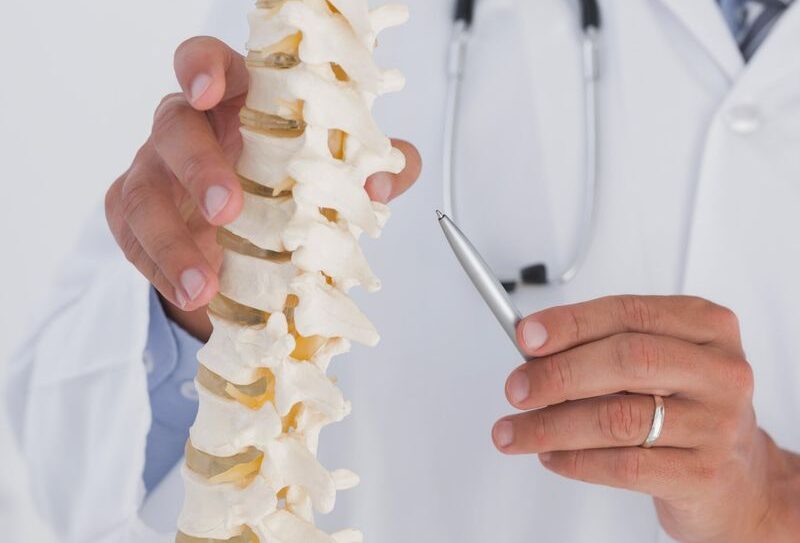
Is Upper Back Pain a Sign of Cancer?
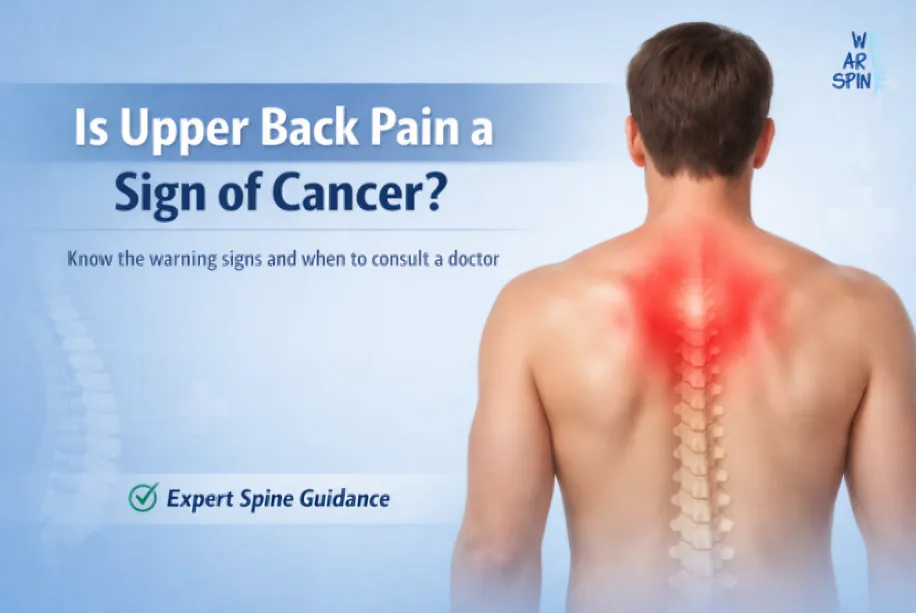
Is Upper Back Pain a Sign of Cancer? When Back Pain Triggers Bigger Fears Upper back pain can be uncomfortable, distracting — and sometimes alarming. If you’ve searched “is upper back pain a sign of cancer?”, you’re likely worried that something serious might be happening.Most upper back pain is NOT caused by cancer. But in rare cases, persistent or unusual back pain can be linked to certain cancers. In this comprehensive guide, we’ll break down: When upper back pain is harmless When it could signal something serious Cancer types associated with back pain Red flag symptoms to watch for When to see a doctor Practical steps you can take right now Let’s separate fear from facts. Understanding Upper Back Pain (Thoracic Spine Pain) The upper back (thoracic spine) runs from the base of your neck to the bottom of your rib cage. It includes: 12 thoracic vertebrae Spinal cord Muscles, ligaments, and ribs Nerves connecting to chest and abdomen Unlike the lower back, the upper back is more stable and less prone to injury — which is why persistent upper back pain deserves attention. Common Causes of Upper Back Pain (Most Are NOT Cancer) Before assuming the worst, understand the most frequent causes related to back pain: 1. Muscle Strain or Poor Posture Especially common in: Desk workers Mobile phone users Drivers Students Symptoms: Aching pain Stiffness Worse with movement Improves with rest 2. Herniated Disc (Thoracic Disc Bulge) Although less common than lumbar disc issues, it can cause: Sharp pain Burning sensation Pain radiating around ribs 3. Arthritis or Degenerative Disc Disease More common after age 50, Signs: Gradual stiffness Morning discomfort Limited mobility 4. Osteoporosis Compression Fracture More common in: Postmenopausal women Elderly individuals Common vs Concerning Upper Back Pain Feature Common Mechanical Pain Possible Serious Cause Duration Improves in days/weeks Persistent >4 weeks Night Pain Rare Common Weight Loss No Unexplained loss Fever No Possible Improves with Rest Yes No Neurological Symptoms Rare Possible So Is Upper Back Pain a Sign of Cancer? The honest answer: Rarely — but it can be. Cancer-related back pain typically occurs when: Cancer spreads (metastasizes) to the spine A tumor presses on spinal nerves Bone cancer affects vertebrae But this accounts for a very small percentage of back pain cases. According to medical research: Less than 1% of primary care back pain cases are due to cancer. In patients without prior cancer history, spinal cancer is extremely rare. (Source: Cancer Centre) Types of Cancer That Can Cause Upper Back Pain 1. Lung Cancer One of the more common cancers associated with upper back pain. Why? Lungs are near the thoracic spine. Tumors may irritate nerves or invade chest wall structures. (Source: Cancer Centre) Other Symptoms: Persistent cough Shortness of breath Chest pain Blood in sputum Fatigue 2. Breast Cancer (Especially in Women) Breast cancer may spread to: Spine Ribs Pelvis Upper back pain could be a symptom of metastasis. Watch for: Breast lump Nipple changes Skin dimpling Swelling 3. Prostate Cancer (In Men) Advanced prostate cancer commonly spreads to bone. Symptoms: Bone pain Difficulty urinating Weak urine stream 4. Multiple Myeloma A cancer of plasma cells affecting bones. Symptoms: Persistent bone pain Fatigue Frequent infections Anemia 5. Spinal Tumors (Primary or Secondary) Rare but possible. Red flags include: Severe night pain Pain not relieved by rest Neurological weakness Warning Signs That Upper Back Pain Could Be Serious Here’s when doctors become concerned: Red Flag Symptoms Pain that wakes you at night Pain not improving after 4–6 weeks Unexplained weight loss Fever or chills History of cancer Progressive weakness Numbness or tingling Loss of bladder or bowel control If you have multiple red flags, seek medical evaluation immediately. How Cancer-Related Back Pain Feels Different Cancer-related pain often: Is deep and constant Does not improve with rest Worsens at night Progressively gets worse May not change with posture Mechanical pain: Improves with stretching Changes with movement Eases with rest When Should You See a Doctor? You should consult a back pain doctor if: Pain lasts more than 3–4 weeks You’re over 50 with new back pain You have a history of cancer Pain is severe and unexplained You experience neurological symptoms Statistical Perspective: Should You Be Worried? Let’s ground this in data. Back pain affects up to 80% of adults at some point. Cancer accounts for <1% of new back pain cases. In patients without red flags, imaging rarely shows cancer. The odds are overwhelmingly in favor of a non-cancer cause. Frequently Asked Questions अक्सर पूछे जाने वाले सवाल How do you treat a posterior disc bulge? Treatment usually includes rest, physiotherapy, posture correction, core strengthening exercises, anti-inflammatory medications, and lifestyle changes. Most cases improve without surgery. Severe nerve compression may require injections or surgical intervention. What is the L4-L5 posterior disc bulge? An L4-L5 posterior disc bulge occurs when the spinal disc between the fourth and fifth lumbar vertebrae protrudes backward, possibly compressing nerves and causing lower back pain, sciatica, or leg numbness. Is disc bulge 100% curable? A disc bulge may not completely reverse anatomically, but symptoms can fully resolve with proper treatment. Many people become pain-free and function normally through physiotherapy, strengthening, and conservative management. Can I live a normal life after disc bulge? Yes, most people live completely normal, active lives after a disc bulge. With regular exercise, posture care, weight management, and medical guidance, symptoms can be controlled effectively. Treatment usually includes rest, physiotherapy, posture correction, core strengthening exercises, anti-inflammatory medications, and lifestyle changes. Most cases improve without surgery. Severe nerve compression may require injections or surgical intervention. An L4-L5 posterior disc bulge occurs when the spinal disc between the fourth and fifth lumbar vertebrae protrudes backward, possibly compressing nerves and causing lower back pain, sciatica, or leg numbness. A disc bulge may not completely reverse anatomically, but symptoms can fully resolve with proper treatment. Many people become pain-free and function normally through physiotherapy, strengthening, and conservative management. Yes, most people live completely normal, active lives after a disc bulge. With regular exercise, posture care, weight management, and medical guidance, symptoms can be controlled effectively. Please enable JavaScript in your browser
Which Doctor to Consult for Back Pain?

