Best Exercises for Desk Workers

16 Best Exercises for Desk Workers to Fix Posture & Relieve Pain Sitting all day is quietly damaging your body but the right movement routine can reverse much of the stiffness, pain, and posture decline caused by desk jobs. If you spend 6–12 hours daily at a computer, your neck, shoulders, hips, spine, wrists, and core are under constant stress. Over time, this can lead to: Neck stiffness Rounded shoulders Upper back tightness Lower back pain Tight hip flexors Weak glutes Wrist strain from typing Reduced mobility and energy Poor posture and spinal fatigue The good news? You do not need an intense gym routine to protect your spine. The best exercises for desk workers are short, targeted mobility and strengthening movements that restore posture, improve circulation, activate weak muscles, and reduce the harmful effects of prolonged sitting. This guide covers: The best stretches for office workers Desk job back pain relief exercises Posture correction exercises Neck stretches at work Hip mobility exercises Wrist exercises for typing A 5-minute desk workout A 15-minute daily mobility plan Mistakes most desk workers make Evidence-based posture recovery strategies Quick Answer: What Are the Best Exercises for Desk Workers? The best exercises for desk workers include: Chin tucks Cat-cow stretch Thoracic extensions Hip flexor stretch Glute bridges Shoulder blade squeezes Wrist mobility drills Planks Standing back extensions Walking breaks every 30–60 minutes These exercises help counteract: Forward head posture Rounded shoulders Tight hips Weak glutes Spinal compression Poor circulation caused by sitting all day Why Desk Jobs Damage the Body Humans are designed for movement not prolonged sitting. When you remain seated for hours: Hip flexors shorten Glutes become inactive Core muscles weaken The thoracic spine stiffens Neck muscles overwork Blood circulation slows Spinal discs experience continuous pressure This creates the classic “desk worker posture”: Forward head Rounded shoulders Tight chest Weak upper back Anterior pelvic tilt Lower back strain Over time, this may contribute to: Cervical spondylosis Lumbar pain Sciatica Disc problems Repetitive strain injuries Chronic stiffness Effects of Prolonged Sitting on the Body Body Area Common Problem Why It Happens Neck Forward head posture Screen positioning Shoulders Rounded shoulders Tight chest muscles Upper back Stiff thoracic spine Lack of movement Lower back Disc pressure Poor sitting posture Hips Tight hip flexors Constant seated position Glutes Weakness (“dead butt syndrome”) Muscle inactivity Wrists Typing strain Repetitive motion Core Weakness Reduced activation How Often Should Desk Workers Stretch? Most physiotherapists recommend: Movement breaks every 30–60 minutes Stretching 2–4 times daily At least 15–30 minutes of total movement daily Even brief movement snacks improve: Blood circulation Posture awareness Joint lubrication Muscle activation Energy and focus Best Exercises for Desk Workers by Body Part Neck Exercises for Desk Workers 1. Chin Tucks What It Helps Forward head posture Neck stiffness Tension headaches Cervical strain How to Do It Sit upright Pull your chin backward gently Keep eyes level Hold for 5 seconds Repeat 10 times Duration/Reps 2 sets of 10 reps Common Mistakes Tilting the head down Forcing the movement Beginners Modification Perform against a wall for posture support. Who Should Avoid It Avoid aggressive motion if you have severe cervical pain or dizziness. 2. Upper Trapezius Stretch What It Helps Tight neck muscles Shoulder tension Stress-related stiffness Steps Sit tall Tilt head sideways Use opposite hand gently Hold 20–30 seconds Reps 2–3 per side Mistakes Pulling too hard Shrugging shoulders Shoulder Mobility Exercises 3. Shoulder Blade Squeezes Benefits Improves posture Activates upper back muscles Reduces rounded shoulders Steps Sit or stand tall Pull shoulder blades backward Hold 5 seconds Relax slowly Reps 15 repetitions Common Mistakes Arching lower back Lifting shoulders upward 4. Wall Angels Helps Thoracic mobility Posture correction Shoulder mobility Instructions Stand against wall Keep arms in “goalpost” position Slide arms upward slowly Maintain contact with wall Reps 10 repetitions Beginners Tip Reduce range if shoulders feel tight. Upper Back Stretches for Office Workers 5. Cat-Cow Stretch Benefits Improves spinal mobility Relieves stiffness Enhances circulation Steps Start on hands and knees Arch spine upward Then lower belly and lift chest Move slowly with breathing Reps 10–15 repetitions Mistakes Moving too fast Holding breath 6. Thoracic Extension Stretch What It Helps Rounded posture Upper back stiffness Desk-related slouching Instructions Sit on chair Place hands behind head Lean upper back gently backward Hold briefly Reps 10 repetitions Lower Back Pain Relief Exercises 7. Standing Back Extensions Helps Lumbar stiffness Disc pressure from sitting Lower back fatigue Steps Stand upright Place hands on hips Lean backward gently Return slowly Reps 10 repetitions every few hours Avoid If Pain shoots down the leg. 8. Child’s Pose Benefits Gentle spinal decompression Relaxation Lower back stretching Hold 30–60 seconds Beginners Tip Place pillow under hips if uncomfortable. Hip Mobility Exercises for Desk Workers 9. Hip Flexor Stretch Why It Matters Sitting shortens hip flexors, pulling the pelvis forward and stressing the lower back. Steps Kneel on one knee Shift hips forward Keep chest upright Hold stretch Duration 30 seconds each side Common Mistakes Leaning forward excessively Overarching lower back 10. Figure-4 Glute Stretch Helps Tight hips Piriformis tension Sciatic irritation Steps Sit on chair Cross ankle over opposite knee Lean forward slightly Hold 20–30 seconds Glute Activation Exercises 11. Glute Bridges Benefits Activates weak glutes Supports lower back Improves pelvic stability Instructions Lie on back Bend knees Lift hips upward Squeeze glutes Reps 12–15 repetitions Mistakes Using lower back excessively Rushing the movement 12. Bodyweight Squats Helps Improve circulation Strengthen hips and legs Reverse prolonged sitting stiffness Reps 10–15 repetitions Beginners Tip Use chair support if needed. Wrist Exercises for Typing and Computer Users 13. Wrist Flexor Stretch Pain in upper left back is a common condition that may develop because of muscle strain, poor posture, cervical spine problems, stress, or degenerative changes in the spine. While many cases improve with rest, posture correction, exercises, and physiotherapy, persistent symptoms should not be ignored. Benefits Reduces typing strain Improves forearm flexibility Helps prevent repetitive strain injury Steps Extend arm
