Can Stress Cause Back Pain

Can Stress Cause Back Pain Many people experiencing ongoing discomfort often ask, can stress cause back pain, especially when no injury or obvious physical cause is present. Stress affects more than emotional well-being, it can directly influence muscle tension, posture, and pain perception. Back pain is one of the most common health complaints worldwide. While structural spine problems are well known, stress-related back pain is increasingly recognized as a real and medically valid condition. Understanding how stress affects the body can help individuals manage symptoms more effectively. Can Stress Cause Back Pain? What Medical Science Shows Yes, stress can cause back pain through multiple physiological pathways. When the body experiences stress, it activates the nervous system’s “fight-or-flight” response. This leads to the release of stress hormones such as cortisol and adrenaline. These hormones prepare the body for action but also cause muscles to tighten. When muscle tension becomes prolonged, especially in the neck, shoulders, and lower back, it can lead to pain, stiffness, and restricted movement. Over time, chronic stress may contribute to ongoing discomfort even without a visible spinal injury. How Stress Physically Triggers Back Pain Persistent Muscle Tension: Stress causes involuntary tightening of muscles. If this tension is not released, muscles may become fatigued, sore, or prone to spasms, especially in the lower back. Postural Changes: People under stress often adopt poor posture, such as slouching or hunching over screens. Poor posture increases pressure on spinal joints and discs, leading to discomfort over time. Altered Pain Perception: Stress affects how the brain processes pain signals. During periods of emotional stress, the body may become more sensitive to pain, making mild back discomfort feel more intense. Common Symptoms of Stress-Related Back Pain Individuals wondering can stress cause back pain often report: Dull or aching pain in the upper or lower back Muscle stiffness, especially after prolonged sitting Pain that worsens during emotionally stressful periods Tightness in the neck and shoulders along with back discomfort Temporary relief with rest, followed by recurrence during stress These symptoms may fluctuate depending on stress levels rather than physical activity. Stress and Pre-Existing Spine Conditions Stress alone does not usually damage the spine, but it can aggravate existing conditions such as: Degenerative disc disease Herniated or bulging discs Chronic lower back pain Muscle imbalance or weakness People with spine conditions may notice flare-ups during stressful life events, highlighting the strong connection between emotional stress and physical pain. When Back Pain Needs Medical Evaluation While stress-related back pain may improve with lifestyle changes, medical evaluation is important if: Pain lasts longer than two to three weeks Pain spreads to the arms or legs There is numbness, tingling, or weakness Back pain interferes with sleep or daily activities In such cases, imaging or specialist assessment may be required to rule out structural causes. Managing Stress to Help Reduce Back Pain Understanding can stress cause back pain helps individuals take preventive and supportive steps: Regular low-impact exercise such as walking or stretching Stress-reduction techniques like deep breathing or mindfulness Ergonomic workspaces to support spinal alignment Adequate sleep and scheduled breaks during the day Professional evaluation if symptoms persist Stress management works best when combined with appropriate medical guidance. Scientific and Medical Evidence Reputable medical institutions recognize the link between stress and musculoskeletal pain. Research shows that emotional stress can influence muscle tone, inflammation, and pain perception. At We Are Spine, we understand that back pain is not always purely physical stress and emotional factors can play a significant role. Our team of fellowship-trained spine specialists combines medical expertise with a holistic, patient-centered approach to help you address both the symptoms and underlying contributors to back discomfort. Your journey to a stronger spine and reduced stress begins with informed care, consult with our specialists at We Are Spine to take the first step toward lasting relief. Frequently Asked Questions (FAQs) Can stress cause back pain without physical injury? Yes. Stress can lead to muscle tension, posture changes, and heightened pain sensitivity, resulting in back pain even without injury. Is stress-related back pain serious? It can become serious if ignored, especially when it contributes to chronic pain or worsens existing spine conditions. Can stress make chronic back pain worse? If pain worsens during emotional stress and improves with relaxation or rest, stress may be a contributing factor. Should stress-related back pain be treated medically? If pain is persistent, severe, or affects daily life, medical evaluation is recommended to rule out structural causes. Yes. Stress can lead to muscle tension, posture changes, and heightened pain sensitivity, resulting in back pain even without injury. It can become serious if ignored, especially when it contributes to chronic pain or worsens existing spine conditions. If pain worsens during emotional stress and improves with relaxation or rest, stress may be a contributing factor. If pain is persistent, severe, or affects daily life, medical evaluation is recommended to rule out structural causes. Conclusion At We Are Spine, your journey toward a pain-free and active life begins with expert care. Backed by the legacy of ABC Spinecare LLP, our fellowship-trained spine specialists in Mumbai provide patient-centered, evidence-based treatment for a wide range of spinal conditions. With consultations and procedures conducted at leading hospitals such as Lilavati Hospital, Breach Candy Hospital, and P.D. Hinduja National Hospital, we combine advanced medical technology with personalized care plans tailored to your needs. If stress, chronic discomfort, or unexplained back pain is affecting your quality of life, seeking expert guidance can make all the difference. Consult the Spine specialists at We Are Spine to address both the physical and contributing factors of back pain and take the first step toward lasting relief. Please enable JavaScript in your browser to complete this form.Please enable JavaScript in your browser to complete this form.Full Name *Email *Phone Number * Submit
Top 10 Spine Surgeons in India

Top 10 Spine Surgeons in India When considering spinal care whether for back pain, herniated disc, scoliosis, spinal stenosis, or trauma, choosing the right specialist is essential. The top 10 spine surgeons in India represent the country’s most experienced and highly trained medical professionals in treating spine conditions through both surgical and non-surgical methods. Spine surgery involves intricate procedures on the spinal column, spinal cord, and nerve roots, and requires expertise in advanced techniques like minimally invasive spine surgery, spinal fusion, and deformity correction. This blog highlights information on the leading spine surgeons in India who have earned recognition for their training, clinical outcomes, and Here is the List Top 10 spine surgeons in India 1. Dr. Shekhar Bhojraj Educational Distinction MBBS, MS (Orthopaedics), FCPS (ORTHO), D (ORTHO) AO Spine Fellowship University of Nottingham, UK AO Spine Fellowship AO spine fellowship Y. Cotrel Spine Fellowship Paris, France Kenton Leathermann Clinical Spine Fellowship University of Louisville Over 40+ Years of Experience Book your Appointment Dr. Shekhar Bhojraj is one of Mumbai’s leading and most dedicated spine surgeons, renowned for his expertise in treating a wide range of spinal deformities, including Scoliosis, Kyphosis, and Spondylolisthesis. As India’s first dedicated spine surgeon, he has decades of experience and has been associated with some of Mumbai’s most prestigious hospitals, including Lilavati Hospital, Breach Candy Hospital, and Hinduja National Hospital. Dr. Bhojraj made immense contributions to the field of spinal surgery through numerous publications in various prestigious international journals and through his office as the past president of the Association of Spine Surgeons of India. Furthermore, he is committed to provide spine care to the under-privileged sections of society as reflected in his position as President and Chief Trustee of The Spine Foundation. Moreover, he is committed to providing spine care to underprivileged sections of society reflected by his position as President and Chief Trustee of the Spine Foundation. Besides his clinical acumen, Dr. Bhojraj has always been patient-centric. Most of the patients have appreciated his meticulous and kind care. He is one of the top choices for patients with complex spinal conditions. 