Which Doctor to Consult for Back Pain? Back pain is frustrating. But what’s worse?Not knowing which doctor to consult for back pain. Orthopedic? Neurologist? Spine surgeon? Choosing the wrong one can delay diagnosis, prolong pain, and cost you precious time. Here’s the expert-backed clarity you need from Mumbai’s leading spine specialists. Quick Answer: Which Doctor to Consult for Back Pain? Here’s the simplified expert rule: Mild pain (few days to 2 weeks) → General Physician Pain after injury / bone-related issues → Orthopedic Doctor Radiating leg pain / numbness / weakness → Spine Specialist Chronic back pain (6+ weeks) → Spine Specialist Severe neurological symptoms → Urgent spine evaluation Now let’s go deeper. Orthopedic Doctor for Back Pain An orthopedic surgeon specializes in bones, joints, ligaments, and discs. They treat: Slip disc (herniated disc) Degenerative disc disease Spondylosis Spinal arthritis Fractures Scoliosis If your pain worsens with movement and improves with rest, it may be mechanical, often orthopedic in nature. However, not all orthopedic doctors specialize exclusively in spine conditions. That distinction matters. Neurologist for Nerve-Related Back Pain A neurologist treats nerve disorders. See a neurologist if you have: Numbness or tingling in legs Burning sensation Electric shock-like pain Leg weakness Bladder/bowel changes (emergency) These symptoms suggest nerve compression — often caused by a disc pressing on spinal nerves. But in most structured spine centers, a spine specialist evaluates both bone and nerve causes together. What Is a Spine Specialist? A spine specialist is either: An orthopedic spine surgeon OR a neurosurgeon specializing exclusively in spinal disorders Unlike general orthopedics, spine specialists focus only on spinal pathology. They manage: Cervical spine disorders Lumbar disc herniation Sciatica Spinal stenosis Spinal deformities Spine trauma Spine tumors Minimally invasive spine surgery Do You Need a Spine Surgeon? This is the biggest fear patients have. The truth: 90–95% of back pain cases do NOT require surgery. Surgery is considered only when: Pain persists beyond 6–8 weeks There is progressive nerve weakness MRI shows severe compression Conservative treatment fails There is spinal instability Modern minimally invasive spine surgery allows: Smaller incisions Faster recovery Reduced blood loss Early mobility But Spine surgery is always the last option — not the first. When Back Pain Is an Emergency Seek urgent evaluation if you experience: Sudden leg weakness Loss of bladder/bowel control Severe trauma High fever with back pain History of cancer with new back pain These may indicate: Cauda equina syndrome Spinal infection Tumor Fracture Immediate spine specialist evaluation is critical. Doctor Comparison Table Symptoms Best Doctor to Consult Mild muscle strain General Physician Injury-related back pain Orthopedic Doctor Radiating leg pain (Sciatica) Spine Specialist Chronic back pain (6+ weeks) Spine Specialist Numbness + weakness Urgent Spine Evaluation Structural deformity Spine Specialist Why a Dedicated Spine Team Matters Back pain is complex. It may involve: Bones Discs Ligaments Nerves Muscles Alignment A multidisciplinary spine team ensures: Comprehensive diagnosis Non-surgical options explored first Minimally invasive expertise if needed Long-term rehabilitation planning When choosing a spine doctor, look for: At We Are Spine, our team is led by Dr. Shekhar Bhojraj India’s first dedicated spine surgeon, along with internationally fellowship-trained spine surgeons. With over 40 years of collective expertise and 600,000+ patients treated, our focus remains: Patient-centered care Conservative-first approach Minimally invasive techniques Spine treatment at Mumbai’s premier hospitals including Lilavati, Breach Candy & P.D. Hinduja Please enable JavaScript in your browser to complete this form.Please enable JavaScript in your browser to complete this form.Full Name *Email *Phone Number * Submit
डाव्या बाजूच्या पाठदुखीवर उपाय
डाव्या बाजूच्या पाठदुखीवर उपाय आजकाल अनेक लोक डाव्या बाजूच्या पाठदुखीवर उपाय शोधताना दिसतात. बदलती जीवनशैली, सतत बसून काम करणे, मोबाईल-लॅपटॉपचा जास्त वापर, चुकीची पोस्चर आणि व्यायामाचा अभाव यामुळे पाठदुखीची समस्या वाढत आहे. काही वेळा ही वेदना सौम्य असते, तर काही वेळा ती तीव्र होऊन दैनंदिन आयुष्यावर परिणाम करते. या लेखात आपण डाव्या बाजूची पाठदुखी का होते, त्याची लक्षणे कोणती आणि त्यावर कोणते उपाय प्रभावी ठरतात हे सविस्तर समजून घेऊ. डाव्या बाजूची पाठदुखी होण्याची प्रमुख कारणे 1. चुकीची बसण्याची सवय: ऑफिसमध्ये किंवा घरी दीर्घकाळ वाकून बसणे, एकाच बाजूला झुकून काम करणे किंवा पाठ न टेकवता बसल्यामुळे पाठीच्या डाव्या बाजूच्या स्नायूंवर ताण येतो. 2. स्नायू ताण (Muscle Strain): अचानक वजन उचलणे, चुकीच्या पद्धतीने व्यायाम करणे किंवा शरीराची हालचाल अचानक बदलल्याने स्नायू ताणले जातात आणि डाव्या बाजूला वेदना जाणवतात. 3. स्लिप डिस्क: कंबर किंवा पाठीच्या मणक्यांमधील डिस्क बाहेर सरकून नसांवर दाब पडल्यास डाव्या बाजूला तीव्र पाठदुखी होऊ शकते. कधी कधी ही वेदना नितंब किंवा पायापर्यंत पसरते. 4. सायटिका: सायटिक नर्व्हवर दाब आल्यास पाठीतून पायापर्यंत डाव्या बाजूला दुखणे, जळजळ किंवा मुंग्या येण्याची तक्रार होऊ शकते. 5. अंतर्गत अवयवांची समस्या: किडनी स्टोन किंवा किडनी संसर्गामुळेही डाव्या बाजूला पाठीमागे खोल दुखणे जाणवू शकते, विशेषतः वेदना सतत आणि तीव्र असतील तर. डाव्या बाजूच्या पाठदुखीची लक्षणे पाठीत सतत किंवा अधूनमधून होणारे दुखणे वाकताना किंवा सरळ उभे राहताना वेदना वाढणे कंबर कडक होणे पायात मुंग्या येणे किंवा बधिरपणा दीर्घकाळ बसल्यानंतर त्रास वाढणे जर ही लक्षणे अनेक दिवस टिकत असतील, तर डाव्या बाजूच्या पाठदुखीवर उपाय करण्यासाठी वैद्यकीय सल्ला घेणे गरजेचे आहे. डाव्या बाजूच्या पाठदुखीवर घरगुती उपाय 1. गरम पाण्याचा शेक: दुखत असलेल्या भागावर गरम पाण्याची पिशवी ठेवली तर स्नायू सैल होतात आणि वेदना कमी होतात. 2. योग्य विश्रांती: अतिश्रम टाळा, पण पूर्णपणे हालचाल बंद करू नका. हलकी हालचाल रक्तप्रवाह सुधारण्यास मदत करते. 3. सौम्य स्ट्रेचिंग व्यायाम: हलके स्ट्रेचिंग आणि पाठीचे व्यायाम केल्याने स्नायूंवरील ताण कमी होतो. मात्र वेदना जास्त असतील तर व्यायाम टाळावा. 4. योग्य झोपण्याची पद्धत: कडेला झोपताना गुडघ्यांमध्ये उशी ठेवा किंवा पाठ टेकून झोपताना गुडघ्याखाली उशी ठेवल्यास पाठीवरचा ताण कमी होतो. 5. पोस्चर सुधारणे: बसताना पाठ सरळ ठेवा, स्क्रीन डोळ्यांच्या समांतर ठेवा आणि दर ३०–४० मिनिटांनी उठून थोडी हालचाल करा. कधी डॉक्टरांचा सल्ला घ्यावा? वेदना ७–१० दिवसांपेक्षा जास्त टिकत असतील पायात कमजोरी किंवा बधिरपणा जाणवत असेल चालताना त्रास होत असेल वेदनांसोबत ताप किंवा वजन घटणे जाणवत असेल पाठदुखी टाळण्यासाठी काय करावे? नियमित चालणे व व्यायाम वजन नियंत्रणात ठेवणे जड वस्तू उचलताना योग्य पद्धत वापरणे दीर्घकाळ एकाच पोस्चरमध्ये बसणे टाळणे ताणतणाव कमी करणे निष्कर्ष डाव्या बाजूच्या पाठदुखीवर उपाय वेळीच केल्यास गंभीर समस्या टाळता येतात. सुरुवातीच्या टप्प्यात योग्य पोस्चर, घरगुती उपाय आणि जीवनशैलीतील बदल केल्याने बराच आराम मिळू शकतो. मात्र वेदना वाढत असतील किंवा इतर लक्षणांसोबत असतील, तर तज्ञ डॉक्टरांचा सल्ला घेणे अत्यंत आवश्यक आहे. योग्य निदान, उपचार आणि काळजी घेतल्यास पाठदुखीवर नियंत्रण मिळवता येते आणि दैनंदिन जीवन पुन्हा आरामदायी बनवता येते. Please enable JavaScript in your browser to complete this form.Please enable JavaScript in your browser to complete this form.Full Name *Email *Phone Number * Submit