Pain in Upper left back
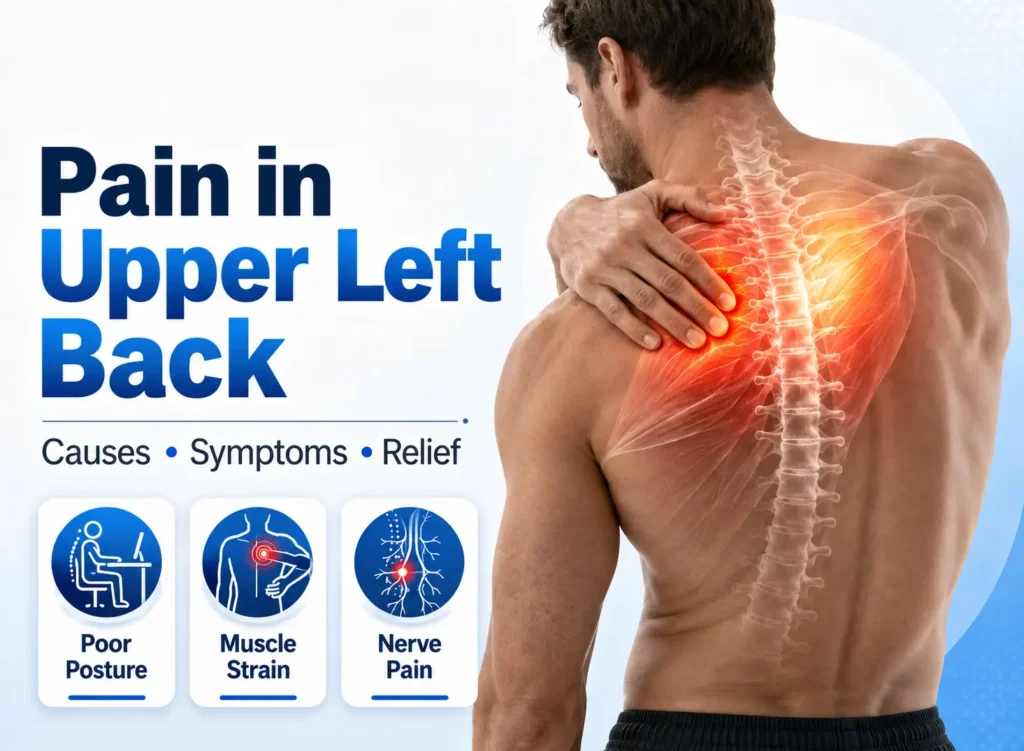
Pain in Upper Left Back: Causes, Symptoms & Treatment Pain in upper left back is a common complaint that can affect people of all ages. The discomfort may appear suddenly after physical activity or gradually develop because of posture-related strain, muscle tension, or spine-related problems. Some people experience mild stiffness, while others may feel sharp pain, burning sensations, or restricted movement. The upper back, also known as the thoracic spine, supports the shoulders, neck, and rib cage. Because several muscles, joints, ligaments, and nerves are connected in this area, pain in upper left back can develop from multiple causes. Long working hours, poor posture, stress, lack of exercise, and repetitive movements are among the most common contributors. In many cases, pain in upper left back improves with rest, posture correction, physiotherapy, and exercises. However, persistent symptoms should not be ignored, especially if the pain is associated with numbness, weakness, chest discomfort, or breathing difficulty. Understanding the possible causes and symptoms of pain in upper left back can help patients seek timely treatment and prevent long-term complications. What Does Pain in Upper Left Back Mean? Pain in upper left back refers to discomfort felt on the left side of the upper thoracic region, usually between the neck and lower rib cage. The pain may involve muscles, spinal joints, discs, nerves, or connective tissues. Some people describe pain in upper left back as: A dull ache Sharp stabbing pain Burning discomfort Tightness around the shoulder blade Muscle spasms Pain during movement The discomfort may remain localized or spread to nearby areas such as: Neck Left shoulder Arm Chest Shoulder blade Upper ribs The severity and duration of pain in upper left back often depend on the underlying cause. Common Causes of Pain in Upper Left Back Several medical and lifestyle-related conditions can contribute to pain in upper left back. 1. Muscle Strain Muscle strain is one of the most common causes of pain in upper left back. Lifting heavy objects, repetitive arm movements, poor sleeping posture, or sudden twisting motions may strain the upper back muscles. Common symptoms include: Muscle tightness Tenderness Pain while moving Stiffness after rest Muscle-related pain in upper left back usually improves with stretching, rest, and physiotherapy. 2. Poor Posture Poor posture places excessive stress on the upper spine and surrounding muscles. Sitting for long hours with rounded shoulders or forward head posture can lead to chronic pain in upper left back. People working on computers or mobile devices for extended periods are especially prone to posture-related upper back pain. 3. Cervical Spine Problems Conditions such as cervical spondylosis or cervical disc degeneration can sometimes cause referred pain in upper left back. Nerve irritation in the neck may spread pain toward the shoulder blade and upper thoracic area. Symptoms may include: Neck stiffness Tingling in the arm Headaches Shoulder discomfort 4. Pinched Nerve Compression of spinal nerves can cause pain in upper left back along with numbness, burning sensations, or weakness in the arm. A pinched nerve may develop because of: Herniated discs Bone spurs Degenerative spine conditions 5. Thoracic Spine Problems The thoracic spine itself may contribute to pain in upper left back. Disc problems, joint inflammation, or spinal degeneration in the upper back region can trigger chronic discomfort. 6. Stress and Muscle Tension Stress is another major cause of pain in upper left back. Emotional stress often leads to tightening of muscles around the neck, shoulders, and upper back. This may result in the: Tight muscles Trigger points Shoulder stiffness Persistent aching pain 7. Shoulder Blade Dysfunction Weakness or imbalance around the shoulder blade muscles may affect posture and movement patterns, contributing to pain in upper left back. Patients may notice: Clicking sensations Pain near the shoulder blade Weakness during lifting Difficulty maintaining posture 8. Osteoarthritis Age-related wear and tear in spinal joints may cause stiffness and chronic pain in upper left back, particularly in older adults. Different Types of Pain in Upper Left Back Pain in upper left back may feel different depending on the underlying cause. Sharp Pain Sharp pain may occur due to muscle strain, sudden injury, or nerve irritation. Burning Pain Burning sensations may indicate nerve involvement or inflammation. Dull Aching Pain A dull ache is commonly associated with posture-related muscle fatigue and stress. Pain While Breathing Pain during deep breathing may sometimes involve muscles between the ribs or irritation around the thoracic region. Pain During Movement Pain that worsens while twisting, bending, or lifting often suggests muscular or spinal involvement.the Symptoms Associated With Pain in Upper Left Back The symptoms associated with pain in upper left back vary depending on the underlying condition. Common symptoms include: Muscle tightness Neck pain Shoulder pain Tingling sensations Numbness Reduced mobility Burning pain Headaches Stiffness Pain during movement Some individuals experience intermittent symptoms, while others may develop chronic pain in upper left back that affects daily activities. Can Pain in Upper Left Back Be Serious? In many cases, pain in upper left back develops because of muscle strain, poor posture, or stress. However, certain symptoms may indicate a more serious medical condition. Seek immediate medical attention if pain in upper left back is associated with: Chest pain Breathing difficulty Severe weakness Fever Sudden numbness Loss of balance Unexplained weight loss Loss of bladder or bowel control Rarely, pain in upper left back may be linked to heart, lung, or severe nerve-related conditions. Persistent symptoms should always be evaluated by a healthcare professional. How Is Pain in Upper Left Back Diagnosed? Doctors usually begin a diagnosis with a detailed physical examination and medical history. The evaluation may include: Posture assessment Neck and shoulder movement evaluation Muscle strength testing Reflex examination Nerve function assessment Depending on symptoms, imaging tests may also be recommended. X-rays X-rays help identify arthritis, spinal alignment problems, and degenerative changes. MRI Scan MRI scans provide detailed images of spinal discs, nerves, muscles, and soft tissues. CT Scan CT scans may help detect bone-related abnormalities. Nerve Tests EMG and nerve conduction studies may
