery and rehabilitation Preventing long-term complications Services Offered by Spine Specialists in Thane 1. Diagnosis Thane spine experts provide precise diagnoses of spine issues like herniated discs, scoliosis, and spinal stenosis through sophisticated imaging methods like MRI or CT scans. 2. Non-Surgical Treatments Choices that are not surgical include physical therapy, pain medication, and procedures like epidurals and nerve blocks, which are commonly described as minimally invasive treatment options. The objectives of such procedures are pain management and improvement of physical mobility. 3. Surgical Interventions Spine specialists would turn to spinal surgery like spinal fusion, disc replacement, or endoscopic spine surgery whenever surgery would best benefit the quality of life for patients. 4. Rehabilitation Post-therapeutic rehabilitation will assist in regaining strength and mobility. Individualized treatment schedules and exercise routines are formulated to enhance flexibility and increase muscle strength for rapid recovery. Why Choose We Are Spine? At We Are Spine, we are dedicated to providing world-class spine care with a patient-first approach. Here’s why you should choose us: 1. Expert Team of Spine Specialists Our experts possess great expertise in managing complicated spinal disorders. With a team of orthopaedic surgeons, neurosurgeons, and rehabilitation specialists, we provide holistic spine management. 2. Cutting-Edge Technology and Advanced Treatment Methods We make use of advanced diagnostic equipment and cutting-edge surgery, such as minimally invasive spinal surgery, robotic surgery, and advanced pain treatment therapies. Our state-of-the-art imaging systems and innovative surgeries assist in delivering accurate diagnoses and successful treatments, with little time for recovery and better outcomes for patients. Top Spine Specialists in Mumbai 3. Personalized Patient Care Each patient is provided with a tailored treatment program specific to their individual condition and requirements. We favour non-surgical treatment and lifestyle changes first before resorting to surgery. Each patient is ensured to fully understand their condition and treatment options through our team, which promotes confidence and ease during their recovery process. 4. Holistic and Multidisciplinary Approach Our professionals work closely with physiotherapists, pain management professionals, and rehab specialists to give a well-rounded recovery plan to ensure long-term spinal wellness. We practice treating the cause, not the symptom, and merge several therapeutic methods like chiropractic practice, yoga, and posture correction to foster complete wellness. 5. Proven Success and High Patient Satisfaction We are proud of our excellent success rates and patient success stories. Our care and excellence have earned us the reputation as one of the most reliable names in spine care in Thane. Our patients who undergo treatment at We Are Spine see enhanced mobility, less pain, and a better quality of life, thanks to our devoted staff and patient-friendly services. Our Spine Specialists in Thane Every spine specialist at We Are Spine brings extensive experience and unwavering commitment to patient care. Dr. Priyank M. Patel Dr. Priyank M. Patel is a distinguished orthopaedic spine surgeon practicing in Mumbai and Thane, India, with over 20 years of experience. He specializes in addressing various spinal conditions, including spine tumors, degenerative spine disorders, spinal deformities, fractures, infections, and pain management. His holistic approach emphasizes non-surgical treatments whenever possible before considering surgical interventions. Educational Background Educational Background MBBS: Maharashtra University of Health Sciences (MUHS), Nashik. MS in Orthopedics: Maharashtra University of Health Sciences (MUHS), Nashik. Fellowships: Spinal Deformity Correction Surgery: Royal Orthopaedic Hospital, Birmingham, UK. Minimally Invasive Spine Surgery: Rush University Medical Center, Chicago, USA. Spine Oncology: Rizzoli Orthopaedic Institute, Bologna, Italy. Advanced Spine Fellowship: The Spine Foundation, Mumbai, India. Adult and Pediatric Spinal Deformity Correction Surgery: University of Wales, Cardiff, UK. Spinal Surgery: Robert Jones and Agnes Hunt Hospital, Oswestry, UK. Professional and Clinical Experience Dr. Patel has performed over 3,000 spine surgeries and is affiliated