सायटिका क्या है?
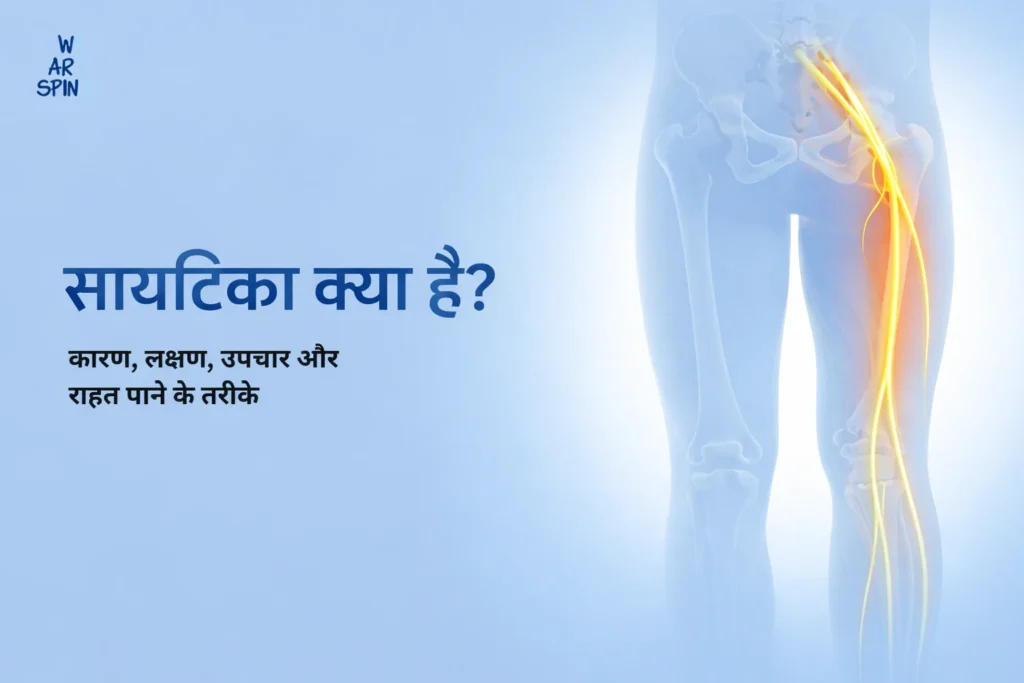
सायटिका क्या है? सायटिका क्या है? कारण, लक्षण, उपचार और राहत पाने के तरीके अगर आप कमर, नितंब या पैर में दर्द महसूस कर रहे हैं, तो आप अकेले नहीं हैं। सायटिका एक सामान्य लेकिन गंभीर समस्या है, जो जीवन की गुणवत्ता को प्रभावित कर सकती है। अच्छी खबर यह है कि सही जानकारी और समय पर उपचार से सायटिका को नियंत्रित किया जा सकता है और आप फिर से सक्रिय जीवन जी सकते हैं। इस ब्लॉग में हम विस्तार से बताएंगे कि सायटिका क्या है, इसके लक्षण, कारण, जांच, उपचार और राहत पाने के आसान उपाय। सायटिका क्या होती है? सायटिका तब होती है जब सायटिक नस पर दबाव पड़ता है। यह नस शरीर की सबसे लंबी नस है और कमर से निकलकर पैरों तक जाती है। दबाव के कारण नस में सूजन, दर्द, झनझनाहट और सुन्नपन महसूस होता है। ध्यान रखें: हर दर्द सायटिका नहीं होता। लेकिन अगर दर्द कमर से लेकर पैर तक फैल रहा है, तो इसे नजरअंदाज न करें सायटिका के कारण सायटिका के होने के कई कारण हैं। मुख्य कारण निम्नलिखित हैं: स्लिप डिस्क (Herniated Disc)डिस्क में चोट या उम्र के कारण परिवर्तन होने पर यह बाहर निकल सकती है और नस पर दबाव डाल सकती है। स्पाइनल स्टेनोसिस (Spinal Stenosis)रीढ़ की हड्डी में नलिका संकरी होने से नसें दब सकती हैं। स्पॉन्डिलोसिस (Spondylosis)उम्र बढ़ने के साथ हड्डियों और डिस्क में बदलाव होता है, जिससे नस पर दबाव पड़ता है। चोट या एक्सीडेंटरीढ़ की चोट या चोटिल बैठने से सायटिका हो सकती है। गलत पोस्चरलंबे समय तक झुककर बैठना या भारी सामान उठाना नसों पर दबाव डाल सकता है। अन्य कारण: मोटापा, वजन अधिक होना, कमर की कमजोरी या शारीरिक कमजोरी भी सायटिका बढ़ा सकती है। सायटिका के लक्षण सायटिका के लक्षण स्पष्ट होते हैं, लेकिन व्यक्ति-व्यक्ति में अलग हो सकते हैं। मुख्य लक्षण हैं: कमर से लेकर नितंब और पैर तक फैलता दर्द एक पैर में ज्यादा दर्द पैर में झनझनाहट या जलन सुन्नपन या कमजोरी लंबे समय तक बैठने या खड़े रहने पर दर्द बढ़ना चलने में या सीढ़ियाँ चढ़ने में कठिनाई अगर ये सायटिका के लक्षण 2–3 हफ्तों से अधिक समय तक बने रहें, तो डॉक्टर से तुरंत सलाह लें। सायटिका का दर्द कितना गंभीर हो सकता है? शुरुआती अवस्था में सायटिका हल्की लग सकती है। लेकिन इलाज न करने पर यह गंभीर रूप ले सकती है।संदर्भित जोखिम: पैरों में स्थायी कमजोरी संतुलन की समस्या पेशाब या शौच पर नियंत्रण की समस्या चिंता न करें। सही इलाज और समय पर निदान से अधिकांश मामलों में पूरी तरह राहत मिलती है। सायटिका की जांच कैसे की जाती है? सायटिका की सही जांच बहुत जरूरी है। आम जांच में शामिल हैं: क्लिनिकल परीक्षण – दर्द और कमजोरी का मूल्यांकन एक्स-रे (X-ray) – हड्डियों की स्थिति देखने के लिए MRI स्कैन – नस और डिस्क की सटीक स्थिति जानने के लिए CT स्कैन – कुछ जटिल मामलों में सही जांच से यह पता चलता है कि सायटिका का कारण क्या है और उपचार किस प्रकार से किया जाए। सायटिका का इलाज सायटिका का इलाज व्यक्ति पर निर्भर करता है। इसे दो मुख्य प्रकारों में बांटा जा सकता है: 1. शस्त्रक्रिया के बिना इलाज शुरुआती अवस्था में सायटिका का इलाज बिना सर्जरी के किया जा सकता है। इसमें शामिल हैं: फिजियोथेरेपी – मांसपेशियों को मजबूत करना दवाइयाँ – दर्द और सूजन कम करने के लिए नर्व ब्लॉक इंजेक्शन – तेज दर्द में राहत के लिए लाइफस्टाइल बदलाव – सही पोस्चर और व्यायाम लगभग 70–80% मरीज बिना सर्जरी के पूरी तरह ठीक हो जाते हैं। 2. सर्जरी कब जरूरी होती है? कुछ मामलों में सायटिका के लिए सर्जरी आवश्यक होती है: दर्द असहनीय हो पैर कमजोर हो रहा हो पेशाब या शौच पर नियंत्रण की समस्या इलाज से आराम न मिलना आजकल मिनिमली इनवेसिव सर्जरी का विकल्प है, जिससे रिकवरी तेज़ होती है और अस्पताल में रहना कम होता है। मिनिमली इनवेसिव सर्जरी के फायदे छोटा चीरा, कम दर्द जल्दी रिकवरी अस्पताल में कम दिन रहना रोज़मर्रा की गतिविधियों में तेजी से वापसी कई मामलों में मरीज 1–2 हफ्तों में सामान्य जीवन जीने लगते हैं। सायटिका से राहत पाने के आसान उपाय (घर पर) लंबे समय तक एक ही स्थिति में न बैठें हल्की स्ट्रेचिंग और योग करें गरम सिकाई से मांसपेशियों को आराम दें भारी सामान उठाने से बचें सही कुर्सी और पोस्चर अपनाएँ छोटे कदम भी दर्द कम करने और सायटिका को नियंत्रित करने में बहुत मदद करते हैं। सायटिका और रोज़मर्रा की जिंदगी सायटिका आपके दैनिक जीवन को प्रभावित कर सकती है। समय पर निदान और सही इलाज से आप: दर्द कम कर सकते हैं पैरों में ताकत और संतुलन बढ़ा सकते हैं फिर से सामान्य जीवन और काम कर सकते हैं चिंता न करें, सही मार्गदर्शन से अधिकांश मरीज पूर्ण स्वस्थ हो जाते हैं। डॉक्टर से कब मिलें? यदि सायटिका का दर्द लगातार बढ़ रहा है या बार-बार हो रहा है, तो स्पाइन विशेषज्ञ से तुरंत मिलें। We Are Spine में अनुभवी स्पाइन विशेषज्ञ आधुनिक तकनीकों से सायटिका का इलाज करते हैं। हम आपकी समस्या को समझते हैं और सुरक्षित, असरदार समाधान प्रदान करते हैं। निष्कर्ष सायटिका आम है, लेकिन डराने वाली नहीं। सही जानकारी, समय पर निदान और उपचार से आप इसे नियंत्रित कर सकते हैं। याद रखें: जल्दी इलाज और सही मार्गदर्शन ही सबसे तेज़ राहत देता है। अक्सर पूछे जाने वाले सवाल साइटिका का सबसे बढ़िया इलाज क्या है? साइटिका का सबसे प्रभावी इलाज उस व्यक्ति की समस्या पर निर्भर करता है। हलके मामलों में योग, स्ट्रेचिंग और फिजियोथेरेपी काफी लाभकारी होते हैं। गंभीर मामलों में मिनिमली इनवेसिव सर्जरी या दर्द निवारक उपचार आवश्यक हो सकते हैं। सही निदान और समय पर उपचार से दर्द में तेजी से राहत मिलती है। साइटिका होने का कारण क्या है? साइटिका तब होती है जब सायटिक नस पर दबाव पड़ता है। इसके मुख्य कारणों में स्लिप डिस्क, रीढ़ की हड्डी में संकुचन (स्पाइनल स्टेनोसिस), उम्र संबंधी बदलाव, चोट या गलत पोस्चर शामिल हैं। अतिरिक्त वजन, कमजोरी और लंबे समय तक बैठे रहना भी साइटिका बढ़ा सकते हैं। साइटिका में क्या खाना चाहिए और क्या नहीं? साइटिका में संतुलित आहार बेहद जरूरी है। प्रोटीन, कैल्शियम, ओमेगा-3 फैटी एसिड और विटामिन डी युक्त भोजन हड्डी और मांसपेशी मजबूत करता है। इसके विपरीत तैलीय, जंक फूड, अत्यधिक चीनी और प्रोसेस्ड फूड से बचना चाहिए। हाइड्रेशन और ताजे फल-सब्ज़ी लेना लाभकारी होता है। साइटिका कितने दिनों में
4 Stages of Disc Herniation