Left Side Upper Back Pain

Left Side Upper Back Pain: Causes, Symptoms & Relief Left side upper back pain is a common problem that can affect people of all ages. The discomfort may range from mild stiffness and muscle tightness to sharp pain that interferes with daily activities. Many people experience left side upper back pain due to poor posture, muscle strain, stress, or spine-related conditions. In some cases, the pain may also be linked to nerve irritation or underlying medical conditions. The upper back, also known as the thoracic spine, supports the shoulders, neck, and rib cage. Because this region is connected to several muscles, joints, and nerves, pain in this area can develop from multiple causes. Long hours of sitting, excessive screen time, improper lifting techniques, and lack of movement are among the most common contributors to left side upper back pain. While most cases improve with rest, posture correction, stretching, and physiotherapy, persistent or severe symptoms should never be ignored. Understanding the causes, symptoms, and treatment options for left side upper back pain can help you seek timely care and prevent long-term complications. Left side upper back pain may sometimes develop due to underlying cervical spondylosis, especially when nerve compression affects the neck and shoulder region. What Is Left Side Upper Back Pain? Left side upper back pain refers to discomfort that occurs in the upper-left portion of the back, usually between the neck and the lower rib cage. The pain may involve muscles, ligaments, joints, spinal discs, or nerves in the thoracic region. Some people experience dull aching pain, while others feel burning sensations, stiffness, muscle spasms, or sharp pain during movement. Left side upper back pain may appear suddenly after physical activity or gradually worsen over time because of poor posture and repetitive strain. The pain can sometimes spread to nearby areas such as: Neck Left shoulder Shoulder blade Chest Arm Upper ribs The severity and location of symptoms often depend on the underlying cause. Common Causes of Left Side Upper Back Pain There are several possible causes of left side upper back pain. Some are related to muscles and posture, while others may involve the spine, nerves, or internal organs. 1. Muscle Strain Muscle strain is one of the leading causes of left side upper back pain. Overuse, sudden twisting movements, lifting heavy objects, or sleeping in an awkward position can strain the muscles in the upper back. Common symptoms include: Muscle tightness Tenderness Pain during movement Stiffness after rest Muscle-related left side upper back pain often improves with rest, stretching, and physiotherapy. 2. Poor Posture Poor posture is another major reason for left side upper back pain. Sitting for long hours with rounded shoulders or forward head posture places excessive stress on the upper spine and surrounding muscles. People who work on computers for extended periods are especially vulnerable to posture-related left side upper back pain. 3. Cervical Spondylosis Degenerative changes in the cervical spine can sometimes cause pain that radiates into the upper back and shoulder blade area. Nerve compression from cervical spondylosis may trigger left side upper back pain along with neck stiffness, tingling, or numbness in the arm. Patients with persistent symptoms may benefit from evaluation by a spine specialist. 4. Herniated Disc A bulging or herniated disc in the cervical or upper thoracic spine may irritate nearby nerves and lead to left side upper back pain. Disc-related pain may worsen during coughing, sneezing, or prolonged sitting. Other symptoms may include: Tingling sensations Arm weakness Numbness Burning pain 5. Stress and Muscle Tension Stress can contribute significantly to left side upper back pain. Emotional stress often causes muscle tension in the neck, shoulders, and upper back. This may result in: Tight muscles Trigger points Stiffness Shoulder discomfort Stress management, stretching, and breathing exercises can help reduce tension-related pain. 6. Scapular Dysfunction The shoulder blade plays an important role in upper body movement. Weakness or imbalance in the muscles surrounding the scapula can lead to abnormal movement patterns and left side upper back pain. People with scapular dysfunction may notice: Pain near the shoulder blade Clicking sensations Weakness while lifting Poor posture 7. Osteoarthritis Age-related wear and tear in the spine joints may cause inflammation and stiffness in the thoracic region. Osteoarthritis can contribute to chronic left side upper back pain, especially in older adults. 8. Injury or Trauma Sports injuries, falls, accidents, or sudden impacts may damage muscles, joints, or ligaments in the upper back. Trauma-related left side upper back pain should be evaluated if symptoms are severe or persistent. Symptoms Associated With Left Side Upper Back Pain The symptoms of left side upper back pain vary depending on the underlying condition. Common symptoms include: Dull aching pain Sharp or stabbing pain Muscle tightness Burning sensations Stiffness Shoulder pain Neck pain Tingling or numbness Reduced mobility Pain while twisting or bending Can Left Side Upper Back Pain Be Serious? In many cases, left side upper back pain is caused by muscle strain or posture-related issues. However, certain symptoms may indicate a more serious condition that requires immediate medical attention. Seek medical care if left side upper back pain is associated with: Chest pain Shortness of breath Sudden weakness Fever Unexplained weight loss Severe numbness Difficulty walking Loss of bladder or bowel control Rarely, left side upper back pain may be linked to heart, lung, or kidney problems. Persistent symptoms should always be evaluated by a qualified healthcare professional. How Is Left Side Upper Back Pain Diagnosed? A spine specialist will usually begin with a detailed medical history and physical examination. The doctor may assess: Posture Neck and shoulder movement Muscle strength Reflexes Nerve function Depending on symptoms, imaging tests may also be recommended. X-rays X-rays help identify spinal alignment problems, arthritis, or degenerative changes. MRI Scan MRI scans provide detailed images of discs, nerves, muscles, and soft tissues. CT Scan CT scans may help detect bone-related abnormalities. Nerve Tests Electromyography (EMG) and nerve conduction studies may be used if nerve compression is suspected. Best
Is Sciatica a Disability ?

