Is Non-Surgical Spine Treatment Effective for Slip-Disc and Sciatica?
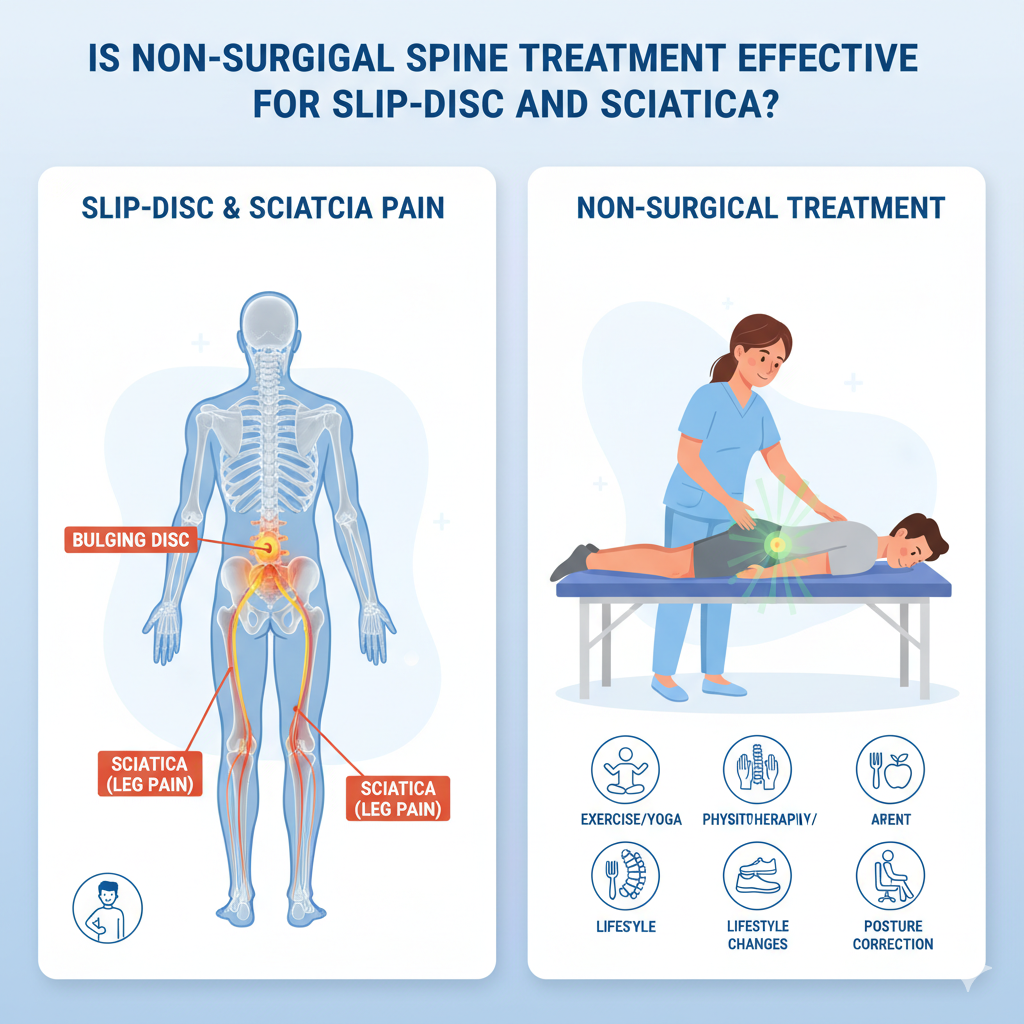
Is Non-Surgical Spine Treatment Effective for Slip-Disc and Sciatica? Modern lifestyles have made back pain one of the most common health complaints worldwide. Whether it’s long hours at a desk, heavy lifting at work, or poor posture, spinal problems are increasingly affecting young and middle-aged adults alike. Among the most widespread conditions are slip-disc (herniated disc) and sciatica, both of which can cause chronic discomfort and limit mobility. Traditionally, many people assume that surgery is the only way to fix severe spinal issues. But in reality, research shows that non-surgical spine treatment can often be just as effective — especially in the early and moderate stages. In fact, according to the World Health Organization (WHO) and National Institutes of Health (NIH), conservative treatment options are usually the first line of management before surgery is even considered. This article explores whether non-surgical spine treatment is effective for slip-disc and sciatica, breaking down the science, treatment methods, and practical strategies patients can rely on.th. Understanding Slip-Disc and Sciatica What Is a Slip-Disc? The human spine is made of 33 vertebrae cushioned by intervertebral discs that act as shock absorbers. A slip-disc, also called a herniated or prolapsed disc, happens when the soft, gel-like core of a disc pushes through a crack in its tougher outer layer. This bulging disc can press on nearby nerves, leading to pain, tingling, or weakness. The severity of symptoms depends on the disc’s location and the degree of nerve compression. Cervical slip-disc: affects the neck, causing radiating pain into the arms or shoulders. Lumbar slip-disc: affects the lower back, commonly linked to sciatica. What Is Sciatica? Sciatica is not a condition itself but a symptom of nerve irritation. It occurs when the herniated disc presses on the sciatic nerve — the longest nerve in the body that runs from the lower back to the legs. Typical signs of sciatica include: Shooting pain down one leg Numbness or tingling in the thigh, calf, or foot Muscle weakness in the lower limb Worsening discomfort after prolonged sitting According to Harvard Health Publishing, more than 80% of people experience back pain at some point, and sciatica affects nearly 40% of adults during their lifetime. Why Surgery Isn’t Always the First Solution Surgical options like discectomy or laminectomy are sometimes necessary, especially if symptoms are severe, progressive, or accompanied by bowel/bladder dysfunction. However, studies published in The Spine Journal and PubMed suggest that most people with herniated discs improve significantly with non-surgical spine treatments. Key Reasons Non-Surgical Approaches Are Preferred First: Lower risk of complications compared to surgery Shorter recovery time Cost-effectiveness Effectiveness for mild to moderate cases Surgery reserved only for severe or persistent cases Non-Surgical Spine Treatments: An Overview When it comes to non-surgical spine treatment, a variety of evidence-based methods are available. These focus on pain relief, mobility restoration, and preventing further disc damage.Here’s a breakdown of the most effective techniques: 1. Physiotherapy and Rehabilitation Core strengthening and flexibility exercises Stretching routines to reduce nerve pressure Manual therapy and mobilization Posture correction programs A 2017 study in the Journal of Orthopaedic & Sports Physical Therapy (JOSPT) confirmed that exercise-based rehabilitation improves pain and functionality in herniated disc patients without surgery. 