4 Stages of Disc Herniation Disc herniation is a common spinal condition that develops gradually due to degeneration, injury, or repetitive stress on the spine. It occurs when the soft inner portion of an intervertebral disc pushes through or leaks out of its outer layer, potentially irritating nearby nerves. Understanding the 4 stages of disc herniation helps in recognizing early symptoms and taking timely steps to prevent progression. Disc herniation can affect any part of the spine, but it most commonly occurs in the cervical (neck) and lumbar (lower back) regions. What Is Disc Herniation? The spine is made up of vertebrae separated by intervertebral discs, which act as shock absorbers. Each disc has: A soft, gel-like center (nucleus pulposus) A tough outer ring (annulus fibrosus) Disc herniation occurs when the outer ring weakens or tears, allowing the inner material to bulge or leak outward. This process typically progresses through four stages. Here are the 4 stages of disc herniation Stage 1: Disc Degeneration This is the earliest stage and often goes unnoticed. What Happens? Discs lose water content and elasticity Disc height begins to reduce The spine becomes less flexible Common Symptoms Mild back or neck stiffness Occasional discomfort after activity No nerve compression at this stage Degeneration is a natural part of aging but may begin earlier due to poor posture, prolonged sitting, or repetitive strain. Stage 2: Disc Bulge (Prolapse) At this stage, the disc starts to protrude beyond its normal boundary. What Happens? The disc bulges outward The outer layer remains intact No rupture occurs Common Symptoms Localized back or neck pain Muscle tightness Pain that worsens with certain movements A disc bulge may press on nearby tissues but does not always cause nerve symptoms. Stage 3: Disc Herniation (Extrusion) This is the stage most people refer to as a “slipped disc.” What Happens? The outer disc layer tears Inner disc material leaks out Nearby nerves may become compressed Common Symptoms Sharp or radiating pain Numbness or tingling in arms or legs Muscle weakness Pain aggravated by coughing or bending Symptoms vary depending on which nerve is affected. Stage 4: Sequestered Disc (Fragmentation) This is the most advanced stage of disc herniation. What Happens? Disc material breaks off and moves into the spinal canal Inflammation increases Nerve compression may become severe Common Symptoms Persistent or severe nerve pain Significant weakness Reduced reflexes Difficulty with daily activities This stage often requires close medical monitoring. How Disc Herniation Progresses Not everyone experiences all four stages. Many people remain in the early stages and never progress to severe herniation. Progression depends on factors such as: Age Physical activity Body weight Occupation Spinal posture Early intervention can slow or halt progression. Common Causes of Disc Herniation Age-related degeneration Poor posture Prolonged sitting Improper lifting techniques Repetitive bending or twisting Sudden injury or trauma Conclusion Disc herniation is a progressive condition that develops through four stages, from early degeneration to advanced disc fragmentation. While advanced stages can cause significant discomfort and nerve symptoms, many cases can be effectively managed when identified early. Paying attention to back or neck pain and addressing risk factors can help prevent long-term complications. Frequently Asked Questions (FAQs) What Is the Most Painful Stage of Herniation? The most painful stage is usually disc extrusion, where the inner disc pushes through the outer layer, compressing nerves, causing severe lower back pain, sciatica, numbness, and leg weakness. The most painful stage is usually disc extrusion, where the inner disc pushes through the outer layer, compressing nerves, causing severe lower back pain, sciatica, numbness, and leg weakness. Is L4-L5 Herniated Disc Serious? An L4-L5 herniated disc can be serious if it compresses nerves, causing pain, numbness, or weakness. Most cases improve with conservative treatment, but severe compression may require urgent medical care. An L4-L5 herniated disc can be serious if it compresses nerves, causing pain, numbness, or weakness. Most cases improve with conservative treatment, but severe compression may require urgent medical care. Can a Herniated Disc Return to Normal? Many herniated discs can heal naturally over time. With rest, physiotherapy, anti-inflammatory medications, and healthy habits, the disc can shrink, relieve nerve pressure, and reduce pain without surgery. Many herniated discs can heal naturally over time. With rest, physiotherapy, anti-inflammatory medications, and healthy habits, the disc can shrink, relieve nerve pressure, and reduce pain without surgery. What Are the Emergency Symptoms of a Herniated Disc? Emergency symptoms include loss of bladder or bowel control, severe leg weakness, numbness, or sudden extreme back pain. These may indicate nerve compression requiring immediate medical attention. Emergency symptoms include loss of bladder or bowel control, severe leg weakness, numbness, or sudden extreme back pain. These may indicate nerve compression requiring immediate medical attention. What Percentage of Herniated Discs Require Surgery? Only about 10–20% of herniated disc cases need surgery. Most patients recover with conservative treatment like physiotherapy, medications, and lifestyle changes, while surgery is reserved for severe or persistent cases. Only about 10–20% of herniated disc cases need surgery. Most patients recover with conservative treatment like physiotherapy, medications, and lifestyle changes, while surgery is reserved for severe or persistent cases. Please enable JavaScript in your browser to complete this form.Please enable JavaScript in your browser to complete this form.Full Name *Email *Phone Number * Submit
Is Lumbar Spondylosis Serious

Is Lumbar Spondylosis Serious What Is Lumbar Spondylosis? Lumbar spondylosis is a common spinal condition, especially among adults over the age of 40, but it is increasingly being diagnosed in younger individuals due to sedentary lifestyles and poor posture. When people are diagnosed with lumbar spondylosis, one of the first questions they often ask is: Is lumbar spondylosis serious? The answer depends on several factors, including the severity of the condition, symptoms, lifestyle, and how early it is managed. While lumbar spondylosis is not usually life-threatening, it can significantly affect daily life if left untreated. Is Lumbar Spondylosis Serious? Lumbar spondylosis is generally a chronic but manageable condition. In most cases, it is not dangerous, but it can become serious if it leads to nerve compression or spinal instability. Mild to Moderate Cases: Cause intermittent lower back pain or stiffness Symptoms often improve with rest, exercise, and lifestyle changes Usually do not interfere significantly with daily activities Severe or Advanced Cases: May cause nerve-related symptoms Can limit mobility and quality of life May require long-term medical management The seriousness of lumbar spondylosis largely depends on whether it affects nearby nerves or the spinal canal. Common Symptoms of Lumbar Spondylosis Symptoms can vary from person to person and may worsen gradually over time. 1. Lower Back Pain Pain is usually dull and aching, often worse after prolonged sitting, standing, or bending. 