Is Sciatica a Disability? Understanding Your Rights, Symptoms, and Limitations Sciatica can make sitting, standing, walking, and even sleeping extremely painful. For some people, the condition causes mild discomfort that improves with rest and therapy. For others, it becomes a long-term problem that interferes with work, mobility, and daily life. This leads many people to ask an important question: Is sciatica a disability? The answer depends on the severity of symptoms, how long the condition lasts, and how much it limits your ability to work or perform everyday activities. In some cases, severe chronic sciatica may qualify as a disability under workplace accommodation laws or disability benefit programs. Is Sciatica a Disability? Quick Answer Yes, sciatica can be considered a disability in severe cases if it significantly limits mobility, work ability, or daily functioning for an extended period. Mild or temporary sciatica usually does not qualify as a disability, but chronic sciatica with nerve damage, severe pain, weakness, or functional limitations may meet disability criteria depending on medical evaluation and local laws. What Is Sciatica? Sciatica is a condition caused by irritation or compression of the sciatic nerve, the largest nerve in the body. Sciatic Nerve→Lower Back→Leg The sciatic nerve travels from the lower spine through the hips and down each leg. When compressed or inflamed, it may cause: Sharp shooting pain Burning sensation Tingling Numbness Muscle weakness Difficulty walking or standing If you are unfamiliar with the condition, this detailed guide on sciatica causes, symptoms, and treatments explains how sciatica develops and why symptoms can vary from person to person. What Causes Sciatica? Sciatica itself is not a disease. It is usually a symptom of an underlying spinal problem. Common Causes Herniated disc Degenerative disc disease Spinal stenosis Piriformis syndrome Bone spurs Lumbar disc bulge Spinal injury Some people confuse sciatica with ordinary back pain, but there are important differences between sciatica and lower back pain , especially when nerve symptoms are involved. When Does Sciatica Become a Disability? The key factor is functional limitation. Sciatica May Be Considered a Disability If It: Prevents you from working Limits walking or standing Causes chronic severe pain Leads to muscle weakness Reduces mobility significantly Interferes with daily activities Requires long-term medical treatment Common Severe Symptoms Persistent nerve pain Leg weakness Loss of balance Difficulty sitting for long periods Reduced range of motion Foot drop Severe numbness People with chronic symptoms often ask does sciatica go away , especially when pain lasts for months despite conservative treatment. Mild Sciatica vs Severe Sciatica Mild Sciatica Severe Sciatica Temporary discomfort Chronic debilitating pain Occasional leg pain Persistent nerve pain Minimal mobility issues Walking difficulties Improves with rest Pain despite treatment Usually manageable Significant functional limitations Not every case of sciatica qualifies as a disability. The severity and duration matter significantly. Symptoms That May Support Disability Claims Physical Symptoms Chronic pain Numbness Weakness Reduced mobility Difficulty lifting Inability to sit or stand for long periods Work-Related Limitations Reduced productivity Missed workdays Inability to perform physical tasks Difficulty commuting Limited concentration due to pain Is Sciatica a Disability Under Workplace Laws? In many countries, chronic medical conditions that substantially limit daily activities may qualify for workplace accommodations. Possible Workplace Accommodations Ergonomic seating Standing desks Reduced lifting duties Flexible schedules Frequent movement breaks Remote work options The exact legal definition depends on your country’s disability laws and employment regulations. Can You Get Disability Benefits for Sciatica? In severe cases, some individuals may qualify for disability benefits if: Symptoms are medically documented Conservative treatment failed Mobility is significantly impaired Work ability is reduced long term Documentation Often Required MRI reports Neurological evaluations Medical records Physical therapy history Functional limitation assessments How Sciatica Affects Daily Life Understanding how debilitating sciatica can become helps answer the question: Is sciatica a disability? Everyday Challenges Pain while driving Difficulty climbing stairs Trouble sleeping Reduced exercise capacity Difficulty sitting at work Walking limitations For many people, even basic daily tasks become exhausting during severe flare-ups. Common Jobs Most Affected by Severe Sciatica High-Risk Occupations Construction workers Drivers Warehouse workers Nurses Factory workers Office workers sitting long hours Can Sciatica Improve Without Surgery? Yes, many cases improve with conservative treatment. Common Non-Surgical Treatments Physical therapy Stretching exercises Pain medication Heat and cold therapy Lifestyle changes Epidural injections Many patients explore non-surgical treatments for sciatica and slip disc before considering surgery. Benefits of Early Sciatica Treatment Treating sciatica early may: Reduce nerve irritation Improve mobility Prevent chronic pain Reduce disability risk Improve quality of life Support faster recovery Limitations and Challenges of Sciatica Recovery While many people recover well, not all cases improve quickly. Challenges Recurring flare-ups Slow nerve healing Sedentary lifestyle habits Poor posture Delayed treatment Chronic inflammation Recovery timelines vary widely between individuals. Real-World Example A 45-year-old delivery driver developed severe sciatica from a lumbar disc herniation. Initially, symptoms included lower back pain and occasional leg tingling. Over time, the pain worsened, making driving and prolonged sitting difficult. After several months: Walking became painful Sleep quality declined Work attendance decreased The individual eventually required physical therapy, ergonomic modifications, and temporary work restrictions. With consistent treatment and rehabilitation, mobility gradually improved. Step-by-Step Guide: What to Do If Sciatica Is Affecting Your Daily Life Step 1: Seek Medical Evaluation Proper diagnosis is essential to identify the underlying spinal issue. Step 2: Document Symptoms Keep records of: Pain severity Mobility limitations Missed workdays Functional challenges Step 3: Start Conservative Treatment Treatment may include: Physiotherapy Stretching Medication Lifestyle changes Some people find additional relief with acupuncture at home for sciatica alongside medical treatment and rehabilitation exercises. Step 4: Improve Movement and Flexibility Gentle stretching may help reduce stiffness and nerve tension. A structured yoga routine for sciatica relief may support flexibility, posture, and lower back mobility when performed safely Step 5: Follow Long-Term Spine Care Habits Recovery often depends on: Weight management Posture correction Activity modification Consistent exercise Many people also try simple strategies for sciatica relief at home to manage symptoms naturally between therapy sessions. Tools and Resources
Best Yoga Poses for Back Pain Relief