2. Dr. Abhay Nene Educational Distinction MBBS, MS – Orthopaedic ASSI-Dartmouth Spine Fellowship Dartmouth-Hitchcock Medical Center, New Hampshire, USA Ulm Germany, Training in Spine Rehabilitation and Sports Medicine 26+ Years Experience Book your Appointment Dr. Abhay Nene is a vastly experienced spine surgeon in Mumbai. He received education and training at some of the most esteemed centers of learning in Europe, the USA, Argentina, the UK, and Singapore. His cases have ranged from osteoporotic spine issues, spinal malignancy reconstruction, and pediatric spine abnormalities to tuberculosis of the spine, which equip him with the ability to plan treatments most appropriate for patients with different conditions. Apart from his clinical work, Dr. Nene is actively involved in academic and research activities. He serves as the prospective Asia Pacific Chair for AOSpine, a global academic spine care organization. He has also received various prestigious awards for his work in this field, such as a Scoliosis Research Society Scholarship and the international ISSLS Spine Fellow designation. The approach and expertise of Dr. Abhay Nene in advanced spine surgery techniques present an assurance for the best possible level of treatment to each patient, individually managed for satisfying diverse needs. Dr. Abhay Nene, alumnus of T N Medical College, is a renowned Mumbai-based spine surgeon, Asia Pacific Chair of AOSpine, author of 50+ publications, and an avid athlete and educator in spinal care. 3. Dr. Premik Nagad Educational Distinction MBBS, DNB Orthopaedics SpineSmith International Spine Surgery Fellowship San Antonio / Bryan-College Station, Texas, USA Advanced Spine Fellowship P. D. Hinduja Hospital & MRC, Mumbai Over 20+ Years of Experience Mumbai Book your Appointment Dr. Premik Nagad is an experienced professional dedicated to achieving the best possible health outcome for his patients. He has experience with fellowships at really prestigious institutions like P.D. Hinduja Hospital, Rush Institute in Chicago, and Brazos Spine in Texas. He is currently practicing at Wockhardt Hospitals in Mumbai Central and heads the Spine Foundation Fellowship Programme. Dr. Nagad is known for his expertise in dealing with disorders relating to the spine, such as minimally invasive spine surgery, reconstructive spine surgery, and cervical spine surgery. His areas of expertise also include fractures, spinal stenosis, and herniated discs. Dr. Nagad combines vast experience with advanced training and dedication to quality patient care, which identifies him as one of the best choices to carry out spine surgery in Mumbai. 4. Dr. Sheetal Mohite Educational Distinction MBBS, DNB – Orthopaedics Spine Travelling Fellowship Oswestry, Cardiff, London, U.K. Scoliosis Research Society International Fellow Miami, Florida 25+ Years Experience Mumbai Book your Appointment Dr. Sheetal Mohite has established himself as a versatile specialist in both orthopedic and spine surgery through his rigorous and global training. His education from prestigious institutions in the UK, Germany, and United States exposed him to diverse perspectives for treating spinal disorders. With expertise spanning a wide range of spinal conditions, Dr. Mohite skillfully performs disc replacements, deformity corrections, and minimally invasive procedures. He notably corrected complex fractures with cutting-edge strategies. Currently practicing at eminent Mumbai hospitals including Lilavati and HN Reliance, Dr. Mohite brings pioneering spinal care to the city. Beyond skilled operations, he partakes in extensive research and educates communities about spine care. 5. Dr. Priyank Patel Educational Distinction MBBS, MS – Orthopaedics Fellowship in Spine Surgery University Hospital Wales and University Hospital Llandough, Cardiff, UKy Fellow in Spine Surgery Fortis Hospital, Mumbai 15+ Years Experience Mumbai Book your Appointment Dr. Priyank Patel is a spine surgeon practicing in Mumbai. After earning his medical degree from Maharashtra University of Health Sciences, he embarked on an internationally acclaimed surgical fellowship journey expanding his expertise. These notable programs incorporated specialized training in deformity correction techniques at the prestigious Royal Orthopaedic Hospital in Birmingham.He studied minimally invasive procedures in Chicago and oncological approaches in Bologna, Italy. His exceptional skills and dedication have attracted high-profile clientele from the city’s creative elite, including prominent Bollywood stars and members
Is Spine Surgery Safe?

Is Spine Surgery Safe? Spine surgery is often considered a last resort for people suffering from chronic back or neck pain, nerve compression, or spinal instability. For many patients, the very idea of surgery on the spine raises fear and uncertainty. A common and understandable question is: Is spine surgery safe? The short answer is yes, spine surgery is generally safe when properly indicated and performed by experienced Spine Specialists, but like any medical procedure, it carries certain risks. Understanding when spine surgery is needed, how safe it is today, and what factors influence outcomes can help patients make informed decisions. Why Is Spine Surgery Performed? Spine surgery is recommended when non-surgical treatments fail to provide relief or when there is a risk of permanent nerve damage. Common conditions that may require spine surgery include: Slipped or herniated disc Spinal stenosis Cervical or lumbar spondylosis with nerve compression Scoliosis or spinal deformities Spine tumors Spinal cord injuries Degenerative disc disease Most spine conditions are initially treated with medication, physiotherapy, lifestyle changes, and injections. Surgery is considered only when these approaches do not work or when symptoms worsen. How Safe Is Spine Surgery Today? Advances in medical technology, imaging, anesthesia, and surgical techniques have made spine surgery safer than ever before. Modern spine procedures often involve: minimally invasive spine surgery Improved surgical precision Real-time imaging guidance Better infection control Faster recovery protocols As a result, complication rates have significantly reduced compared to the past, especially in well-equipped centers with experienced spine surgeons. Common Risks of Spine Surgery Although spine surgery is generally safe, potential risks include: Infection Bleeding Nerve injury Persistent pain Blood clots Delayed healing It is important to note that serious complications are uncommon, especially when surgery is carefully planned and executed. Life After Spine Surgery Recovery depends on the type of surgery and individual health. Most patients: Resume light activities within weeks Begin physiotherapy soon after surgery Experience gradual improvement over months Long-term success depends on maintaining good posture, staying active, and following rehabilitation plans. Key Takeaway So, Is spine surgery safe? For most patients, the answer is YES, when done for the right reasons, by experienced and the best Spine Surgeons, and with proper preparation. Modern spine surgery has become significantly safer and more effective, helping many patients regain mobility, reduce pain, and improve quality of life. सायटिका आम है, लेकिन डराने वाली नहीं। सही जानकारी, समय पर निदान और उपचार से आप इसे नियंत्रित कर सकते हैं। याद रखें: जल्दी इलाज और सही मार्गदर्शन ही सबसे तेज़ राहत देता है। Frequently Asked Questions (FAQs) How painful is spine surgery? Spine surgery itself is performed under anesthesia, so there is no pain during the procedure. After surgery, patients may experience discomfort or soreness around the surgical area, especially in the first few days. However, pain is usually well controlled with medications, physiotherapy, and gradual movement. Most patients report that surgical pain reduces significantly within a few weeks. Can you live a normal life after spinal surgery? Yes, many patients return to a normal and active life after spinal surgery. Once the spine heals and rehabilitation is completed, daily activities such as walking, working, and light exercise become possible again. Long-term outcomes depend