with leading hospitals in Mumbai and Thane. His expertise includes: Minimally Invasive Spine Surgery (MISS): Utilizing small incisions for faster recovery, reduced postoperative pain, and shorter hospital stays. Endoscopic Spine Surgery: Using small cameras and instruments for precise interventions with minimal tissue disruption. Comprehensive Spine Care: Managing a broad range of spinal conditions, including: Degenerative Disc Diseases: Addressing age-related spinal wear and tear. Spinal Deformities: Treating scoliosis, kyphosis, and other structural abnormalities. Spinal Trauma and Fractures: Providing surgical and non-surgical treatment for spinal injuries. Spinal Tumors and Infections: Diagnosing and treating primary, metastatic spine tumors and infections like tuberculosis of the spine. Pain Management and Spine Rehabilitation: Multimodal approaches to treating chronic spinal pain. Awards & Contributions Trustee of Dr. Shekhar Y. Bhojraj’s The Spine Foundation. Official Signatory of TSF for the Rural Spine Care Centres with the Maharashtra Government. Academic Chief Coordinator of The Spine Foundation. Active participation in charitable initiatives, spine health workshops, and free spine camps. Where to Consult Dr. Priyank M. Patel in Thane, Mumbai? Dr. Patel consults at the following hospitals: Jupiter Hospital (Thane West) Address: Eastern Express
Minimally Invasive Spine Surgery: A Modern Solution for Spinal Disorders
Minimally Invasive Spine Surgery: A Modern Solution for Spinal Disorders Minimally Invasive Spine Surgery (MISS) Minimally Invasive Spine Surgery (MISS) is a set of surgical procedures designed to address spinal disorders through smaller incisions than open surgery. The underlying philosophy of MISS is to perform the same operations as open surgery – for example, stabilizing the spine, decompressing nerves, or tumor removal – but with minimal disturbance to surrounding muscles and soft tissues. Here’s a breakdown of key aspects of MISS: How it’s Performed: Smaller Cuts: One or more tiny cuts which are usually smaller than an inch, are made by surgeons. Tubular Retractors: One of the most typical approaches is to pass a stiff, tube-like instrument called a tubular retractor through the tiny cut down to the spine. It establishes a tunnel to the surgical area and opens up the muscles without cutting them. Specialized Equipment: Long and slender instruments that can be used with the tubular retractor or through small cuts. Visualization: Surgeons use the following to visualize the operating site like: Microscope: A magnified view is given by a surgical microscope. Endoscope: A slim tube containing a camera and light source that enables the surgeon to look inside the body on a TV screen. Fluoroscopy (Real-time X-rays): For guiding instrument and implant placement. Computer-Assisted Navigation and Robotics: Can be employed in a few instances to improve accuracy. With these instruments, the surgeon removes degenerated tissues, decompresses nerves or stabilizes the spine while maintaining as much of the normal anatomy as possible. Common MISS Techniques A. Microdiscectomy Purpose: Used for herniated disc removal, relieving pressure on spinal nerves. How it Works: The surgeon removes the damaged portion of the disc pressing against the nerve, reducing pain and numbness. Advantage: Faster recovery as compared to open discectomy. B. Laminectomy/Spinal Decompression Purpose: Treats spinal stenosis (narrowing of the spinal canal). How it Works: A small part of the lamina (vertebral bone) and thickened ligaments is removed to create more space for the nerves. Advantage: Reduces pain, numbness, and weakness in the legs. C. Spinal Fusion (For Stabilization) Purpose: Treats spinal instability, spondylolisthesis, and degenerative disc disease. Types of MISS Fusion Techniques: Transforaminal Lumbar Interbody Fusion (TLIF): Accesses the spine from the back at an angle to minimize muscle damage. Extreme Lateral Interbody Fusion (XLIF) / Direct Lateral Interbody Fusion (DLIF): Accesses the spine from the side, avoiding back muscles altogether. Percutaneous Screw Fixation: Uses small skin incisions to place screws and rods for spinal stability. Advantage: Faster recovery compared to open spinal fusion. D. Vertebroplasty/Kyphoplasty (For Spinal Fractures) Purpose: Used to treat vertebral compression fractures, often caused by osteoporosis or trauma. How it Works: Bone cement