2. Morning Stiffness Stiffness in the lower back is common, especially after waking up, and usually improves with movement. 3. Reduced Flexibility Difficulty bending or twisting the lower back may develop as the spine becomes less flexible. 4. Pain Radiating to the Legs If nerves are affected, pain may travel from the lower back to the hips, thighs, or legs. 5. Numbness or Tingling Compression of spinal nerves can cause tingling, numbness, or weakness in the legs or feet. When Does Lumbar Spondylosis Become Serious? Lumbar spondylosis may be considered serious if it leads to the following complications: Nerve Compression Bone spurs or disc degeneration can compress spinal nerves, leading to chronic pain, weakness, or sensory changes. Spinal Stenosis Narrowing of the spinal canal may occur, causing difficulty walking, balance problems, or leg pain during activity. Loss of Bladder or Bowel Control Although rare, this is a medical emergency and requires immediate attention. Persistent Pain Affecting Daily Life Pain that does not improve with conservative treatment may significantly impact work, sleep, and mobility. What Causes Lumbar Spondylosis to Worsen? शुरुआती अवस्था में सायटिका हल्की लग सकती है। लेकिन इलाज न करने पर यह गंभीर रूप ले सकती है।संदर्भित जोखिम:a Several factors can accelerate spinal degeneration or worsen symptoms: Aging Poor posture Sedentary lifestyle Obesity Repetitive heavy lifting Smoking Previous spinal injuries While lumbar spondylosis cannot be completely reversed, these factors can influence how serious it becomes. पैरों में स्थायी कमजोरी संतुलन की समस्या पेशाब या शौच पर नियंत्रण की समस्या चिंता न करें। सही इलाज और समय पर निदान से अधिकांश मामलों में पूरी तरह राहत मिलती है। How Is Lumbar Spondylosis Diagnosed? Diagnosis usually includes: Medical history and physical examination Assessment of posture, movement, and nerve function Imaging tests such as X-rays or MRI to assess disc and joint degeneration Early diagnosis helps prevent progression and complications. Is Surgery Needed for Lumbar Spondylosis? Surgery is rarely the first option. It may be considered only when: Symptoms do not improve with conservative treatment There is severe nerve compression Mobility or nerve function is significantly affected Most people with lumbar spondylosis never require surgery. Key Takeaway So, is lumbar spondylosis serious? For most people, lumbar spondylosis is a manageable, non-life-threatening condition. While it can cause discomfort and stiffness, serious complications are uncommon when the condition is identified early and managed properly. Paying attention to symptoms and adopting healthy spinal habits can significantly reduce the risk of long-term problems. Take Action: If you’re experiencing persistent back pain or stiffness, consult a spine specialist early to prevent progression and protect your spinal health. Please enable JavaScript in your browser to complete this form.Please enable JavaScript in your browser to complete this form.Full Name *Email *Phone Number * Submit
Best Sleeping Position for Back Pain
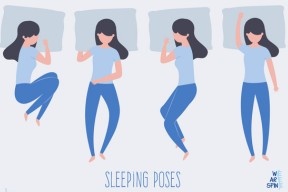
Best Sleeping Position for Back Pain Best Sleeping Position for Back Pain: How to Rest Without Discomfort Finding the best sleeping position for back pain can significantly improve comfort, sleep quality, and daily mobility. Many people focus on daytime posture but overlook how several hours of sleep in a poor position can strain the spine and surrounding muscles. Back pain may develop due to poor posture, muscle tension, spinal disc issues, or prolonged stress on the lower back. Selecting the right sleeping position supports natural spinal alignment and reduces unnecessary pressure during rest. This article explains how sleep posture affects back pain, outlines recommended sleeping positions, and provides practical guidance to improve nighttime comfort. Why Sleep Posture Is Important for Back Pain The spine has natural curves that help absorb shock and maintain balance. When sleep posture disrupts these curves, it can increase pressure on spinal discs, muscles, and ligaments. Over time, this may lead to stiffness, inflammation, or worsening pain. The best sleeping position for back pain helps: Maintain neutral spinal alignment Reduce disc compression Relax back and core muscles Support proper blood circulation A supportive sleeping posture allows the body to recover from daily strain and promotes better long-term spinal health. Best Sleeping Position for Back Pain: What Works Best 1. Sleeping on Your Back With Knee Support: Sleeping on your back is often recommended as the best sleeping position for back pain because it allows even weight distribution across the body. This position minimizes stress on the spine when proper support is used. To improve comfort: Place a pillow under your knees to maintain the natural curve of the lower back Use a pillow that keeps your neck aligned without pushing your head forward This position is particularly helpful for people with lower back stiffness or posture-related pain. 2. Side Sleeping With a Pillow Between the Knees Side sleeping is another commonly recommended option for those experiencing back pain. Adding a pillow between the knees improves pelvic alignment and reduces twisting of the lower spine. Helpful tips: Keep legs slightly bent, not tightly curled Use a firm pillow between the knees Ensure your head pillow aligns your neck with the spine For many individuals, this is among the best sleeping positions for back pain, especially when discomfort is linked to nerve irritation or muscle imbalance. 3. Fetal Position for Disc-Related Pain: The fetal position involves sleeping on your side with your knees drawn slightly toward your chest. This posture may help reduce pressure on spinal discs and ease nerve compression. This position may be beneficial for: Disc bulge or herniation symptoms Sciatic nerve discomfort However, it is important not to curl too tightly, as excessive bending can strain the neck and upper back. 4. Stomach Sleeping With Modifications: Stomach sleeping is usually not considered the best sleeping position for back pain because it can flatten the spine’s natural curve and strain the neck. However, if this position is unavoidable, small adjustments may help reduce stress. Suggestions include: Using a very thin pillow or none under the head Placing a pillow under the pelvis or lower abdomen These changes can reduce strain on the lower back and improve comfort. How Sleep Quality Affects Back Pain Poor sleep can increase pain sensitivity and slow muscle recovery. When sleep is disrupted, the body produces higher levels of stress hormones, which may worsen inflammation