on the type of surgery, overall health, and how well post-surgery instructions and physiotherapy are followed. Can you climb stairs after spine surgery? Spine surgery may not be suitable for patients whose pain can be managed with non-surgical treatments like medication, physiotherapy, or lifestyle changes. People with severe medical conditions, poor bone health, or active infections may also not be ideal candidates. A spine specialist evaluates imaging, symptoms, and overall health before recommending surgery. Is spine surgery safe with modern techniques? Yes, spine surgery is generally safe today due to advances in medical technology, minimally invasive techniques, and improved imaging. These developments reduce surgical risks, blood loss, and recovery time. When performed by experienced spine surgeons, complication rates are relatively low. Spine surgery itself is performed under anesthesia, so there is no pain during the procedure. After surgery, patients may experience discomfort or soreness around the surgical area, especially in the first few days. However, pain is usually well controlled with medications, physiotherapy, and gradual movement. Most patients report that surgical pain reduces significantly within a few weeks. Yes, many patients return to a normal and active life after spinal surgery. Once the spine heals and rehabilitation is completed, daily activities such as walking, working, and light exercise become possible again. Long-term outcomes depend on the type of surgery, overall health, and how well post-surgery instructions and physiotherapy are followed. Spine surgery may not be suitable for patients whose pain can be managed with non-surgical treatments like medication, physiotherapy, or lifestyle changes. People with severe medical conditions, poor bone health, or active infections may also not be ideal candidates. A spine specialist evaluates imaging, symptoms, and overall health before recommending surgery. Yes, spine surgery is generally safe today due to advances in medical technology, minimally invasive techniques, and improved imaging. These developments reduce surgical risks, blood loss, and recovery time. When performed by experienced spine surgeons, complication rates are relatively low. Please enable JavaScript in your browser to complete this form.Please enable JavaScript in your browser to complete this form.Full Name *Email *Phone Number * Submit
How to cure cervical spondylosis permanently
How to cure cervical spondylosis permanently Cervical spondylosis is one of the most common causes of neck pain, stiffness, and nerve-related symptoms in adults. However, with increasing screen time, desk jobs, poor posture, and reduced physical activity, cervical spondylosis in young age is becoming increasingly common. Many people in their 30s and even late 20s are now being diagnosed with early degenerative changes in the cervical spine. In fact, the early signs of cervical spondylosis are often overlooked or mistaken for routine neck strain, leading many patients to ask an important question: How to cure cervical spondylosis permanently? To answer this honestly, it is important to understand what cervical spondylosis is, why it occurs, and what “permanent cure” actually means in medical terms. What Is Cervical Spondylosis? Cervical spondylosis refers to age-related degenerative changes in the cervical spine, which includes the seven vertebrae in the neck. Over time, the intervertebral discs lose hydration and elasticity, joints undergo wear and tear, and bone spurs (osteophytes) may form. These changes can: Reduce disc height Narrow nerve spaces Compress spinal nerves or the spinal cord Cause stiffness and pain Cervical spondylosis develops slowly and is considered a chronic degenerative condition, not an infection or injury. Can Cervical Spondylosis Be Cured Permanently? Cervical spondylosis cannot be permanently cured in the sense of reversing spinal degeneration. Once discs and joints undergo degenerative changes, they cannot return to their original state. However, cervical spondylosis can be effectively managed, symptoms can be controlled long-term, and progression can be slowed significantly. Many patients live pain-free, active lives by following the right treatment and lifestyle strategies. In medical practice, the goal is: Long-term pain relief Preservation of neck movement Prevention of nerve damage Avoidance of surgery whenever possible Common Symptoms of Cervical Spondylosis Symptoms vary depending on severity and nerve involvement. Common symptoms include: Chronic neck pain or stiffness Pain radiating to shoulders or arms Tingling or numbness in hands or fingers Headaches starting at the base of the skull Reduced neck mobility Muscle weakness in advanced cases Symptoms may worsen after long periods of sitting, mobile phone use, or poor sleeping posture, as shown in research on the effect of prolonged smartphone use on posture. Best Long-Term Treatments for Cervical Spondylosis 1. Posture Correction (Most Critical Factor) Poor posture is one of the biggest contributors to symptom progression. Forward head posture, slouching, and prolonged screen use increase stress on cervical discs. Corrective measures include: Keeping screens at eye level Avoiding bending the neck while using phones Sitting with proper back and neck support Maintaining neutral neck alignment Consistent posture correction can significantly reduce pain and prevent flare-ups. 2. Physiotherapy and Neck Exercises Physiotherapy is the cornerstone of long-term management. A trained physiotherapist designs exercises to: Strengthen neck and upper back muscles Improve flexibility and range of motion Reduce nerve compression Improve posture control Daily exercises, when done correctly, can reduce stiffness and pain over time and help prevent recurrence. 3. Lifestyle Modifications Small lifestyle changes play a big role in long-term relief: Take frequent breaks during desk work Avoid sudden neck movements Use a supportive pillow that maintains natural neck curvature Maintain a healthy weight Stay physically active Reducing prolonged static postures helps lower pressure on cervical discs. 4. Medications for Symptom Control Medications help manage pain during acute flare-ups but do not cure the condition. These may include: Anti-inflammatory medications Muscle relaxants Neuropathic pain medications Medications should always be used under medical supervision and are not meant for long-term dependency. 5. Cervical Collar (Short-Term Use Only) A soft cervical collar may be recommended during severe pain episodes to limit neck movement temporarily. However: Long-term use is discouraged Overuse can weaken neck muscles It should only be used for short durations when advised by a doctor. 6. Injection Therapy (Selective Cases) In cases of persistent nerve-related pain, cervical epidural steroid injections may help reduce inflammation and pain. These provide temporary relief and are used selectively when conservative treatment is insufficient. When Is Surgery Needed for Cervical Spondylosis? Surgery is not required for most patients and is considered only when symptoms do not improve with conservative care. In such cases, a specialist may evaluate different cervical spondylosis treatment options to determine whether surgical intervention is necessary. Surgery is typically recommended only when: Symptoms do not improve with conservative treatment Progressive nerve weakness develops There is spinal cord compression Balance or coordination is affected Surgical procedures aim to relieve nerve or spinal cord pressure, not cure degeneration. Can Cervical Spondylosis Improve Naturally? Yes, many people experience significant improvement with: Regular physiotherapy Correct posture Consistent exercise Lifestyle changes Symptoms often come in cycles, and with proper care, patients can remain symptom-free for long periods. How to Prevent Cervical Spondylosis From Worsening Although aging cannot be stopped, progression can be slowed by: Maintaining neck muscle strength Staying physically active Avoiding smoking Managing stress Sleeping in a neutral neck position Prevention plays a crucial role in long-term comfort. Key Takeaway How to Cure Cervical Spondylosis Permanently is a common question, but the truth is that cervical spondylosis cannot be cured permanently. However, it does not have to control your life. With early diagnosis, physiotherapy, posture correction, and healthy lifestyle changes, most people achieve long-term relief and maintain normal daily activities without the need for surgery. Long-term relief is possible when the condition is managed through the right cervical spondylosis treatment approach based on individual spine health. Frequently Asked Questions (FAQs) Is cervical spondylosis permanent? Cervical spondylosis is a degenerative condition, meaning the structural changes in the spine are permanent. However, symptoms are not always permanent. With proper posture, physiotherapy, lifestyle changes, and medical care, many people experience long periods without pain or stiffness. Can cervical spondylosis affect the brain? Cervical spondylosis does not directly affect the brain, but severe cases may compress the spinal cord or nearby nerves, leading to symptoms such as dizziness, headaches, balance problems, or coordination issues. These symptoms occur due to nerve involvement, not because the brain itself is damaged. What is the best sleeping position for cervical pain? The best