is injected into the fractured vertebra to stabilize it and reduce pain. Advantage: Provides immediate pain relief in many cases. E. Endoscopic Spine Surgery Purpose: Used for disc herniations, spinal stenosis, and nerve decompression. How it Works: A tiny endoscope (1 cm or less) is inserted with saline irrigation to improve visibility. Advantage: Minimally invasive, often performed under local anesthesia with faster recovery. Conditions Treated with MISS MISS is suitable for various spinal conditions, including: Herniated discs (bulging disc pressing on nerves) Spinal stenosis (narrowing of the spinal canal) Degenerative disc disease (age-related disc wear and tear) Spondylolisthesis (a vertebra slipping forward) Spinal deformities (such as scoliosis or kyphosis) Spinal tumors (removal of abnormal growths with minimal damage) Vertebral compression fractures (due to osteoporosis) Spinal infections Benefits of MISS In comparison to conventional open spine surgery, MISS has the following benefits: Smaller Scars: Produces one or more small scars rather than one long incision that results in improved cosmetic results. Less Pain After Surgery: Fewer muscle and tissue damages usually mean less postoperative discomfort. Faster Recovery: Patients may have a faster recovery to everyday activities like in some cases within weeks rather than months. Shorter Hospital Stay: Many MISS procedures can be done on an outpatient basis or require a shorter hospital stay ,1-2 days compared to 3-5 days for traditional surgery. Reduced Blood Loss: Smaller incisions and less tissue disruption result in decreased bleeding during surgery. Lower Risk of Infection: Smaller incisions decrease the possibility of points for the entry for bacteria. Reduced Muscle Damage: Steering clear of cutting or considerable retraction of muscles may result in reduced weakness and quicker recovery to usual strength. Reduced Dependence on Pain Medication: As a result of less postoperative pain. Increased Potential Lower Risk of Painkiller Dependency: Because of lower dependence on long-term pain control. Improved Surgical Experience for Some Patients: Could be especially useful for obese, older patients, or patients with chronic pain because of reduced incisions and less physiological stress. Risks of MISS Although MISS has numerous advantages, it is still a surgical procedure and thus has potential risks which are explained below: Infection: Either at the site of the incision or in the surgical wound. Excessive Bleeding: While usually less than open surgery. Nerve Damage: May result in numbness, weakness or other neurological symptoms. The risk is usually lower than with open surgery but it still exists. Blood Clots: Development of blood clots in the legs or lungs. Inadequate Decompression or Fusion: The less invasive technique may not always meet the desired extent of nerve decompression or proper bone fusion (non-union or pseudarthrosis). This complication can be increased in smokers and diabetic patients. Screw Malposition: Where screws are applied for fusion, there is a risk of the screws being mispositioned. Dural Tear: A tear in the dura mater, the membrane that envelops the spinal cord, and can result in cerebrospinal fluid leakage. Need for More Surgery: In case the first surgery fails or complications develop. Persistent Pain: There is a possibility that the surgery might not be able to remove the initial pain or may introduce another kind of pain. Reduced Spinal Flexibility: Fusion, whether it’s open or minimally invasive, can be responsible for loss of some degree of flexibility at the fused area. Surgeons’ Learning Curve: MISS can be technically demanding and takes specialist training and expertise. Important Considerations Not all patients are suitable for MISS. The suitability of MISS on a patient will vary with the spinal
Top 10 Spine Hospitals in Mumbai for Expert Care & Advanced Treatment