Best Yoga Poses for Back Pain: 12 Expert-Recommended Stretches for Lasting Relief Back pain can turn simple daily activities into a struggle. Sitting for long hours, poor posture, muscle stiffness, stress, and lack of movement are some of the biggest reasons millions of people experience discomfort in the lower back, upper back, and spine. The good news? Practicing the best yoga poses for back pain regularly may help reduce stiffness, improve flexibility, strengthen supporting muscles, and support better spinal health naturally. Whether you deal with mild lower back tension after work or recurring stiffness from poor posture, yoga offers a gentle yet effective way to improve mobility and reduce pain without high-impact exercise. People experiencing neck stiffness and posture-related discomfort may also benefit from specific routines like yoga for cervical spondylosis , which focuses on improving spinal flexibility and reducing cervical strain. Best Yoga Poses for Back Pain: Quick Answer The best yoga poses for back pain include Child’s Pose, Cat-Cow Stretch, Cobra Pose, Downward Dog, Sphinx Pose, Bridge Pose, Supine Twist, and Knees-to-Chest Pose. These yoga poses help stretch tight muscles, improve spinal mobility, strengthen the core, and reduce tension that contributes to chronic or occasional back pain. Why Yoga Helps Relieve Back Pain Yoga combines stretching, controlled breathing, posture correction, and muscle strengthening. Unlike high-impact workouts, yoga focuses on slow and mindful movement, making it ideal for people with stiffness or mild-to-moderate back discomfort. Research suggests yoga may help: Improve spinal flexibility Reduce muscle tension Strengthen core muscles Enhance posture Improve circulation Lower stress-related muscle tightness Support long-term mobility Many doctors, physiotherapists, and rehabilitation specialists now recommend yoga as part of a conservative back pain management plan. Common Causes of Back Pain Before practicing yoga, it helps to understand what may be causing your discomfort. Muscle-Related Causes Tight hamstrings Weak core muscles Muscle strain Poor posture Sedentary lifestyle Spine-Related Causes Herniated disc Sciatica Degenerative disc disease Spinal arthritis Spondylosis People experiencing persistent neck pain, stiffness, headaches, or tingling sensations should also watch for the early signs of cervical spondylosis, especially if they spend long hours sitting or working on screens. Lifestyle Factors Sitting for long hours Stress and tension Obesity Lack of physical activity Poor sleeping posture If your pain is severe, associated with numbness, weakness, fever, or loss of bladder/bowel control, seek medical attention immediately. 12 Best Yoga Poses for Back Pain Relief 1. Child’s Pose (Balasana) Child’s Pose is one of the safest and best yoga poses for back pain because it gently stretches the lower back and hips. How to Do It Kneel on the floor. Sit back on your heels. Stretch your arms forward. Lower your chest toward the floor. Hold for 30–60 seconds. Benefits Relaxes spinal muscles Reduces lower back tension Calms the nervous system Improves flexibility 2. Cat-Cow Stretch The Cat-Cow sequence improves spinal mobility and helps warm up stiff back muscles. How to Do It Start on all fours. Inhale and arch your back (Cow Pose). Exhale and round your spine (Cat Pose). Repeat slowly for 1–2 minutes. Benefits Increases spinal flexibility Improves posture Reduces stiffness Encourages healthy movement For people dealing with neck stiffness and posture-related discomfort, combining yoga with targeted cervical spondylosis exercises may help improve mobility and reduce muscle tightness. 3. Cobra Pose (Bhujangasana) Cobra Pose strengthens the spine and opens tight chest muscles caused by prolonged sitting. How to Do It Lie face down. Place palms under shoulders. Lift your chest gently while keeping hips grounded. Hold for 15–30 seconds. Benefits Strengthens lower back muscles Improves spinal extension Reduces slouching posture Opens the chest Avoid If You have severe disc problems You feel sharp pain during extension People diagnosed with lumbar disc issues may also want to understand available L4-L5 disc bulge treatment options before starting intense stretching routines. 4. Downward Facing Dog This full-body stretch helps decompress the spine and lengthen tight muscles. Benefits Stretches hamstrings and calves Relieves spinal compression Improves circulation Strengthens shoulders and core Beginner Tip Bend your knees slightly if your hamstrings feel tight. 5. Sphinx Pose Sphinx Pose is gentler than Cobra Pose and often recommended for beginners. Why It Works The pose encourages mild spinal extension without excessive pressure on the lower back. Benefits Supports lumbar mobility Helps reduce stiffness Beginner-friendly Improves posture 6. Knees-to-Chest Pose This simple stretch releases tension in the lower back. How to Perform Lie on your back. Pull both knees toward your chest. Hold gently for 30 seconds. Benefits Relaxes lumbar muscles Reduces lower back tightness Massages spinal muscles 7. Supine Spinal Twist Twisting stretches may improve spinal mobility and reduce muscular tension. Benefits Relieves stiffness Improves spinal rotation Helps relax muscles Enhances flexibility Important Move gently and avoid forcing the twist. People experiencing radiating leg pain or nerve-related symptoms may benefit from a dedicated yoga routine for sciatica relief designed specifically for sciatic nerve discomfort. 8. Bridge Pose Bridge Pose strengthens the glutes and core, which are important for spinal support. Benefits Strengthens posterior chain muscles Improves hip mobility Supports posture Activates core muscles Weak glutes are often linked to recurring lower back pain. 9. Triangle Pose Triangle Pose stretches the sides of the body while improving balance and stability. Benefits Improves posture Enhances flexibility Strengthens legs and core Opens hips and spine 10. Seated Forward Bend This pose stretches the lower back and hamstrings. Benefits Releases muscle tightness Improves flexibility Calms the mind Reduces tension Caution Avoid excessive rounding if you have disc-related pain. 11. Happy Baby Pose Happy Baby Pose gently opens the hips and decompresses the lower spine. Benefits Relieves lumbar pressure Stretches inner thighs Reduces stress Encourages relaxation 12. Legs-Up-the-Wall Pose This restorative pose is excellent for recovery and relaxation. Benefits Relieves pressure on the spine Improves circulation Reduces fatigue Supports relaxation It is one of the easiest and most relaxing yoga poses for beginners. Comparison Table: Best Yoga Poses for Back Pain Yoga Pose Best For Difficulty Level Main Benefit Child’s Pose Lower back tension Beginner Gentle stretch
Does Scoliosis Get Worse With Age?

Does Scoliosis Get Worse With Age? What Adults Need to Know About Spine Changes Over Time Many people believe scoliosis is only a teenage condition. However, adults across their 40s, 50s, and even 70s are increasingly being diagnosed with spinal curvature problems that affect posture, mobility, and quality of life. One of the most common questions patients ask spine specialists is: does scoliosis get worse with age? The answer is often yes. In many adults, scoliosis can gradually worsen over time due to spinal degeneration, weak muscles, arthritis, osteoporosis, and disc wear. While mild curves may remain stable for years, moderate or severe scoliosis can progress and lead to chronic pain, stiffness, nerve compression, walking difficulty, and reduced independence if not managed properly. The good news is that modern spine care, physiotherapy, targeted exercise, and early intervention can help slow progression and improve long-term spine health. Quick Answer: Does Scoliosis Get Worse With Age? Yes, scoliosis can worsen with age, especially in adults with degenerative spine changes or untreated spinal curves from adolescence. Ageing-related disc degeneration, osteoporosis, arthritis, and muscle weakness may increase spinal curvature over time. However, early diagnosis, exercise, physiotherapy, and expert spine care can help manage symptoms and slow progression. What Is Scoliosis? Type Description Common Age Group Idiopathic Scoliosis Cause unknown Teenagers Congenital Scoliosis Present at birth Infants Neuromuscular Scoliosis Linked to neurological disorders Children & Adults Degenerative Scoliosis Caused by age-related spinal wear Adults over 40 Degenerative scoliosis is one of the fastest-growing spine conditions seen in older adults today. Why Does Scoliosis Get Worse With Age? The reason many people search for does scoliosis get worse with age is because symptoms often become more noticeable later in life. Even a mild spinal curve from youth may become painful decades later. Several age-related factors contribute to progression. 1. Degenerative Disc Changes As people age, spinal discs lose hydration, elasticity, and height. This creates uneven pressure across the spine and can increase spinal curvature. Degenerative disc disease may also contribute to: Lower back pain Reduced flexibility Stiffness Nerve irritation Muscle fatigue Patients experiencing disc-related pain may also benefit from learning about the 4 stages of disc herniation and how degeneration affects spinal stability. 