Top 5 Spine Surgeon in India

Top 5 Spine Surgeon in India If you are searching for the top 5 spine surgeon in India, chances are you or a loved one is dealing with persistent back pain, a slipped disc, spine deformity, or nerve-related symptoms. Choosing the best spine doctor in India can make a life-changing difference, not just in treatment outcomes, but also in avoiding unnecessary surgery. India is home to globally trained spine surgeons who offer advanced, patient-centric spine care. This guide helps you understand your options and take the right next step toward relief by connecting you with the best spine doctors in India. How We Identify the Top Spine Surgeons in India We consider the following factors while identifying reputed spine surgeons: 15+ years of focused spine surgery experience International fellowships and advanced training Association with reputed hospitals Expertise in both surgical and non-surgical spine care Patient-first and ethical treatment approach Here is the List Top 5 spine surgeon in India 1. Dr. Shekhar Bhojraj Educational Distinction MBBS, MS (Orthopaedics), FCPS (ORTHO), D (ORTHO) AO Spine Fellowship University of Nottingham, UK AO Spine Fellowship AO spine fellowship Y. Cotrel Spine Fellowship Paris, France Kenton Leathermann Clinical Spine Fellowship University of Louisville Over 40+ Years of Experience Book your Appointment Dr. Shekhar Bhojraj is one of the most respected names in Indian spine surgery and is widely known as India’s first dedicated spine surgeon. With over four decades of experience, he specializes in treating complex spinal deformities such as scoliosis, kyphosis, and spondylolisthesis. Dr. Bhojraj has been associated with leading hospitals such as Lilavati Hospital, Breach Candy Hospital, and Hinduja National Hospital. He is the Past President of the Association of Spine Surgeons of India and currently serves as President & Chief Trustee of The Spine Foundation, reflecting his commitment to ethical and inclusive spine care. 2. Dr. Abhay Nene Educational Distinction MBBS, MS – Orthopaedic ASSI-Dartmouth Spine Fellowship Dartmouth-Hitchcock Medical Center, New Hampshire, USA Ulm Germany, Training in Spine Rehabilitation and Sports Medicine 26+ Years Experience Book your Appointment Dr. Abhay Nene is a highly trained spine surgeon with international exposure across the USA, Europe, UK, Argentina, and Singapore. His expertise covers a wide range of spine conditions including osteoporotic spine disorders, pediatric spine problems, spinal infections, malignancy reconstruction, and tuberculosis of the spine. Dr. Nene is actively involved in research and academics and serves as the Prospective Asia Pacific Chair for AOSpine, a global spine organization. 3. Dr. Premik Nagad Educational Distinction MBBS, DNB Orthopaedics SpineSmith International Spine Surgery Fellowship San Antonio / Bryan-College Station, Texas, USA Advanced Spine Fellowship P. D. Hinduja Hospital & MRC, Mumbai Over 20+ Years of Experience Mumbai Book your Appointment Dr. Premik Nagad is known for combining advanced training with compassionate patient care. He has trained at leading institutions such as P. D. Hinduja Hospital, Rush Institute (Chicago), and Brazos Spine (Texas). He currently practices at Wockhardt Hospitals, Mumbai Central, and heads the Spine Foundation Fellowship Programme. 4. Dr. Sheetal Mohite Educational Distinction MBBS, DNB – Orthopaedics Spine Travelling Fellowship Oswestry, Cardiff, London, U.K. Scoliosis Research Society International Fellow Miami, Florida 25+ Years Experience Mumbai Book your Appointment Dr. Sheetal Mohite has received advanced spine training in the UK, Germany, and the USA. His expertise spans disc replacement, deformity correction, minimally invasive spine surgery, and complex fracture management. He is currently associated with Lilavati Hospital and HN Reliance Hospital and is actively involved in spine research and public education. 5. Dr. Priyank Patel Educational Distinction MBBS, MS – Orthopaedics Fellowship in Spine Surgery University Hospital Wales and University Hospital Llandough, Cardiff, UKy Fellow in Spine Surgery Fortis Hospital, Mumbai 15+ Years Experience Mumbai Book your Appointment Dr. Priyank Patel is internationally trained in spine surgery with fellowships in the UK and India. His training includes deformity correction at the Royal Orthopaedic Hospital, Birmingham, minimally invasive techniques in Chicago, and oncological spine approaches in Bologna, Italy. What sets him apart is his strong belief that conservative treatment should always be explored before surgery, ensuring personalized and ethical care. Best Spine Surgeon in Mumbai Many of the above doctors are recognized as leading spine surgeons making it easier for patients in and around Mumbai to access advanced spine care. Explore more: Spine Surgeon in Mumbai When Should You Consult a Spine Specialist Doctor? You should consult a spine specialist doctor if you experience: Back or neck pain lasting more than 2–3 weeks Pain radiating to arms or legs Numbness, tingling, or weakness Difficulty walking or maintaining balance Spine injury due to accident or fall If you are searching for the top 5 spine surgeons in India, chances are you or a loved one is dealing with persistent back pain, a slipped disc, spine deformity, or nerve-related symptoms. Choosing the best spine doctor in India can make a life-changing difference, not just in treatment outcomes, but also in avoiding unnecessary surgery. Frequently Asked Questions (FAQs) What is the success rate of spine surgery in India? The success rate of spine surgery in India is generally high, especially when performed by an experienced spine specialist doctor in a well-equipped hospital. For common procedures such as disc surgery or decompression, success rates are often 80–95%, depending on the condition, overall health of the patient, and post-surgery rehabilitation. Proper diagnosis and choosing the right surgeon play a major role in outcomes. The success rate of spine surgery in India is generally high, especially when performed by an experienced spine specialist doctor in a well-equipped hospital. For common procedures such as disc surgery or decompression, success rates are often 80–95%, depending on the condition, overall health of the patient, and post-surgery rehabilitation. Proper diagnosis and choosing the right surgeon play a major role in outcomes. What should be avoided after spine surgery? Heavy lifting or bending, Sudden twisting movements, Sitting or standing for long periods without breaks, Ignoring physiotherapy or follow-up visits Heavy lifting or bending, Sudden twisting movements, Sitting or standing for long periods without breaks, Ignoring physiotherapy or
Ankylosing Spondylitis Symptoms
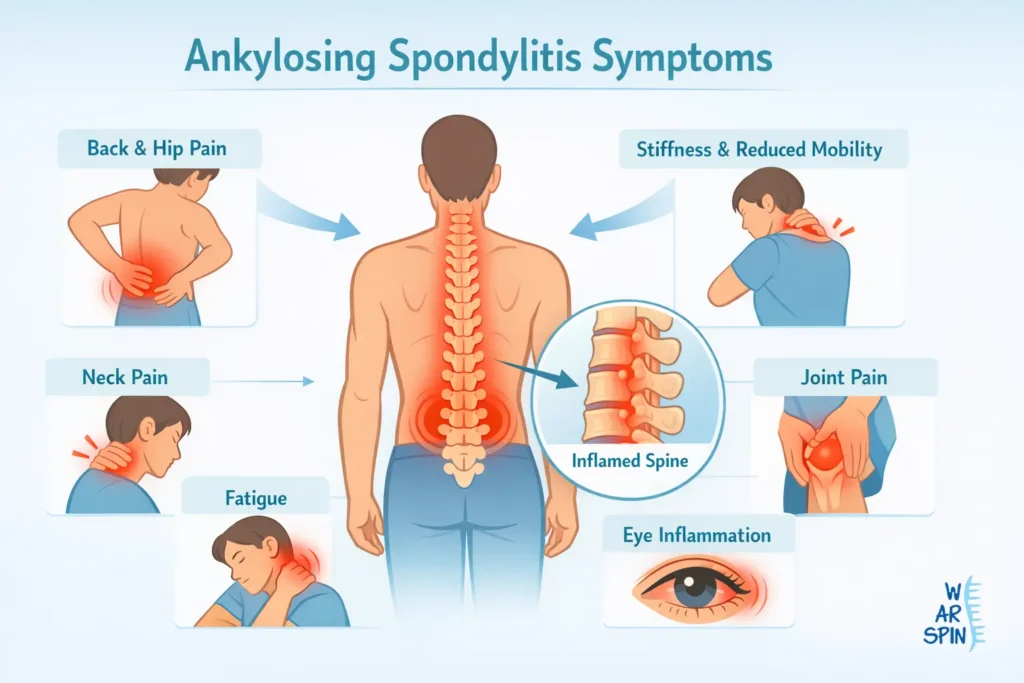