Top 10 Spine Hospitals in Mumbai for Expert Care & Advanced Treatment Mumbai, the bustling heart of India, is not just a hub for finance and culture—it’s also a leading center for world-class medical care. When it comes to spine health, the city houses some of the most advanced and trusted spine hospitals in the country. Whether you’re dealing with chronic back pain, slipped discs, scoliosis, or complex spinal disorders, Mumbai offers top-tier facilities backed by cutting-edge technology and globally trained spine specialists. In this comprehensive guide, we’ll take you through the best spine hospitals in Mumbai, what makes them stand out, and how to choose the right one for your needs. If you’re searching for a spine clinic near you, Mumbai offers a wide range of specialized spine centers and expert-led hospitals that provide advanced diagnosis, personalized treatment, and long-term rehabilitation. Why Specialized Spine Care Matters The spine is the central support structure of the body. It plays a vital role in our mobility, posture, and nervous system health. Even minor issues in the spine can lead to significant discomfort and complications. That’s why specialized care is essential. Spine hospitals focus solely on diagnosing, treating, and rehabilitating spinal disorders. They bring together neurosurgeons, orthopaedic surgeons, pain management experts, physiotherapists, and rehabilitation professionals under one roof. These institutions offer advanced diagnostic tools like MRI, CT scans, and digital X-rays, alongside minimally invasive and robotic surgical techniques. What to Look for in a Spine Hospital When selecting a spine hospital in Mumbai, consider the following: Expertise of the medical team: Look for institutions with experienced spine surgeons and specialists. Technology and infrastructure: Modern facilities, including advanced imaging and surgical equipment like MRI, CT scan, digital X-rays, and EMG/nerve studies for accurate diagnosis, make a significant difference. Range of services: From conservative treatment to complex surgeries and post-op rehabilitation. Patient-Centric Care: Transparent treatment plans, affordable packages, and long-term follow-up support. Accessibility and insurance support: Convenient location and cashless facilities can ease the treatment process. Multidisciplinary Approach: Collaboration between pain specialists, neurologists, physiotherapists, and rehabilitation experts. Top 10 Spine Hospitals in Mumbai for Spine Treatment 1. Lilavati Hospital, Bandra (West) Why It’s Trusted – Lilavati Hospital is one of the most renowned multi-specialty hospitals in Mumbai, with more than 20 years of clinical excellence. A hospital with proven consistent medical results, high ethical standards, and individualized attention, it’s a preferred hospital for patients worldwide and across India. Specialties – Spine surgery, neurosurgery, orthopaedics, ICU care, physiotherapy, and post-op rehabilitation. USP – Lilavati is world-famous for its comprehensive spine care—ranging from consultation and diagnosis to surgery and post-rehabilitation care. It boasts some of the best spine experts in India with international reputation. 2. Jaslok Hospital, Peddar Road Jaslok is a historical hospital with a reputation spanning over 50 years, recognized for its emphasis on clinical research, ethical medical procedures, and impeccable infrastructure. Specialties – Spine surgery, neurology, critical care, radiology, and physiotherapy. USP – First in motion-preserving spine surgery and minimally invasive methods. Equipped with advanced MRI/CT scanners and high-tech operating theatres designed to facilitate spinal operations. 3. Wockhardt Hospital, Mumbai Central Why It’s Trusted – The hospital merges technology with human empathy. It belongs to the Wockhardt Group and has attracted international attention with its robotic spine surgery abilities. Specialties – Robotic spine surgery, neuro and ortho spine care, trauma care, and spinal deformity correction. USP – Wockhardt is one among a handful of centers in India to have computer-assisted spinal navigation and intraoperative real-time monitoring, offering improved accuracy for spine surgeries. 4. Saifee Hospital, Charni Road Why It’s Trusted – Saifee has a good reputation for its hygienic, patient-centric infrastructure and expert consultants in various specialties. It provides quality but affordable tertiary care. Specialties – Orthopaedic and spine surgery, general surgery, internal medicine, and diagnostics. USP – It is supported by seasoned surgeons and has customized rehab programs, with special emphasis on conservative care prior to surgery. 5. Breach Candy Hospital, South Mumbai Why It’s Trusted – A top-of-the-line hospital with a reputation for handling VIP patients and adopting strict international standards of quality. It is particularly trusted for complex surgery and risky patients. Specialties – Neurosurgery and spine, cardiology, ICU, and advanced diagnostics. USP – Focused on providing personalized care, Breach Candy offers holistic assistance for complex spine surgery, particularly revisions and spinal deformities. 