2. Arthritis in the Spine Spinal arthritis causes inflammation and wear in the joints connecting the vertebrae. Over time, arthritis can destabilize spinal alignment and worsen scoliosis. Common symptoms include: Morning stiffness Difficulty standing upright Reduced range of motion Persistent lower back pain 3. Osteoporosis and Bone Weakness Bone density naturally decreases with age, particularly in women after menopause. Osteoporosis weakens the vertebrae, making the spine more vulnerable to curvature progression. This is one major reason why does scoliosis get worse with age becomes especially relevant after age 50. 4. Weak Core Muscles The muscles surrounding the spine help maintain posture and alignment. Ageing, inactivity, prolonged sitting, and lack of exercise can weaken these support structures. Poor muscle support may accelerate: Postural imbalance Spinal instability Chronic pain Mobility limitations Regular movement and targeted physiotherapy become increasingly important with age. 5. Untreated Childhood Scoliosis Adults who were diagnosed with scoliosis during adolescence may experience progression later in life, especially if the spinal curve exceeded 30–40 degrees. In many cases, patients remain symptom-free for years before degeneration begins triggering pain and imbalance. Signs Your Scoliosis May Be Progressing Not all scoliosis cases worsen significantly. However, certain symptoms suggest progression and should not be ignored. Common Warning Signs Increasing back pain Uneven shoulders or hips Leaning to one side Height loss Difficulty standing for long periods Leg numbness or tingling Fatigue while walking Reduced mobility Visible posture changes If scoliosis begins affecting nerves, patients may also experience radiating leg pain similar to sciatica. Understanding spinal nerves and back pain can help explain why nerve symptoms occur. Does Mild Scoliosis Get Worse With Age? Mild scoliosis often remains stable for years, particularly when the curve is below 20 degrees. However, progression is still possible depending on: Bone health Lifestyle Weight Activity levels Muscle strength Menopause Existing spinal degeneration Even mild scoliosis may become painful with aging because of joint stress and muscle imbalance. So while progression varies between individuals, the answer to does scoliosis get worse with age is still yes for many adults. Adult Scoliosis vs Adolescent Scoliosis Factor Adolescent Scoliosis Adult Scoliosis Main Cause Growth spurts Degeneration Pain Level Often painless Frequently painful Progression During growth years Slow progression over decades Treatment Bracing & monitoring Therapy, injections, surgery Associated Issues Cosmetic concerns Pain & nerve compression Can Scoliosis Cause More Pain as You Age? Yes. Pain is one of the most common symptoms in adults with scoliosis. As spinal curvature progresses, abnormal pressure develops on: Spinal discs Facet joints Muscles Ligaments Nerves This may lead to: Chronic lower back pain Neck pain Muscle spasms Sciatica symptoms Difficulty walking Reduced stamina Patients with radiating nerve pain often explore therapies like acupuncture at home for sciatica relief or gentle movement programs, such as a yoga routine for sciatica relief. Does Scoliosis Get Worse With Age After 40? Many adults first notice scoliosis symptoms after age 40 because spinal degeneration accelerates during this period. Several factors increase progression risk: Sedentary lifestyle Weight gain Poor posture Desk jobs Reduced flexibility Disc degeneration Osteoporosis Modern work habits involving prolonged sitting can significantly increase spinal stress over time. Maintaining a spine-friendly diet for disc health may also support overall spinal function and reduce inflammation. How Fast Does Scoliosis Progress in Adults? Progression speed varies greatly from person to person. General Progression Patterns Curve Severity Possible Progression Mild May remain stable Moderate Slow worsening over years Severe Faster progression possible In some adults, curves may worsen by 1–3 degrees annually, particularly when degeneration is advanced. Best Exercises for Adult Scoliosis Core Strengthening: Strong core muscles help stabilise the spine. Stretching Exercises: Stretching reduces muscular tightness and improves flexibility. Physiotherapy Programs: Targeted scoliosis rehabilitation can improve posture awareness and movement control. Yoga and Mobility Training: Gentle movement therapy may reduce stiffness and
Spine Clinic in Mumbai

Spine Clinic in Mumbai Are you searching for the best spine clinic in Mumbai? Look no further. Mumbai offers a wide range of specialized spine clinics dedicated to diagnosing, treating, and rehabilitating spinal disorders. With advanced medical facilities and expert spine specialists, these clinics ensure you receive world-class care. Why Choose a Spine Clinic in Mumbai? A spine clinic in Mumbai provides comprehensive care for various spinal conditions, including: Back pain Neck pain Sciatica Slipped (herniated) disc Scoliosis and kyphosis Spinal injuries and fractures These clinics combine advanced diagnostic tools, experienced specialists, and holistic treatment approaches to deliver exceptional results. Top Features of a Spine Clinic in Mumbai Expert Spine SpecialistsMumbai’s spine clinics are led by highly qualified spine surgeons such as Dr. Shekhar Bhojraj, Dr. Abhay Nene, and Dr. Priyank Patel. These specialists have years of experience and expertise in treating complex spinal disorders. Advanced Diagnostic ToolsModern spine clinics in Mumbai utilize advanced imaging technologies like MRI, CT scans, and digital X-rays for precise diagnosis and effective treatment planning. Personalized Treatment PlansEvery patient is unique, and clinics in Mumbai emphasize personalized care. From conservative treatments like physiotherapy to minimally invasive spine surgeries, the approach is tailored to individual needs. Minimally Invasive TechniquesFor patients requiring surgery, spine clinics in Mumbai specialize in minimally invasive spine procedures that reduce recovery time and minimize risks. Post-Treatment RehabilitationRehabilitation is a critical component of spinal care. Mumbai’s clinics offer physiotherapy and other rehabilitation services to ensure a complete and speedy recovery. Benefits of Visiting a Spine Clinic in Mumbai Access to some of the best spine specialists in India Comprehensive diagnostic and treatment options under one roof Advanced surgical techniques ensuring faster recovery Focus on non-surgical treatments wherever possible Post-treatment care for long-term spinal health Trusted Spine Clinics in Mumbai Some of the top-rated spine clinics in Mumbai include: We Are Spine A team of expert spine specialists offering holistic care. Lilavati Hospital Hinduja Hospital Offers advanced diagnostic and treatment options for various spinal conditions. Breach Candy Hospital Renowned for its experienced spine surgeons and exceptional patient care in treating complex spinal disorders. Breach Candy Hospital When to Visit a Spine Clinic in Mumbai You should consult a spine specialist if you experience: Persistent back or neck pain Numbness, tingling, or weakness in your arms or legs Difficulty walking or maintaining posture Loss of bladder or bowel control Timely treatment can prevent complications and improve your quality of life. When to Visit a Spine Clinic in Mumbai You should consult a spine specialist if you experience: Persistent back or neck pain Numbness, tingling, or weakness in your arms or legs Difficulty walking or maintaining posture Loss of bladder or bowel control Timely treatment can prevent complications and improve your quality of life. Conclusion Mumbai’s spine clinics are dedicated to providing top-tier care for all types of spinal conditions. With expert doctors, advanced technology, and patient-focused services, these clinics ensure you receive the best possible treatment. If you are looking for a reliable spine clinic in Mumbai, take the first step toward a healthier, pain-free life today. Please enable JavaScript in your browser to complete this form.Please enable JavaScript in your browser to complete this form.Full Name *Email *Phone Number * Submit
Top Spine Surgeons Mumbai