Ankylosing Spondylitis Symptoms Ankylosing spondylitis (AS) is a chronic inflammatory condition that primarily affects the spine and sacroiliac joints. Over time, it can lead to pain, stiffness, reduced mobility, and in severe cases, fusion of spinal bones. Because early symptoms often resemble common back problems, diagnosis is frequently delayed. Understanding ankylosing spondylitis symptoms is essential for early detection, timely ankylosing spondylitis treatment, and preventing long-term complications. What Is Ankylosing Spondylitis? Ankylosing spondylitis is a type of inflammatory arthritis that mainly affects the spine. Inflammation usually begins in the sacroiliac joints, where the spine meets the pelvis, and may gradually move upward. Over time, chronic inflammation can cause: Persistent pain and stiffness Reduced spinal flexibility Fusion of vertebrae (ankylosis) AS often begins in early adulthood, typically between ages 20 and 40 Why Early Ankylosing Spondylitis Symptoms Are Often Missed Early ankylosing spondylitis symptoms are frequently mistaken for: Muscle strain Poor posture Mechanical lower back pain Disc-related issues Unlike common back pain, AS-related pain is inflammatory, not mechanical. Because symptoms may come and go, many people delay medical evaluation for years. Early Ankylosing Spondylitis Symptoms 1. Chronic Lower Back Pain: The most common early sign is persistent lower back pain that: Lasts longer than 3 months Starts gradually rather than suddenly Improves with movement or exercise Worsens with rest This pattern is a key feature distinguishing AS from routine back pain. 2. Morning Stiffness: Morning stiffness lasting more than 30–60 minutes is a hallmark symptom. People often report: Difficulty bending after waking up Stiffness that eases as the day progresses Increased discomfort after prolonged sitting 3. Pain in the Buttocks or Hips: Inflammation of the sacroiliac joints can cause: Deep buttock pain Hip discomfort Alternating pain from one side to the other 4. Fatigue: Chronic inflammation can lead to: Persistent tiredness Low energy levels Reduced stamina Advanced Ankylosing Spondylitis Symptoms 1. Reduced Spinal Flexibility: Ongoing inflammation can limit spinal movement, leading to: Difficulty bending forward Reduced ability to twist Stiff, inflexible posture 2. Neck and Upper Back Pain: Ongoing inflammation can limit spinal movement, leading to: Difficulty bending forward Reduced ability to twist Stiff, inflexible posture Neck stiffness caused by ankylosing spondylitis may resemble cervical spondylosis, especially in early stages. 3. Stooped or Forward-Bending Posture: In advanced cases, fusion of vertebrae may cause: Fixed forward-bending posture Loss of natural spinal curves Difficulty maintaining balance Ankylosing Spondylitis Symptoms Females vs Males Historically, ankylosing spondylitis was considered more common in men. However, recent research shows that ankylosing spondylitis symptoms females may be different rather than less severe, leading to underdiagnosis. How Symptoms Often Present in Females Women with AS may experience: More neck, shoulder, and upper back pain Less obvious spinal fusion on imaging Greater fatigue compared to men More peripheral joint pain (hips, knees, ankles) Because symptoms may not fit the “classic” male presentation, diagnosis in females is often delayed. Why Diagnosis Is Delayed in Females Symptoms may be mistaken for fibromyalgia or mechanical back pain Imaging changes may appear later Pain distribution may be less localized to the lower spine Recognizing ankylosing spondylitis symptoms females is critical for early intervention and better outcomes. Conclusion Recognizing ankylosing spondylitis symptoms early can prevent long-term spinal damage and disability. Persistent inflammatory back pain, morning stiffness, fatigue, and reduced mobility should never be ignored especially in young adults. Awareness of ankylosing spondylitis symptoms females is equally important, as differences in presentation often lead to delayed diagnosis. With early medical evaluation and appropriate treatment, many people with AS can maintain mobility, function, and quality of life. Frequently Asked Questions (FAQs) What is the life expectancy of someone with ankylosing spondylitis? Most people with ankylosing spondylitis have a normal or near-normal life expectancy. With early diagnosis, regular treatment, and proper management of inflammation, serious complications can often be prevented. In rare cases, severe disease or untreated complications may slightly affect longevity, but this is uncommon with modern medical care. What is the main cause of ankylosing spondylitis? The exact cause of ankylosing spondylitis is not fully understood, but it is strongly linked to genetic factors, particularly the HLA-B27 gene. Not everyone with this gene develops the condition, suggesting that environmental and immune system factors also play a role in triggering inflammation. What is the main cause of ankylosing spondylitis? The exact cause of ankylosing spondylitis is not fully understood, but it is strongly linked to genetic factors, particularly the HLA-B27 gene. Not everyone with this gene develops the condition, suggesting that environmental and immune system factors also play a role in triggering inflammation. Can I live a normal life with ankylosing spondylitis? Yes, many people with ankylosing spondylitis live active and productive lives. Early treatment, regular exercise, good posture habits, and medical follow-up help control symptoms, maintain mobility, and prevent long-term spinal damage. Disease severity varies, and symptoms can often be managed effectively. Does ankylosing spondylitis go away? Ankylosing spondylitis is a chronic condition, meaning it does not completely go away. However, symptoms can go into remission, where pain and stiffness are minimal or absent for long periods. Proper treatment can significantly slow disease progression and reduce flare-ups. What can be mistaken for ankylosing spondylitis? Ankylosing spondylitis (AS) can sometimes be mistaken for other conditions because its early symptoms, such as back pain and stiffness, are common in many disorders. Mechanical or nonspecific back pain caused by muscle strain, poor posture, or disc problems can mimic AS. Similarly, a slipped disc (herniated disc) may cause localized or radiating pain that resembles inflammatory back pain. Most people with ankylosing spondylitis have a normal or near-normal life expectancy. With early diagnosis, regular treatment, and proper management of inflammation, serious complications can often be prevented. In rare cases, severe disease or untreated complications may slightly affect longevity, but this is uncommon with modern medical care. The exact cause of ankylosing spondylitis is not fully understood, but it is strongly linked to genetic factors, particularly the HLA-B27 gene. Not everyone with this gene develops the condition, suggesting that environmental and immune system factors also play a role in triggering inflammation. The exact cause
Slipped Disc Symptoms
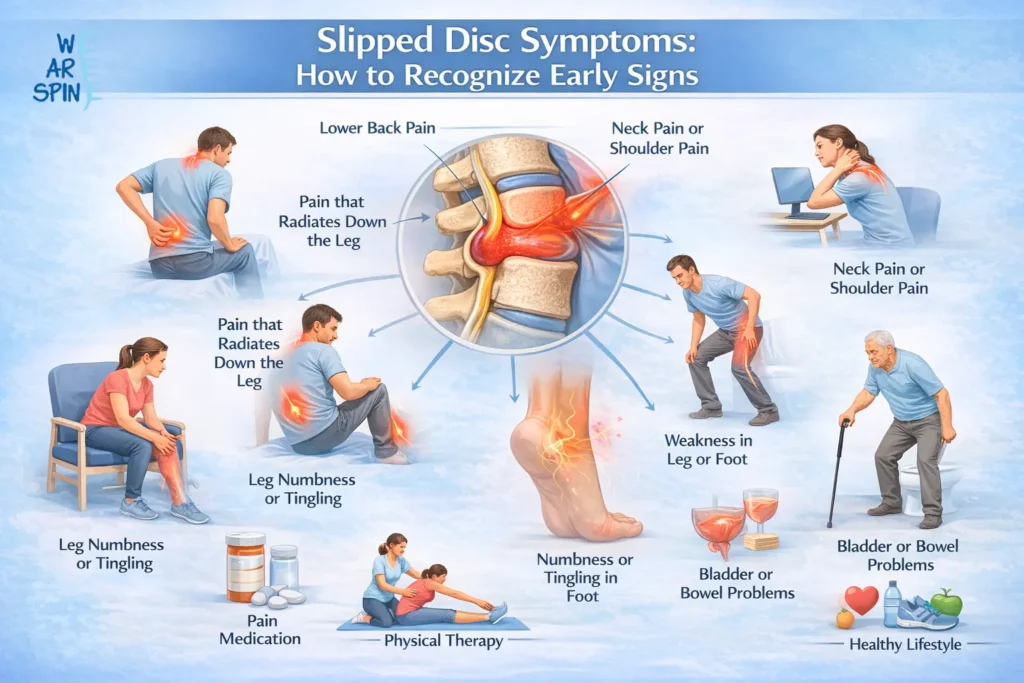
Slipped Disc Symptoms A slipped disc, also known as a herniated disc, is a common spinal condition that occurs when the soft inner gel of a spinal disc protrudes through the tougher outer layer. This can irritate nearby nerves and cause pain, numbness, or weakness in different parts of the body. Understanding the slipped disc symptoms is crucial for early diagnosis and timely treatment. Many people dismiss early signs as simple back strain or fatigue, which can delay care and lead to complications. This blog will help you identify the early warning signs, understand the risks, and know when to seek medical attention. What Is a Slipped Disc? The spine consists of vertebrae separated by intervertebral discs, which act as shock absorbers and provide flexibility. When a disc bulges or ruptures, it is referred to as a slipped disc. This can compress nearby spinal nerves, causing pain, numbness, tingling, or weakness. Slipped discs can occur anywhere along the spine: cervical (neck), thoracic (mid-back), or lumbar (lower back). The lumbar region is the most commonly affected area due to its load-bearing role. In severe cases, symptoms may resemble spinal stenosis or sciatica. Causes and Risk Factors A slipped disc can result from degeneration, injury, or lifestyle factors. Key causes and risk factors include: Age-related wear and tear: Discs lose flexibility and water content as we age, making them more prone to herniation. Poor posture: Slouching while sitting or standing increases stress on the spine. Repetitive lifting or twisting: Improper lifting techniques can strain discs. Obesity: Excess weight places additional pressure on spinal discs, particularly in the lower back. Sedentary lifestyle: Weak core and back muscles provide less support to the spine. Genetic predisposition: Some people inherit weaker discs or connective tissues, increasing vulnerability. For risk management, consult our spine specialists for evaluation. Common Slipped Disc Symptoms Symptoms may vary depending on the disc’s location and severity. Common slipped disc symptoms include: Localized pain: Aching or sharp pain at the site of the affected disc. Radiating pain: Pain that spreads to arms, hands, buttocks, or legs due to nerve compression. Numbness or tingling: A “pins and needles” sensation along the affected nerve. Muscle weakness: Difficulty lifting objects or performing routine activities. Limited mobility: Trouble bending, twisting, or standing for long periods. Pain aggravated by sitting or bending: Discomfort increases with certain positions. Many of these symptoms are similar to cervical spondylosis or ankylosing spondylitis, making accurate diagnosis essential. Symptoms by Location 1. Lumbar (Lower Back) Slipped Disc: The lower back is most prone to slipped discs. Symptoms include: Pain radiating down one or both legs (sciatica) Tingling or numbness in the legs or feet Muscle weakness in the legs, making walking or climbing stairs difficult Lower back stiffness and reduced flexibility Symptoms may resemble spinal stenosis or spondylolisthesis. 