6. Hiranandani Hospital, Powai Why It’s Trusted – Situated at the center of Powai, this hospital merges world-class infrastructure with community-centric healthcare. It has received several awards for service excellence. Specialties – Orthopaedics, spine surgery, paediatrics, gynaecology, and physiotherapy. USP – It is one of the few hospitals to provide paediatric spine surgery by doctors specifically trained in the treatment of scoliosis and kyphosis in children and adolescents. 7. Global Hospital, Parel Why It’s Trusted – One of the Gleneagles Global chain, this hospital is recognized for organ transplant and upscale surgical facilities. It is an international patients’ hub for specialized treatment. Specialties – Neurosciences, spine surgery, organ transplants, and oncology. USP – The hospital has a reputation for handling complex spine cases, particularly tumor, infection, or multi-level degenerative conditions, with outstanding post-op rehab capabilities. 8. Nanavati Max Super Speciality Hospital, Vile Parle (West) Why It’s Trusted – With a legacy of more than 70 years, Nanavati Max is a renowned institution for cutting-edge treatments and among the biggest private hospitals in Mumbai. Specialties – Spine, neurosurgery, joint replacement, oncology, and internal medicine. USP – Provides real-time robot-assisted guidance, multidisciplinary spine boards, and sophisticated pain management centers. 9. P.D. Hinduja Hospital, Mahim Why It’s Trusted – A name that is equated with ethical care and sustained quality results. Hinduja is NABH and CAP-accredited, reliable over generations. Specialties – Neurosurgery, internal medicine, oncology, nephrology, and spine surgery. USP – Emphasizes evidence-based, conservative care wherever possible and turns to surgery only when necessary—making it a second option center of choice. 10. Kokilaben Dhirubhai Ambani Hospital, Andheri (West) Why It’s Trusted – A state-of-the-art hospital with international standards of healthcare and some of the most sophisticated operation theatres in the nation. Specialties – Robot spine surgery, neurosurgery, oncology, orthopaedics, and critical care. USP – Renowned for its robotic-assisted
Say Goodbye to Pain: Discover the 10 Best Yoga Poses for Cervical Spondylosis Relief!

Yoga Poses for Cervical Spondylosis Cervical spondylosis, or neck arthritis, is a prevalent degenerative disorder of the cervical spine. It arises from the deterioration of cartilage, bones, and spinal discs due to wear and tear, which causes pain, stiffness, and reduced mobility of the neck. Various factors such as poor posture, excessive screen time, lack of physical activity, and age contribute to its development. The good news is that yoga presents a holistic and practical solution for the management of cervical spondylosis. Not only does yoga reduce symptoms, but it also strengthens the neck, shoulders, and spine, which improves quality of life overall. In this comprehensive guide, we’ll explore the benefits of yoga for cervical spondylosis, share the most effective yoga poses, and provide tips to make your practice safe and impactful. What Causes Cervical Spondylosis? Before diving into yoga’s benefits, it’s essential to understand the underlying causes of cervical spondylosis. Common factors include: Poor Posture: Spending hours hunched over a desk or screen puts strain on the neck and shoulders. Prolonged Screen Time: Excessive use of electronic devices contributes to “tech neck,” which is a leading cause of cervical spine issues. Sedentary Lifestyle: Lack of physical activity weakens supporting muscles in the neck and shoulders, increasing stress on the cervical spine. Age-Related Degeneration: Natural aging leads to wear and tear of discs, ligaments, and joints. Injury or Trauma: Whiplash injuries or accidents can accelerate cervical spine degeneration. Recognizing these factors is key to managing cervical spondylosis, and integrating yoga into your routine is a proactive step toward healing. 10 Best Yoga Poses for Cervical Spondylosis Here are the 10 best yoga poses for cervical spondylosis to help you manage pain, restore neck health, and enhance overall well-being. 