Top 10 Spine Surgeons in Mumbai If you are searching for the top 10 spine surgeons in Mumbai, it’s likely that you or a loved one are dealing with persistent back pain, slipped disc, spine deformity, or nerve-related issues. Choosing the right spine specialist can make a life-changing difference not only in treatment outcomes but also in avoiding unnecessary surgery.Mumbai is home to highly skilled, globally trained spine surgeons who offer advanced, patient-focused spine care. This guide highlights the top 10 spine surgeons in the city, helping you make an informed choice on your path to relief. Here is the List Top 10 spine surgeons in Mumbai 1. Dr. Shekhar Bhojraj Educational Distinction MBBS, MS (Orthopaedics), FCPS (ORTHO), D (ORTHO) AO Spine Fellowship University of Nottingham, UK AO Spine Fellowship AO spine fellowship Y. Cotrel Spine Fellowship Paris, France Kenton Leathermann Clinical Spine Fellowship University of Louisville Over 40+ Years of Experience Book your Appointment Dr. Shekhar Bhojraj is one of Mumbai’s leading and most dedicated spine surgeons, renowned for his expertise in treating a wide range of spinal deformities, including Scoliosis, Kyphosis, and Spondylolisthesis. As India’s first dedicated spine surgeon, he has decades of experience and has been associated with some of Mumbai’s most prestigious hospitals, including Lilavati Hospital, Breach Candy Hospital, and Hinduja National Hospital. Dr. Bhojraj made immense contributions to the field of spinal surgery through numerous publications in various prestigious international journals and through his office as the past president of the Association of Spine Surgeons of India. Furthermore, he is committed to provide spine care to the under-privileged sections of society as reflected in his position as President and Chief Trustee of The Spine Foundation. Moreover, he is committed to providing spine care to underprivileged sections of society reflected by his position as President and Chief Trustee of the Spine Foundation. Besides his clinical acumen, Dr. Bhojraj has always been patient-centric. Most of the patients have appreciated his meticulous and kind care. He is one of the top choices for patients with complex spinal conditions. 2. Dr. Abhay Nene Educational Distinction MBBS, MS – Orthopaedic ASSI-Dartmouth Spine Fellowship Dartmouth-Hitchcock Medical Center, New Hampshire, USA Ulm Germany, Training in Spine Rehabilitation and Sports Medicine 26+ Years Experience Book your Appointment Dr. Abhay Nene is a vastly experienced spine surgeon in Mumbai. He received education and training at some of the most esteemed centers of learning in Europe, the USA, Argentina, the UK, and Singapore. His cases have ranged from osteoporotic spine issues, spinal malignancy reconstruction, and pediatric spine abnormalities to tuberculosis of the spine, which equip him with the ability to plan treatments most appropriate for patients with different conditions. Apart from his clinical work, Dr. Nene is actively involved in academic and research activities. He serves as the prospective Asia Pacific Chair for AOSpine, a global academic spine care organization. He has also received various prestigious awards for his work in this field, such as a Scoliosis Research Society Scholarship and the international ISSLS Spine Fellow designation. The approach and expertise of Dr. Abhay Nene in advanced spine surgery techniques present an assurance for the best possible level of treatment to each patient, individually managed for satisfying diverse needs. 3. Dr. Premik Nagad Educational Distinction MBBS, DNB Orthopaedics SpineSmith International Spine Surgery Fellowship San Antonio / Bryan-College Station, Texas, USA Advanced Spine Fellowship P. D. Hinduja Hospital & MRC, Mumbai Over 20+ Years of Experience Mumbai Book your Appointment Dr. Premik Nagad is an experienced professional dedicated to achieving the best possible health outcome for his patients. He has experience with fellowships at really prestigious institutions like P.D. Hinduja Hospital, Rush Institute in Chicago, and Brazos Spine in Texas. He is currently practicing at Wockhardt Hospitals in Mumbai Central and heads the Spine Foundation Fellowship Programme. Dr. Nagad is known for his expertise in dealing with disorders relating to the spine, such as minimally invasive spine surgery, reconstructive spine surgery, and cervical spine surgery. His areas of expertise also include fractures, spinal stenosis, and herniated discs. Dr. Nagad combines vast experience with advanced training and dedication to quality patient care, which identifies him as one of the best choices to carry out spine surgery in Mumbai. 4. Dr. Sheetal Mohite Educational Distinction MBBS, DNB – Orthopaedics Spine Travelling Fellowship Oswestry, Cardiff, London, U.K. Scoliosis Research Society International Fellow Miami, Florida 25+ Years Experience Mumbai Book your Appointment Dr. Sheetal Mohite has established himself as a versatile specialist in both orthopedic and spine surgery through his rigorous and global training. His education from prestigious institutions in the UK, Germany, and United States exposed him to diverse perspectives for treating spinal disorders. With expertise spanning a wide range of spinal conditions, Dr. Mohite skillfully performs disc replacements, deformity corrections, and minimally invasive procedures. He notably corrected complex fractures with cutting-edge strategies. Currently practicing at eminent Mumbai hospitals including Lilavati and HN Reliance, Dr. Mohite brings pioneering spinal care to the city. Beyond skilled operations, he partakes in extensive research and educates communities about spine care. 5. Dr. Priyank Patel Educational Distinction MBBS, MS – Orthopaedics Fellowship in Spine Surgery University Hospital Wales and University Hospital Llandough, Cardiff, UKy Fellow in Spine Surgery Fortis Hospital, Mumbai 15+ Years Experience Mumbai Book your Appointment Dr. Priyank Patel is a spine surgeon practicing in Mumbai. After earning his medical degree from Maharashtra University of Health Sciences, he embarked on an internationally acclaimed surgical fellowship journey expanding his expertise. These notable programs incorporated specialized training in deformity correction techniques at the prestigious Royal Orthopaedic Hospital in Birmingham.He studied minimally invasive procedures in Chicago and oncological approaches in Bologna, Italy. His exceptional skills and dedication have attracted high-profile clientele from the city’s creative elite, including prominent Bollywood stars and members of beloved national cricket team seeking relief. However, what truly separates Dr. Patel is his philosophy that conservative options must be exhausted prior to any operation, ensuring each patient receives the most tailored treatment plan for their individual pathology. 6. Dr. Raghu Varma Educational
L4-L5 Disc Bulge Treatment Without Surgery: Safe & Effective Recovery Guide
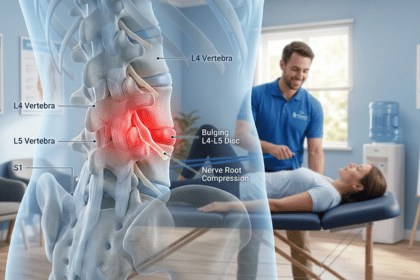
L4-L5 Disc Bulge Treatment Without Surgery: Safe & Effective Recovery Guide Lower back pain that radiates to your legs can disrupt daily life and one of the most common causes is an L4-L5 disc bulge. The good news? In most cases, you don’t need surgery. Understanding the right approach to L4-L5 disc bulge treatment without surgery can help you recover faster, reduce pain, and avoid complications. This guide explains proven, medically recommended non-surgical treatments that actually work. Direct Answer: L4-L5 Disc Bulge Treatment Without Surgery L4-L5 disc bulge treatment without surgery typically includes physiotherapy, medications, posture correction, lifestyle changes, and targeted exercises. Around 80–90% of patients improve with conservative treatment within a few weeks to months. What is an L4-L5 Disc Bulge? The L4-L5 disc is located in the lower lumbar spine and plays a key role in movement and weight-bearing. A disc bulge occurs when: The disc protrudes outward It presses on nearby nerves It causes pain, numbness, or weakness This makes L4-L5 disc bulge treatment without surgery essential for early recovery. Why Choose Non-Surgical Treatment? Most spine specialists recommend conservative care first. Benefits: Avoid surgical risks Lower cost Faster initial recovery Natural healing of the spine This is why L4-L5 disc bulge treatment without surgery is the preferred first-line approach. Best L4-L5 Disc Bulge Treatment Without Surgery 1. Physiotherapy (Most Effective Treatment) Physiotherapy is the cornerstone of L4-L5 disc bulge treatment without surgery. Key Components: Core strengthening exercises Flexibility training Posture correction McKenzie extension exercises Helps reduce pressure on the disc and improves spinal stability. 