2. Thoracic (Mid Back) Slipped Disc Less common but still significant, mid-back herniations can lead to: Upper or mid-back pain Pain radiating around the chest or rib cage Tingling or numbness in the torso Muscle weakness affecting posture or stability Misdiagnosis may occur with kyphosis or spinal deformities. 3. Thoracic (Mid Back) Slipped Disc Less common but still significant, mid-back herniations can lead to: Upper or mid-back pain Pain radiating around the chest or rib cage Tingling or numbness in the torso Muscle weakness affecting posture or stability Misdiagnosis may occur with kyphosis or spinal deformities. Complications if Untreated Ignoring slipped disc symptoms can lead to: Chronic back pain Muscle weakness or atrophy Nerve damage leading to permanent numbness Reduced mobility and daily activity limitations Potential impact on bladder or bowel control Severe cases should be evaluated immediately by spine surgeons in Mumbai. Warning Signs That Require Immediate Medical Attention Seek urgent care if you notice: Loss of bladder or bowel control Severe leg or arm weakness Progressive numbness in limbs or groin area Inability to walk or maintain balance Severe pain not relieved by rest If symptoms persist, book a consultation for evaluation. Conclusion Recognizing slipped disc symptoms early is vital for effective treatment and avoiding complications. Persistent pain, tingling, numbness, or weakness should not be ignored. Early evaluation, diagnosis, and treatment by trained specialists can help maintain mobility, reduce pain, and improve quality of life. For more information, visit We Are Spine for a personalized consultation. Frequently Asked Questions (FAQs) How to heal a slipped disc? Most slipped discs heal with rest, physical therapy, and pain management. Short-term rest, anti-inflammatory medication, and exercises to strengthen the back and core help recovery. Surgery is rarely needed. How do I know if I’ve slipped a disc? Signs include persistent back pain, pain radiating to the arms or legs, numbness or tingling, and muscle weakness. A doctor may confirm with MRI, X-ray, or nerve tests. How long does a slipped disc last? Mild cases often improve in 4–6 weeks. Moderate or severe herniations can take 3–6 months, depending on treatment and lifestyle adjustments. What are the main causes of a slipped disc? Common causes include age-related degeneration, poor posture, repetitive lifting, injury, sedentary lifestyle, and obesity. Genetics may also increase risk. How can I test for a slipped disc at home? Common causes include age-related degeneration, poor posture, repetitive lifting, injury, sedentary lifestyle, and obesity. Genetics may also increase risk. Most slipped discs heal with rest, physical therapy, and pain management. Short-term rest, anti-inflammatory medication, and exercises to strengthen the back and core help recovery. Surgery is rarely needed. Signs include persistent back pain, pain radiating to the arms or legs, numbness or tingling, and muscle weakness. A doctor may confirm with MRI, X-ray, or nerve tests. Mild cases often improve in 4–6 weeks. Moderate or severe herniations can take 3–6 months, depending on treatment and lifestyle adjustments. Common causes include age-related degeneration, poor posture, repetitive lifting, injury, sedentary lifestyle, and obesity. Genetics may also increase risk. Common causes include age-related degeneration, poor posture, repetitive lifting, injury, sedentary lifestyle, and obesity. Genetics may also increase risk. Please enable JavaScript in your browser to complete this form.Please enable JavaScript in your browser to complete this form.Full Name *Email *Phone Number * Submit
First symptoms of spinal cancer
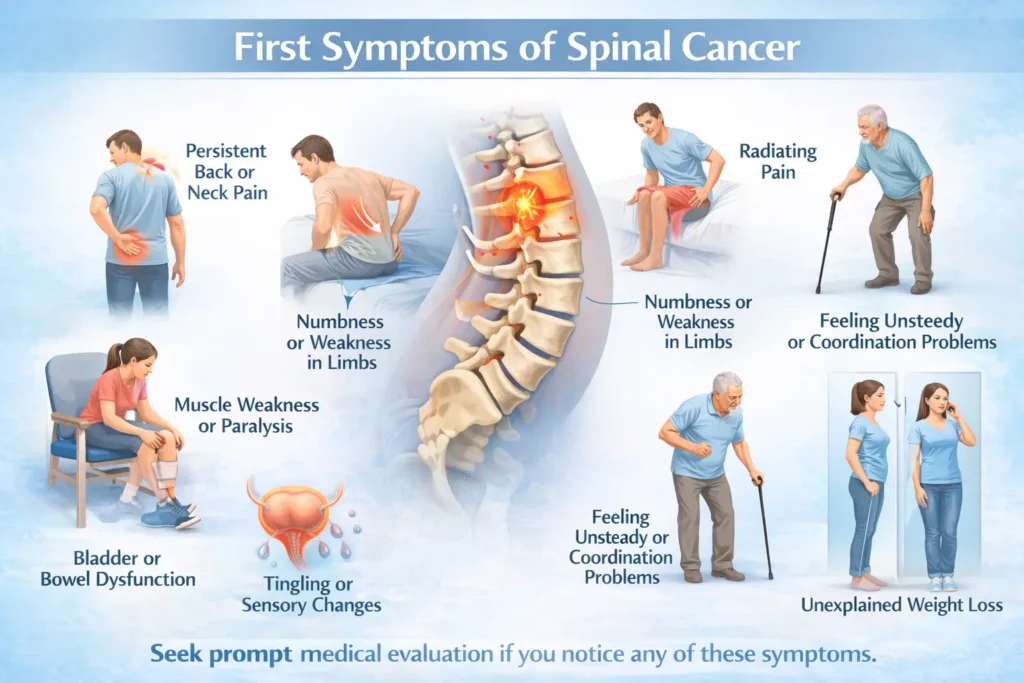
First symptoms of spinal cancer Spinal cancer is a rare but serious condition that occurs when abnormal cells grow within the spine or spinal cord. It may originate in the spine itself (primary spinal cancer) or spread from another part of the body (secondary or metastatic spinal cancer). One of the biggest challenges with spinal cancer is that early symptoms are often subtle and easily mistaken for common back problems. Understanding the first symptoms of spinal cancer is critical for early diagnosis, timely treatment, and better outcomes. This blog explains the early warning signs in a clear, factual, and medically accurate way. What Is Spinal Cancer? Spinal cancer refers to tumors that develop in or around: The vertebrae (spinal bones) The spinal cord Spinal nerves Surrounding tissues https://youtu.be/-T7BmXxWcWs?si=3CPjvHSOLyAhX6Bm Spinal cancer is often referred to clinically as a spine tumour treatment, which may develop within the spinal cord, vertebrae, or surrounding tissues. Tumors may be benign (non-cancerous) or malignant (cancerous). Even benign tumors can cause serious problems if they compress the spinal cord or nerves. Why Early Symptoms Are Often Missed In the early stages, spinal cancer symptoms may resemble: Muscle strain Degenerative spine disease Disc problems Age-related back pain Early spinal cancer symptoms are sometimes mistaken for age-related conditions such as cervical spondylosis, especially when neck pain and stiffness are present. Chronic back pain related to spinal cancer is sometimes wrongly attributed to osteoarthritis, particularly in older adults. First Symptoms of Spinal Cancer 1. Persistent Back Pain That Does Not Improve The most common and earliest symptom of spinal cancer is persistent back pain. Red flags include: Pain that lasts for weeks or months Pain that does not improve with rest or medication Pain that worsens over time Pain that is more severe at night or wakes you from sleep Unlike mechanical back pain, cancer-related pain is often deep, constant, and progressive. Persistent back pain related to spinal tumors is often misdiagnosed initially as a slipped disc due to overlapping pain patterns. Inflammatory back pain caused by spinal tumors may mimic symptoms of ankylosing spondylitis, especially when stiffness is worse at night. 2. Night Pain or Pain at Rest Back pain that becomes worse at night or while lying down is an important warning sign. This occurs because: Tumor-related inflammation increases at rest Pressure on spinal structures is constant, not movement-related Night pain should always be medically evaluated, especially when it is persistent. 3. Unexplained Weight Loss and Fatigue Systemic symptoms may appear early, particularly in malignant or metastatic spinal cancer. These include: Unintentional weight loss Persistent fatigue Loss of appetite General weakness These symptoms suggest that the body is under stress from an underlying disease process. 4. Numbness, Tingling, or Altered Sensation As a spinal tumor grows, it may compress nearby nerves or the spinal cord. Early neurological symptoms include: Tingling or pins-and-needles sensation Numbness in the arms, hands, legs, or feet Sensory changes on one side or both sides of the body These symptoms often start mildly and worsen gradually. Nerve compression from a spinal tumor can cause leg pain and tingling similar to sciatica. 5. Weakness in the Arms or Legs Muscle weakness is a serious early sign of spinal cord or nerve compression. You may notice: Difficulty gripping objects Trouble lifting arms Weak or heavy legs Difficulty climbing stairs Progressive compression of the spinal cord can lead to symptoms similar to a spinal cord injury, including weakness and loss of coordinati 6. Difficulty Walking or Balance Problems Spinal cancer affecting the spinal cord can disrupt coordination and balance. Early signs include: Unsteady walking Frequent stumbling Loss of coordination Feeling of stiffness or heaviness in the legs Gait imbalance caused by spinal tumors may resemble symptoms seen in spinal stenosis, leading to delayed diagnosis. 