1. Tadasana (Mountain Pose) Tadasana is a foundational yoga pose that helps improve posture and alignment, reducing strain on the neck. How to Do It: Stand with feet hip-width apart and arms by your side. Engage your core, lengthen your spine, and keep your chin parallel to the ground. Take deep breaths while maintaining this posture for 30 seconds to 1 minute. Benefits: Strengthens neck and shoulder muscles. Improves posture and spinal alignment. Enhances balance, stability, and body awareness. Helps prevent slouching, reducing strain on the cervical spine. 2. Bhujangasana (Cobra Pose) Enhances blood circulation in the neck and shoulders. How to Do It: Lie on your stomach with your legs extended and palms placed under your shoulders. Inhale and lift your chest while keeping your elbows slightly bent. Hold for 15-30 seconds, then slowly release back to the ground. Benefits: Strengthens upper back and neck muscles. Reduces stiffness in the spine and shoulders. Improves blood circulation in the neck and shoulders. Helps counteract the forward-head posture caused by excessive screen use. 3. Marjariasana-Bitilasana (Cat-Cow Pose) This gentle flow between two poses increases flexibility and mobility in the cervical spine. How to Do It: Start in a tabletop position with hands under shoulders and knees under hips. Inhale, arch your back (Cow Pose), lifting your head and chest. Exhale, round your back (Cat Pose), tucking your chin towards your chest. Repeat for 8-10 rounds, synchronizing movement with breath. Benefits: Enhances spinal flexibility and mobility. Relieves tension and stiffness in the neck and shoulders. Encourages better coordination between movement and breath. Boosts circulation to the cervical spine, promoting healing. 4. Balasana (Child’s Pose) Balasana is a relaxing pose that helps release tension in the neck and upper back while promoting deep relaxation. How to Do It: Sit on your heels and extend your arms forward, lowering your forehead to the mat. Breathe deeply, holding for 30 seconds to 1 minute. Relax into the stretch, allowing the spine to lengthen naturally. Benefits: Stretches and relaxes the spine and upper back. Reduces stress and tension in the neck and shoulders. Encourages mindfulness and relaxation, reducing stress-related pain. Improves flexibility in the lower back, complementing cervical spine health. 5. Setu Bandhasana (Bridge Pose) This pose strengthens the back and promotes spinal flexibility, reducing strain on the neck. How to Do It: Lie on your back, bend your knees, and place your feet hip-width apart. Inhale, lift your hips while pressing your feet and shoulders into the ground. Hold for 15-30 seconds, then release. Benefits: Strengthens neck, shoulders, and upper back muscles. Improves spinal alignment and posture. Relieves stress and tension in the cervical spine. It enhances blood circulation to the brain, promoting relaxation. 6. Ardha Matsyendrasana (Half Spinal Twist) A gentle spinal twist that improves mobility and relieves stiffness in the cervical region. How to Do It: Sit with your legs extended and bend your right knee, placing the foot outside the left thigh. Place your right hand behind and twist your torso to the right. Hold for 15-30 seconds, then switch sides. Benefits: Increases spinal flexibility and mobility. Reduces tension in the neck, shoulders, and back. Stimulates the nervous system, promoting relaxation and reducing pain perception. 7. Uttanasana (Standing Forward Bend) This pose stretches the spine and relaxes the neck muscles, reducing stress and stiffness. How to Do It: Stand with feet hip-width apart and slowly bend forward, letting your head hang. Hold onto your elbows and stay for 30 seconds to 1 minute. Benefits: Releases tension in the neck, shoulders, and spine. Enhances blood flow to the head, promoting relaxation. Reduces stress-related neck pain and headaches. 8. Shavasana (Corpse Pose) Shavasana promotes deep relaxation and stress relief, which is crucial for cervical pain management. How to Do It: Lie on your back with arms by your side and palms facing up. Close your eyes, focus on deep breathing, and relax for 5-10 minutes. Benefits: Relaxes the nervous system and reduces chronic pain. Helps release built-up tension in the cervical region. Improves sleep quality, which is essential for healing. 9. Sukhasana with Neck Stretch (Easy Pose) This seated pose combined with gentle neck stretches helps to loosen tension in the cervical spine. How to Do