2. Medications for Pain Relief Doctors may prescribe: NSAIDs (reduce inflammation) Muscle relaxants Nerve pain medications These support L4-L5 disc bulge treatment without surgery by managing symptoms. 3. Activity Modification Avoid: Long sitting hours Heavy lifting Sudden twisting Instead: Stay active with light movements Take frequent breaks 4. Hot & Cold Therapy Ice packs reduce inflammation (early stage) Heat therapy relaxes muscles (later stage) 5. Ergonomic & Posture Correction Improving posture is critical in L4-L5 disc bulge treatment without surgery. Use: Lumbar support cushions Ergonomic chairs Standing desks 6. Epidural Steroid Injections (If Needed) Used when pain is severe Reduces nerve inflammation Provides temporary relief Comparison Table: Non-Surgical vs Surgical Treatment Factor Non-Surgical Treatment Surgery Risk Low Moderate Recovery Time 4–12 weeks 6–12 weeks Cost Lower Higher Effectiveness High (most cases) High (severe cases) First Option Yes No Advantages of L4-L5 Disc Bulge Treatment Without Surgery Preserves natural spine structure Lower complication risk Suitable for most patients Can be started immediately Encourages long-term spine health Limitations & Challenges While effective, L4-L5 disc bulge treatment without surgery has some limitations: Requires consistency and patience Pain relief may be gradual Not effective in severe nerve damage cases Lifestyle changes are mandatory Real-World Example Case A: A 35-year-old starts physiotherapy early → recovers in 6 weeks Case B: A 48-year-old delays care → needs injections after 3 months This highlights the importance of timely L4-L5 disc bulge treatment without surgery. Step-by-Step Recovery Plan Step 1: Diagnosis Clinical exam MRI if required Step 2: Pain Management Medications Ice/heat therapy Step 3: Start Physiotherapy Guided exercises Core strengthening Step 4: Lifestyle Changes Improve posture Avoid strain Step 5: Regular Follow-Up Track improvement Adjust treatment plan Exercises That Help (With Guidance) Pelvic tilts Cat-cow stretch Knee-to-chest stretch Core stabilization exercises Avoid exercises that strain the lower back. Frequently Asked Questions Can L4-L5 disc bulge heal without surgery? Yes, most cases improve with L4-L5 disc bulge treatment without surgery, including physiotherapy and lifestyle changes. How long does recovery take? Recovery typically takes 4 to 12 weeks, depending on severity. Can exercise fix a disc bulge? Yes, guided exercises are a key part of treatment. When is surgery needed? Only in severe cases with nerve damage or no improvement after months. Can I sit with an L4-L5 disc bulge? Yes, but limit duration and maintain proper posture. Yes, most cases improve with L4-L5 disc bulge treatment without surgery, including physiotherapy and lifestyle changes. Recovery typically takes 4 to 12 weeks, depending on severity. Yes, guided exercises are a key part of treatment. Only in severe cases with nerve damage or no improvement after months. Yes, but limit duration and maintain proper posture. Conclusion: Choose the Right L4-L5 Disc Bulge Treatment Without Surgery Choosing L4-L5 disc bulge treatment without surgery is the safest and most effective path for most patients. With the right combination of physiotherapy, posture correction, and guided care, recovery is not only possible, it’s highly likely.
L5 S1 Exercises to Avoid: Protect Your Spine from Further Damage

L5 S1 Exercises to Avoid: Protect Your Spine from Further Damage If you’ve been diagnosed with an L5-S1 disc bulge or herniation, exercise can either help your recovery or make things significantly worse. Many people unknowingly perform the wrong workouts, increasing pain and delaying healing. That’s why understanding L5 S1 exercises to avoid is just as important as knowing which exercises to do. This guide will clearly explain what movements to stay away from, why they’re harmful, and how to modify your routine safely. Direct Answer: L5 S1 Exercises to Avoid L5 S1 exercises to avoid include heavy lifting, deep forward bending, high-impact workouts, twisting movements, and sit-ups/crunches. These exercises increase pressure on the lower spine and can worsen disc bulge or nerve compression. Why Certain Exercises Are Dangerous for L5 S1 The L5-S1 disc carries maximum load and is highly sensitive to pressure. When you perform incorrect exercises: Disc pressure increases Nerve compression worsens Pain and inflammation flare up This is why avoiding harmful movements is essential during recovery. Top L5 S1 Exercises to Avoid 1. Sit-Ups and Crunches One of the most common mistakes. Puts excessive pressure on the lower spine Increases disc bulge risk Can worsen sciatica symptoms Heavy Weightlifting (Especially Deadlifts & Squats) These are major L5 S1 exercises to avoid if done incorrectly or during recovery. High spinal load Risk of improper form Sudden strain on discs Especially avoid: Barbell deadlifts Heavy squats Leg press with excessive weight Toe Touches & Deep Forward Bending Directly compresses the disc Increases bulge pressure Triggers nerve pain Twisting Exercises Movements like: Russian twists Golf swings (forceful rotation) Certain yoga twists These can aggravate the disc and worsen symptoms. High-Impact Activities Running on hard surfaces Jumping exercises HIIT workouts These create repetitive shock on the spine. Leg Raises (Straight Leg Lifts) Strains lower back muscles Pulls on lumbar spine Can increase nerve irritation Comparison Table: Safe vs Unsafe Exercises Category Avoid Safer Alternatives Core Crunches Planks (modified) Cardio Running Walking, cycling Strength Heavy squats Bodyweight exercises Flexibility Toe touches Gentle hamstring stretch Why Avoiding These Exercises Matters Following the right precautions around L5 S1 exercises to avoid can: Prevent worsening of disc bulge Reduce nerve compression Speed up recovery Avoid long-term complications Reduce risk of surgery Common Mistakes People Make Even with good intentions, many worsen their condition: Exercising through pain Copying generic YouTube workouts Ignoring posture Returning to gym too early Avoiding these mistakes is as important as avoiding wrong exercises. Limitations & Considerations Not all exercises are universally harmful Some movements may be safe under supervision Recovery stage matters Individual diagnosis differs Always consult a physiotherapist before restarting workouts. Real-World Example Case 1: A gym-goer continues deadlifts → pain worsens → recovery delayed Case 2: Another patient avoids risky movements → follows guided rehab → recovers faster This shows how understanding L5 S1 exercises to avoid directly impacts healing. Step-by-Step: Safe Exercise Approach Step 1: Stop Painful Movements: Immediately avoid exercises that trigger discomfort Step 2: Focus on Neutral Spine: Maintain correct posture during all activities Step 3: Start Gentle Exercises: Begin with physiotherapy-based movements Step 4: Gradual Progression: Increase intensity only under guidance Step 5: Monitor Symptoms: Stop if pain increases Frequently Asked Questions What exercises should I avoid with L5 S1 disc bulge? Key L5 S1 exercises to avoid include crunches, heavy lifting, twisting movements, and high-impact workouts. Can I go to the gym with L5 S1 disc bulge? Yes, but only with modified exercises and proper guidance. Can yoga worsen L5 S1 issues? Certain poses involving bending and twisting can worsen symptoms. What happens if I ignore precautions? You may worsen the disc bulge and delay healing. Key L5 S1 exercises to avoid include crunches, heavy lifting, twisting movements, and high-impact workouts. Yes, but only with modified exercises and proper guidance. Certain poses involving bending and twisting can worsen symptoms. You may worsen the disc bulge and delay healing. Conclusion: Avoid the Wrong Moves to Heal Faster Understanding L5 S1 exercises to avoid is crucial for protecting your spine and ensuring proper recovery. The wrong exercises can worsen your condition, while the right approach can significantly speed up healing. Recovery is not about doing more, it’s about doing what’s right.