7. Changes in Bladder or Bowel Function Although this usually occurs in more advanced stages, it can sometimes appear early and should be treated as a medical emergency. Warning signs include: Difficulty controlling urination Urinary retention Bowel incontinence Numbness in the groin or saddle area These symptoms indicate significant spinal cord compression. First Symptoms of Spinal Cancer vs Common Back Pain Feature Common Back Pain Spinal Cancer Pain Improves with rest Yes No Worse at night Rare Common Progressive No Yes Neurological symptoms Rare Common Associated weight loss No Possible When to See a Doctor Immediately Seek medical evaluation if you experience: Persistent back pain lasting more than a few weeks Back pain with night worsening Numbness, weakness, or balance issues Unexplained weight loss Bladder or bowel changes Early imaging and diagnosis can prevent permanent neurological damage. If you notice persistent back pain, weakness, or numbness, it is important to speak with our spine experts for a timely evaluation. How Is Spinal Cancer Diagnosed? Diagnosis may involve: MRI of the spine CT scan or X-rays Blood tests Biopsy (if needed) Early diagnosis significantly improves treatment options and outcomes. Final Thoughts The first symptoms of spinal cancer are often subtle and easily overlooked. Persistent back pain, night pain, unexplained weight loss, numbness, weakness, and balance problems should never be ignored especially when they worsen over time. While spinal cancer is rare, early recognition of warning signs and prompt medical evaluation are crucial. If symptoms feel unusual, persistent, or progressive, seeking timely medical advice can make a life-changing difference. Frequently Asked Questions (FAQs) What are the first signs of spinal cancer? Early signs may include persistent back pain, numbness or tingling in the limbs, weakness, and difficulty walking. Pain is often worse at night or does not improve with rest. Can spinal cancer be cured? Treatment depends on the type, location, and stage. Some spinal cancers can be cured with surgery, radiation, or chemotherapy, while others can be controlled to relieve symptoms and slow progression. What age do people get spinal tumors? Spinal tumors can occur at any age, but they are most commonly diagnosed in adults between 40 and 70. Certain types are more common in children or younger adults. Would spinal cancer show in a blood test? There is no routine blood
Causes of Scoliosis
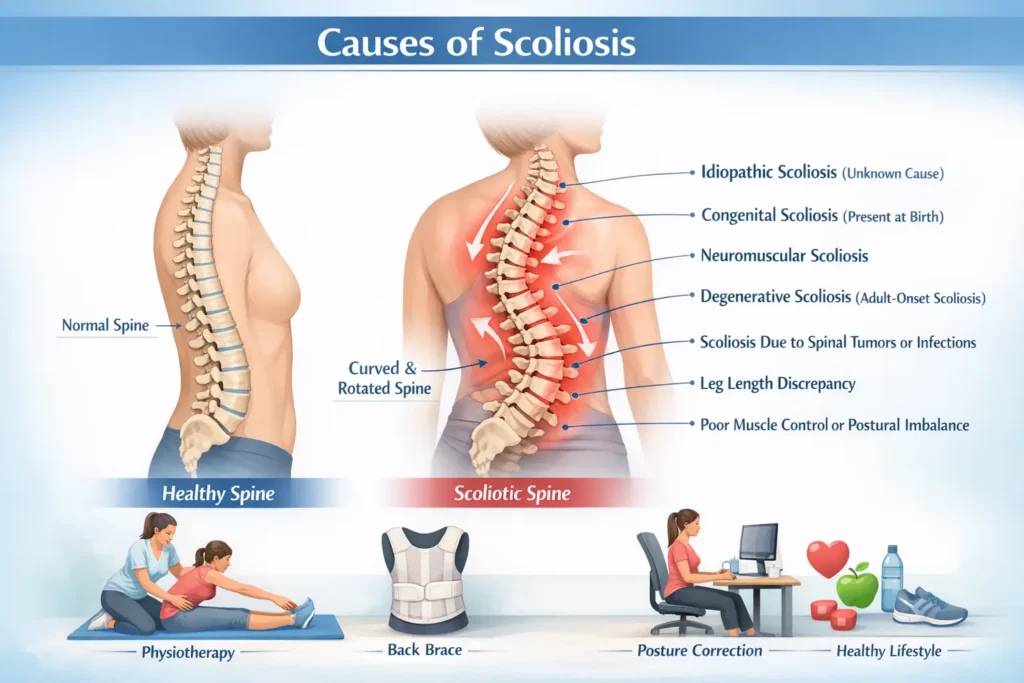
Causes of Scoliosis Scoliosis is a spinal condition in which the spine curves sideways in an abnormal “S” or “C” shape when viewed from behind. While the human spine naturally has gentle curves when viewed from the side, any sideways curvature beyond a certain degree is considered abnormal. Understanding the causes of scoliosis is essential for early detection, appropriate treatment, and preventing progression especially in children and adolescents. Scoliosis can affect people of all ages, from infants to older adults. In some cases, it remains mild and causes little discomfort. In others, it may progress and lead to pain, posture changes, breathing issues, or functional limitations. This blog explains the causes of scoliosis in a clear, factual, and medically accurate way, without myths or assumptions. What Is Scoliosis? Scoliosis is defined as a lateral (sideways) curvature of the spine measuring more than 10 degrees, confirmed through X-ray imaging. The curvature may involve: The thoracic spine (upper and mid-back) The lumbar spine (lower back) Both regions together Scoliosis is not just a cosmetic issue. In progressive cases, spinal rotation, muscle imbalance, and altered biomechanics can affect posture, mobility, and quality of life. Primary Causes of Scoliosis The causes of scoliosis vary based on age, spinal development, muscle control, and underlying medical conditions. Below are the most recognized causes, explained in detail. 1. Idiopathic Scoliosis (Most Common Cause): Key characteristics: Most commonly appears during adolescence (ages 10–18) More common in girls than boys Often detected during growth spurts May progress rapidly during puberty Idiopathic scoliosis is most commonly diagnosed during growth spurts, particularly in cases of scoliosis in children. What causes idiopathic scoliosis? Despite extensive research, the exact cause remains unknown. However, studies suggest possible links to: Genetic predisposition Abnormal spinal growth patterns Hormonal factors Neuromuscular control differences It is important to understand that idiopathic scoliosis is NOT caused by poor posture, carrying heavy school bags, sleeping positions, or lack of exercise. 2. Congenital Scoliosis (Present at Birth): Congenital scoliosis develops due to abnormal formation of the spine during early pregnancy, usually within the first 6–8 weeks of fatal development. How congenital scoliosis occurs: Some vertebrae may not form completely (hemivertebra) Vertebrae may be fused together Uneven growth leads to spinal curvature Key points: Present at birth, though may be detected later Often associated with kidney or heart abnormalities Curve may worsen as the child grows Because congenital scoliosis results from structural defects, it often requires close monitoring and, in some cases, surgical management. 3. Neuromuscular Scoliosis: Neuromuscular scoliosis occurs due to poor muscle control or muscle weakness, which prevents the spine from being properly supported. Common conditions associated with neuromuscular scoliosis: Cerebral palsy Muscular dystrophy Spinal cord injury Polio Spina bifida Why it develops: Weak or imbalanced muscles pull the spine unevenly Poor trunk control causes progressive curvature Curves often worsen over time Neuromuscular scoliosis is typically more severe and progressive than idiopathic scoliosis and often affects sitting balance and mobility. 4. Degenerative Scoliosis (Adult-Onset Scoliosis): Degenerative scoliosis develops in adults, usually after the age of 40–50, due to age-related changes in the spine. Major contributing factors: Disc degeneration Facet joint arthritis Ligament laxity Osteoporosis Spinal instability As discs lose height and joints wear out unevenly, the spine may gradually curve sideways. This form of scoliosis is often associated with chronic back pain, stiffness, and nerve compression. 5. Scoliosis Due to Leg Length Discrepancy: When one leg is shorter than the other, the pelvis tilts to compensate. Over time, this can lead to a functional scoliosis. Important points: The spine curves to maintain balance Curve may disappear when sitting or lying down Often improves with shoe lifts or leg-length correction This type is not a true structural scoliosis and is usually reversible once the underlying cause is corrected. 6. Scoliosis Caused by Spinal Tumors or Infections: Although rare, scoliosis can develop due to serious underlying spinal conditions. Possible causes include: Spinal tumors Vertebral infections (osteomyelitis, discitis) Inflammatory spinal diseases These conditions may weaken spinal bones or alter alignment, causing abnormal curvature. Sudden onset scoliosis accompanied by pain, fever, or neurological symptoms should always be evaluated urgently. 7. Postural and Muscle Imbalance Factors: Long-standing muscle imbalance or poor neuromuscular control may contribute to spinal asymmetry, particularly when combined with growth spurts or other risk factors. Important clarification: Poor posture alone does NOT cause structural scoliosis However, it may worsen existing curves or cause postural scoliosis Postural scoliosis typically improves with posture correction and physiotherapy. When Should Scoliosis Be Evaluated Medical evaluation is recommended if: One shoulder appears higher than the other Uneven hips or waistline is noticed One shoulder blade protrudes Clothes fit unevenly Back pain or stiffness develops Early evaluation by spine specialists is important to identify the cause of scoliosis and monitor the risk of progression. If signs of spinal curvature are noticed early, it is advisable to connect with our team for proper medical evaluation. Why Identifying the Cause of Scoliosis Matters Knowing the underlying cause helps determine: Risk of progression Appropriate treatment approach Need for observation, bracing, or surgery Long-term prognosis Understanding the underlying cause helps doctors plan the most appropriate scoliosis treatment for long-term spinal health. Causes of Scoliosis by Age Group In Children and Adolescents: Idiopathic scoliosis (most common) Congenital scoliosis Neuromuscular causes In Adults: Degenerative scoliosis Progression of untreated childhood scoliosis Osteoporosis-related spinal changes Understanding age-related causes helps guide diagnosis and treatment planning. Common Myths About the Causes of Scoliosis 1. Heavy school bags cause scoliosis False – They may cause back pain but do not cause structural scoliosis. 2. Bad posture causes scoliosis False – Poor posture does not cause true scoliosis. 3. Exercise can cause scoliosis False – Exercise does not cause scoliosis and is often beneficial. Understanding these myths helps reduce unnecessary fear and misinformation. Final Thoughts The causes of scoliosis are varied and complex, ranging from unknown developmental factors to congenital abnormalities, neuromuscular conditions, and age-related degeneration. While many casese specially idiopathic scoliosis have no clearly identifiable cause, early recognition and proper evaluation play a critical role in managing the condition effectively. Scoliosis