and discomfort. Improving sleep posture supports deeper, more restorative sleep and may reduce the frequency of pain flare-ups. When Back Pain Needs Medical Attention If back pain continues despite improving sleep posture, pillow support, and lifestyle habits, medical evaluation may be necessary. Ongoing pain may indicate issues such as disc problems, joint degeneration, or muscle imbalance that require professional care. Persistent pain that interferes with daily activities or sleep quality should not be ignored. Common Sleeping Mistakes to Avoid Some habits can unintentionally worsen back pain during sleep: Using multiple pillows that misalign the neck Sleeping on an overly soft mattress Staying in one position all night without adjustment Twisting the spine during side sleeping Avoiding these mistakes helps maintain spinal balance and comfort. Frequently Asked Questions (FAQs) What is the best sleeping position for back pain? Sleeping on your back with a pillow under the knees or side sleeping with knee support are often considered the best sleeping positions for back pain. Can poor sleep posture cause long-term back pain? Yes, prolonged poor posture during sleep can increase strain on spinal structures and contribute to chronic discomfort. Is side sleeping better than back sleeping for back pain? Both can be effective. The best option depends on individual comfort, pain location, and proper pillow support. Should back pain improve immediately after changing sleep position? Some people notice improvement quickly, while others may need several weeks for the body to adjust and heal. Sleeping on your back with a pillow under the knees or side sleeping with knee support are often considered the best sleeping positions for back pain. Yes, prolonged poor posture during sleep can increase strain on spinal structures and contribute to chronic discomfort. Both can be effective. The best option depends on individual comfort, pain location, and proper pillow support. Some people notice improvement quickly, while others may need several weeks for the body to adjust and heal. Please enable JavaScript in your browser to complete this form.Please enable JavaScript in your browser to complete this form.Full Name *Email *Phone Number * Submit
L4 L5 Disc Bulge Treatment
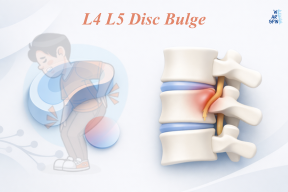
L4 L5 Disc Bulge Treatment L4 L5 Disc Bulge Treatment: Symptoms, Non-Surgical Options, Exercises, and Recovery Lower back pain is one of the most common musculoskeletal problems worldwide, and an L4 L5 disc bulge is a frequent cause. This condition can affect daily activities such as walking, sitting, bending, and even sleeping. The good news is that most people recover without surgery when the right treatment plan is followed. This comprehensive guide explains everything you need to know about L4 L5 disc bulge treatment, including symptoms, causes, treatment without surgery, effective exercises, and when surgery may be required. What Is an L4 L5 Disc Bulge? The human spine is made up of vertebrae separated by intervertebral discs that act as shock absorbers. The L4 L5 disc is located in the lower lumbar spine and carries significant body weight while allowing flexibility. A disc bulge occurs when the disc protrudes outward beyond its normal boundary but without tearing the outer layer (annulus fibrosus). This is different from a disc herniation, where the inner gel leaks out. Because the L4 L5 level is close to major spinal nerves, even a small bulge can cause pain and nerve-related symptoms. L4 L5 Disc Bulge Symptoms Symptoms vary depending on the severity of the bulge and nerve involvement. Common Symptoms Lower back pain Pain radiating to the buttocks or legs Stiffness in the lower back Difficulty bending or standing for long periods Nerve-Related Symptoms (Sciatica) Shooting pain down one leg Numbness or tingling in the leg or foot Muscle weakness Burning or electric-shock–like pain Severe Symptoms (Require Medical Attention) Loss of bowel or bladder control Progressive leg weakness Severe, unrelenting pain How Is L4 L5 Disc Bulge Diagnosed? Diagnosis usually involves: Physical examination Medical history review MRI scan (gold standard) X-rays (to rule out other conditions) MRI helps confirm the disc bulge and assess nerve compression. L4 L5 Disc Bulge Treatment (Overview) The goal of treatment is to: Relieve pain Reduce nerve compression Restore mobility Prevent recurrence In most cases, conservative care is effective, and surgery is not needed. L4 L5 Disc Bulge Treatment Without Surgery 1. Rest and Activity Modification Short-term rest helps reduce inflammation, but prolonged bed rest should be avoided. Light activities and walking promote healing. 2. Pain Management Doctors may recommend: NSAIDs (ibuprofen, naproxen) Muscle relaxants Short-term pain relievers These medications reduce inflammation and discomfort but should not be used long-term without medical advice. Physiotherapy (Most Important Non-Surgical Treatment) Physiotherapy plays a key role in L4 L5 disc bulge treatment without surgery. A structured program helps: Strengthen core and back muscles Improve flexibility Reduce pressure on the disc Prevent recurrence A physiotherapist designs a personalized plan based on pain level and mobility. Lifestyle Modifications Small daily changes make a big difference: Maintain correct sitting posture Use lumbar support Avoid heavy lifting Maintain a healthy weight Quit smoking (improves disc nutrition) Heat and Cold Therapy Cold packs reduce inflammation Heat therapy relaxes tight muscles Alternating both can help relieve pain. Epidural Steroid Injections (If Needed) For severe nerve pain, steroid injections may reduce inflammation and pain temporarily, allowing rehabilitation to continue. Best Exercises for L4 L5 Disc Bulge Always consult a physiotherapist before starting exercises. 