Latest Advances in Non-Surgical Spine Care You Should Know
Latest Advances in Non-Surgical Spine Care You Should Know Spine problems are no longer limited to the elderly. With modern lifestyles that involve long hours of sitting, minimal physical activity, and digital device overuse, spinal conditions like slip discs, sciatica, cervical spondylosis, and chronic back pain are increasingly common in young and middle-aged adults. Traditionally, severe back or neck issues often led people to believe surgery was the only solution. However, medical science has made significant progress in non-surgical spine care, offering safer, effective, and long-lasting treatments that avoid the risks associated with surgery. If you are searching for the best spine care solutions, you’ll be glad to know that today’s non-invasive and minimally invasive treatments combine advanced technology, physiotherapy, regenerative medicine, and lifestyle modifications. This article explores the latest advances in non-surgical spine treatment that are reshaping how patients recover from spinal problems. Why Non-Surgical Spine Care Matters Before diving into the latest innovations, it is important to understand why non-surgical approaches are gaining more attention worldwide: Lower risk compared to surgery: No anesthesia, surgical scars, or hospital stays. Faster recovery time: Patients often resume daily activities sooner. Cost-effective: Non-surgical treatments are generally more affordable than surgery. Focus on long-term health: Treatments aim at rehabilitation, posture correction, and lifestyle changes. Spine specialists and physiotherapists now prefer these approaches whenever possible, recommending surgery only when absolutely necessary. Regenerative Medicine in Spine Care One of the most exciting areas in advanced spine treatment is regenerative medicine, which uses the body’s natural healing mechanisms to repair damaged tissues. Stem Cell Therapy Uses stem cells harvested from the patient’s own bone marrow or fat tissue. Helps regenerate damaged spinal discs or cartilage. Reduces inflammation and promotes natural healing. Platelet-Rich Plasma (PRP) Therapy Involves drawing the patient’s blood, processing it to concentrate platelets, and injecting it into the affected spine area. Platelets release growth factors that accelerate tissue repair. Benefits: Minimally invasive Can reduce chronic pain May delay or even prevent the need for surgery Image-Guided Injections for Precision Treatment Traditional pain injections were often given without precise targeting, but now advanced imaging like fluoroscopy and ultrasound has revolutionized their accuracy. Epidural Steroid Injections (ESIs) Used to reduce inflammation around irritated nerves (commonly in sciatica or herniated discs). Provides significant short- to medium-term pain relief. Facet Joint Injections Target the small joints between vertebrae that often cause localized pain. Nerve Blocks Temporarily interrupt pain signals sent from the nerves to the brain. With imaging technology, doctors can now deliver medications with pinpoint accuracy, minimizing side effects and maximizing results. Minimally Invasive Pain Procedures Non-surgical does not mean “no procedure.” Some minimally invasive techniques are highly effective for chronic back pain patients who don’t respond to conservative care. Radiofrequency Ablation (RFA) Uses heat generated by radio waves to “switch off” specific pain-carrying nerves. Relief can last for months or even years. Cryoablation Freezes the targeted nerve to stop pain signals. These techniques have transformed spine care by giving patients longer-lasting relief without the risks of major surgery. Advances in Physiotherapy and Rehabilitation Physiotherapy has always been the foundation of non-surgical spine treatment. Today, it has evolved with technology and science-backed approaches. Robotic-Assisted Rehabilitation Robotic devices guide patients through precise movements, improving muscle control and posture. AI-Guided Exercise Programs Apps and platforms analyze patient progress and adjust exercise difficulty in real time. Manual Therapy + Technology Traditional hands-on techniques are now combined with ultrasound therapy, laser therapy, and electrical stimulation to enhance recovery. Spinal Decompression Therapy This is a non-surgical, traction-based treatment that relieves pressure on spinal discs and nerves. Involves a motorized table that gently stretches the spine. Creates negative pressure inside the discs, encouraging retraction of herniated material. Promotes nutrient-rich fluid flow for healing. Studies show that patients with slip discs or chronic lower back pain often benefit from this therapy when combined with physiotherapy and lifestyle changes. Wearable Technology for Spine Care Wearables are no longer just for fitness tracking; they now play a role in spinal health. Posture-correcting wearables: Alert users when they slouch. Smart braces: Provide support while allowing mobility. Mobile health apps: Track pain levels, daily activity, and recovery progress. This trend empowers patients to take charge of their spine care on a daily basis. The Role of Lifestyle Medicine in Spine Health One of the biggest advances in spine care is not a device or drug—it’s a holistic approach. Modern spine specialists now emphasize lifestyle medicine as an essential part of treatment. Exercise and Movement Regular stretching and strengthening exercises prevent stiffness and maintain spinal flexibility. Core-strengthening workouts support the spine and reduce the risk of disc-related problems. Ergonomics Adjustable chairs, sit-stand desks, and ergonomic keyboards can prevent posture-related strain. Work-from-home setups are now being tailored with spine health in mind. Sleep and Recovery Orthopedic mattresses and proper sleeping positions reduce spinal stress. Sleep tracking technology helps identify poor sleep patterns that may worsen pain. By treating the root causes (sedentary lifestyle, poor posture, excess weight), lifestyle medicine reduces dependency on drugs or surgery. Yoga and Mind-Body Therapies Non-surgical spine care increasingly recognizes the connection between mental health and back pain. Stress, anxiety, and poor lifestyle habits can worsen spinal problems. Yoga Therapy Poses like Cat-Cow, Child’s Pose, and Cobra improve flexibility and reduce stiffness. Focuses on deep breathing, posture awareness, and body balance. Mindfulness and Meditation Helps manage chronic pain perception. Reduces stress hormones that contribute to muscle tension. Hospitals and spine care centers are now offering integrated yoga-based rehabilitation programs, combining traditional wisdom with medical guidance. Nutritional Support for Spinal Healing Nutrition is often overlooked in spine care, but it plays a key role in recovery. Key Nutrients for Spine Health Calcium & Vitamin D: Essential for strong bones. Magnesium: Reduces muscle spasms. Omega-3 fatty acids: Natural anti-inflammatory properties. Collagen & protein: Support disc and cartilage health. Specialized diet plans now form part of advanced non-surgical treatment to support healing and prevent recurrence of spine problems. Telemedicine and Digital Spine Care The COVID-19 pandemic accelerated the adoption of virtual spine consultations. Today, telemedicine is a