1. Pelvic Tilts Strengthen core muscles Reduce lumbar stiffness 2. Knee-to-Chest Stretch Relieves lower back tension Improves flexibility 3. Cat-Cow Stretch Improves spinal mobility Reduces stiffness 4. Bridging Exercise Strengthens glutes and core Supports lumbar spine 5. McKenzie Extension Exercises Particularly useful if pain radiates down the leg Exercises to Avoid Heavy weightlifting Toe touches Twisting movements High-impact activities Sit-ups and crunches (initial phase) When Is Surgery Needed for L4 L5 Disc Bulge? Surgery is considered only when: Pain persists after 6–12 weeks of conservative treatment Progressive nerve damage occurs Severe weakness or loss of bladder/bowel control is present Common Surgical Options Microdiscectomy Laminectomy Even then, surgery is recommended only after careful evaluation. Can L4 L5 Disc Bulge Heal Naturally? Yes. In many cases: The bulge reduces over time Inflammation subsides Symptoms improve with conservative care This is why L4 L5 disc bulge treatment without surgery is the first-line approach. Frequently Asked Questions (FAQs) Is walking good for L4 L5 disc bulge? Yes, walking improves blood circulation and reduces stiffness when done moderately. Can I sit with an L4 L5 disc bulge? Yes, but avoid prolonged sitting and use lumbar support. Is bed rest recommended? Only short-term rest is advised. Movement aids recovery. Can physiotherapy cure L4 L5 disc bulge? Physiotherapy cannot “cure” the disc but effectively manages symptoms and promotes healing. Yes, walking improves blood circulation and reduces stiffness when done moderately. Yes, but avoid prolonged sitting and use lumbar support. Only short-term rest is advised. Movement aids recovery. Physiotherapy cannot “cure” the disc but effectively manages symptoms and promotes healing. Final Thoughts An L4 L5 disc bulge can be painful and disruptive, but most people recover fully with the right approach. L4 L5 disc bulge treatment without surgery, including physiotherapy, exercises, posture correction, and lifestyle changes, is effective in the majority of cases. Early diagnosis, consistent rehabilitation, and preventive care are key to long-term spine health. Please enable JavaScript in your browser to complete this form.Please enable JavaScript in your browser to complete this form.Full Name *Email *Phone Number * Submit
Does Sciatica go away
Does Sciatica go away Does Sciatica Go Away? Understanding Recovery and Treatment Many people experiencing shooting pain from the lower back down the leg often wonder, does sciatica go away, or is it a long-term condition. Sciatica is not a disease itself but a symptom caused by irritation or compression of the sciatic nerve, the largest nerve in the body. For most individuals, sciatica does improve over time. However, recovery depends on the underlying cause, lifestyle factors, and how early appropriate care begins. Understanding how sciatica develops and what influences recovery helps people manage symptoms effectively and avoid long-term discomfort. What Is Sciatica? Sciatica refers to pain that follows the path of the sciatic nerve, which runs from the lower spine through the hips, buttocks, and down each leg. The pain typically affects one side of the body. People asking does sciatica go away often experience symptoms such as: Sharp or burning pain in the lower back or leg Tingling or numbness in the leg or foot Muscle weakness Pain that worsens with sitting or bending Sciatica occurs when the nerve becomes compressed or inflamed, most commonly due to spinal conditions. Does Sciatica Go Away on Its Own? In many cases, sciatica does go away without surgical intervention. Mild to moderate sciatica often improves within a few weeks as inflammation reduces and the affected nerve recovers. However, recovery is not the same for everyone. Some people experience recurring episodes, while others may develop chronic symptoms if the underlying cause remains untreated. Common Causes That Affect Recovery Understanding the cause helps answer the question: does sciatica go away in a specific situation. 1. Slip Disc (Herniated Disc): A bulging or ruptured disc can press on the sciatic nerve. Many disc-related cases improve with conservative care, but severe compression may take longer to resolve. 2. Spinal Degeneration: Age-related changes such as disc degeneration or spinal narrowing can lead to repeated sciatic pain episodes. 3. Muscle Tightness: Tight muscles in the lower back or hips can irritate the sciatic nerve and usually improve with stretching and activity modification. 4. Poor Posture and Lifestyle Factors: Prolonged sitting, lack of movement, and improper lifting can prolong symptoms. How Long Does Sciatica Usually Last? Acute sciatica often improves within 4 to 6 weeks. During this time, inflammation gradually subsides, and nerve irritation reduces. If symptoms last longer than three months, the condition may be classified as chronic sciatica. At this stage, structured medical evaluation becomes more important. Does Sciatica Go Away Without Treatment? Acute sciatica often improves within 4 to 6 weeks. During this time, inflammation gradually subsides, and nerve irritation reduces. If symptoms last longer than three months, the condition may be classified as chronic sciatica. At this stage, structured medical evaluation becomes more important. Non-Surgical Treatment Options For most people, non-surgical care forms the foundation of recovery and answers the question does sciatica go away positively. Medication : Pain-relieving and anti-inflammatory medicines help control symptoms during flare-ups. Physiotherapy Physiotherapy focuses on: Improving flexibility Strengthening core and back muscles Reducing pressure on the sciatic nerve Regular exercise is one of the most effective long-term solutions. Posture and Ergonomic Changes : Correct sitting posture, proper sleeping positions, and ergonomic workspaces help prevent nerve irritation. Activity Modification : Avoiding heavy lifting and prolonged sitting reduces stress on the lower spine. When Does Sciatica Require Medical Attention? Although many cases improve, medical evaluation is essential if: Pain worsens despite home care Numbness or weakness increases Symptoms affect walking or balance Pain persists beyond several weeks These signs may indicate significant nerve compression. Surgical Treatment and Recovery Surgery is considered only when conservative treatment fails or nerve damage progresses. The goal is to relieve pressure on the sciatic nerve. Even in surgical cases, many people ask if sciatica goes away permanently. Surgery can provide lasting relief when appropriately indicated, especially when combined with rehabilitation. Lifestyle Changes That Support Recovery Lifestyle habits play a significant role in whether sciatica resolves fully. Helpful measures include: Maintaining a healthy body weight Regular low-impact exercise Avoiding prolonged sitting Practicing safe lifting techniques These changes reduce recurrence risk. Can Sciatica Come Back After Recovery? Yes, sciatica can return if the underlying causes persist. People who do not address posture, muscle strength, or spinal health may experience repeated episodes. Preventive care is essential even after symptoms improve. Does Sciatica Go Away Completely? For many individuals, sciatica does go away completely, especially when treated early and managed properly. Others may experience intermittent flare-ups that require ongoing care. Recovery depends on: Cause of nerve irritation Treatment consistency Lifestyle adjustments Living Well After Sciatica People recovering from sciatica often return to normal activities with appropriate care. Understanding the condition and following medical guidance helps maintain long-term spinal health. Asking if sciatica goes away is common, and in most cases, the answer is reassuring, yes, with the right approach and patience. Frequently Asked Questions (FAQs) Does sciatica go away faster with exercise or rest? Gentle movement and guided exercises generally support faster recovery than prolonged rest. Controlled activity helps improve circulation and reduces nerve irritation. Can sitting for long hours delay sciatica recovery? Yes. Prolonged sitting can increase pressure on the lower spine and slow recovery, especially without proper posture or breaks. Is sciatica more common in certain age groups? Sciatica is more frequently seen in adults between 30 and 60 years of age due to spinal wear-and-tear and disc changes. Can sciatica affect both legs at the same time? Sciatica usually affects one side, but in rare cases, nerve involvement can cause symptoms in both legs, requiring medical evaluation. Are lifestyle changes necessary after sciatica improves? Yes. Long-term habits such as regular exercise, posture correction, and weight management help reduce the risk of recurrence. Gentle movement and guided exercises generally support faster recovery than prolonged rest. Controlled activity helps improve circulation and reduces nerve irritation. Yes. Prolonged sitting can increase pressure on the lower spine and slow recovery, especially without proper posture or breaks. Sciatica is more frequently seen in adults between 30 and 60 years of age
Best Treatment for Slip Disc in India
Best Treatment for Slip Disc in India Back pain related to a slip disc is a frequent health concern among adults in India. Many individuals search for the best treatment for slip disc in India when persistent pain, numbness, or restricted movement begins to affect daily life. A slip disc medically referred to as a herniated or prolapsed disc occurs when the soft inner material of a spinal disc moves out of place and presses on nearby nerves. India offers a wide spectrum of evidence-based treatment options, ranging from conservative care to advanced surgical procedures. Understanding these approaches helps patients choose appropriate care based on symptoms, severity, and long-term health goals. What Is a Slip Disc? The spine consists of bones called vertebrae, separated by discs that act as shock absorbers. A slip disc develops when one of these discs weakens or ruptures, allowing its inner portion to bulge outward. This can irritate spinal nerves and cause pain or neurological symptoms. People seeking the best treatment for slip disc in India often benefit from early diagnosis, proper imaging, and structured care planning. Common Symptoms of a Slip Disc Symptoms vary depending on the disc’s location and nerve involvement, but commonly include: Persistent lower back or neck pain Pain radiating to the arms or legs Tingling or numbness in limbs Muscle weakness Difficulty sitting, standing, or walking for long periods Symptoms that worsen over time or interfere with daily activities should be medically evaluated. Best Treatment for Slip Disc in India: Non-Surgical Approaches Most slip disc cases improve without surgery. Non-surgical care is usually the first step in the best treatment for slip disc in India. Medication Management : Pain-relieving and anti-inflammatory medicines help reduce swelling around affected nerves and relieve discomfort during the acute phase. Physiotherapy : Physiotherapy plays a central role in recovery. A structured exercise program helps: Strengthen core and back muscles Improve spinal flexibility Reduce pressure on the affected disc Regular physiotherapy also lowers the risk of recurrence. 3. Activity Modification : Avoiding heavy lifting, maintaining proper posture, and limiting prolonged sitting support healing and reduce strain on the spine. 4. Spinal Injections : In selected cases, targeted injections may be used to reduce inflammation and control pain when other conservative treatments are insufficient. When Is Surgery Required? Surgery is not the first option for most patients. It may be considered when: Pain persists despite weeks of conservative care Progressive nerve weakness develops There is loss of bladder or bowel control Daily activities become severely limited The goal of surgery is to relieve nerve compression and restore function safely. Surgical Options Available in India For patients requiring intervention, the best treatment for slip disc in India may include modern, minimally invasive techniques. 1. Microdiscectomy This procedure removes the portion of the disc pressing on the nerve using small incisions, reducing tissue damage and recovery time. 2. Endoscopic Spine Surgery Endoscopic techniques use specialized instruments and cameras, allowing precise disc removal with minimal disruption to surrounding structures. 3. Spinal Decompression Procedures Used in complex or recurrent cases, these procedures relieve nerve pressure while maintaining spinal stability. Why Patients Seek Treatment in India Many patients look for the best treatment for slip disc in India because: Advanced diagnostic and treatment options are widely available Both conservative and surgical care are accessible Treatment costs are comparatively affordable Rehabilitation and follow-up care are integrated These factors make India a preferred destination for slip disc management. Living With a Slip Disc Many individuals manage slip disc symptoms successfully with lifestyle adjustments and medical guidance. Understanding the condition and following recommended care plans allows people to remain active and functional. Choosing the best treatment for slip disc in India involves personalized assessment, realistic expectations, and long-term commitment to spine health. Conclusion At We Are Spine, we understand that a slip disc can significantly impact daily life and mobility. Our team of fellowship-trained spine doctors who provide comprehensive care, ranging from conservative management to advanced minimally invasive surgical procedures. Your journey to lasting relief and spinal wellness begins with informed, expert care, consult our specialists today to determine the best treatment for your slip disc. Please enable JavaScript in your browser to complete this form.Please enable JavaScript in your browser to complete this form.Full Name *Email *Phone Number * Submit