2. Medications NSAIDs (Non-Steroidal Anti-Inflammatory Drugs): For pain and inflammation control Muscle relaxants: To ease muscle spasms Neuropathic pain medications: For nerve-related discomfort Doctors usually prescribe medications for short-term relief while encouraging long-term lifestyle adjustments. 3. Epidural Steroid Injections Targeted injections reduce inflammation around the irritated nerve. Provide temporary relief (weeks to months). Often combined with physiotherapy for better results. According to Mayo Clinic, epidural injections can be particularly useful for severe sciatica cases when oral medications alone aren’t effective. 4. Lifestyle and Ergonomics Adjusting sitting posture Using ergonomic chairs and standing desks Weight management Regular breaks during long hours of sitting WHO recommends at least 150 minutes of moderate physical activity per week, which significantly lowers risks of chronic back problems. 5. Alternative Therapies (Evidence-Supported) Yoga: Improves flexibility and core strength Acupuncture: Recognized by NIH as effective for chronic back pain in some patients Heat therapy: Relieves muscle tension and stiffness How Effective Are Non-Surgical Spine Treatments? The central question many patients ask is: “Do non-surgical methods really work for slip-disc and sciatica?” The answer is yes, in most cases. Numerous clinical studies have shown that non-surgical treatments can relieve symptoms, improve mobility, and prevent progression. A study published in the British Medical Journal (BMJ, 2016) found that 90% of patients with lumbar disc herniation improved with conservative care within three months. The National Institute of Neurological Disorders and Stroke (NINDS, USA) reports that most sciatica cases resolve without surgery if patients follow prescribed physiotherapy and lifestyle modifications. In India, guidelines from the Ministry of Health & Family Welfare recommend physiotherapy, exercise, and ergonomic correction as first-line management for herniated discs. These findings reinforce that surgery is not always the default solution. Instead, non-surgical spine treatments can be highly effective, especially when patients are consistent and proactive about their care. Benefits of Non-Surgical Spine Treatments Non-surgical care isn’t just about avoiding the risks of surgery. It offers multiple benefits: 1. Lower Risk Profile No anesthesia or surgical complications Reduced chance of infection or nerve damage. 2. Cost-Effectiveness Surgery can be significantly more expensive compared to physiotherapy and medication. 3. Faster Return to Normal Activity Most patients can resume daily routines with guided rehabilitation. 4. Preventing Recurrence Lifestyle and ergonomic corrections address root causes, lowering the risk of future slip-disc episodes. When Is Surgery Necessary? While non-surgical spine treatments work for the majority, there are cases where surgery becomes unavoidable. Surgery may be considered if: Severe, disabling pain persists beyond 6–12 weeks of non-surgical care. Progressive neurological deficits (e.g., worsening leg weakness) are noted. Bowel or bladder dysfunction occurs (a red-flag emergency). Even then, modern minimally invasive surgeries like microdiscectomy have high success rates. But the key message remains: most people do not require surgery if they respond to non-surgical treatment. Practical Tips to Support Recovery Without Surgery Non-surgical treatment is most effective when combined with healthy daily habits. Here are actionable tips: Ergonomic Adjustments Use a chair with lumbar support. Keep computer screens at eye level. Take breaks every 30–40 minutes to stretch. Stretching & Microbreaks Gentle hamstring and back stretches can ease nerve pressure. Short “microbreaks” of 2–3 minutes throughout the day
Neck Strain vs Cervical Disc Problem: How to Tell the Difference
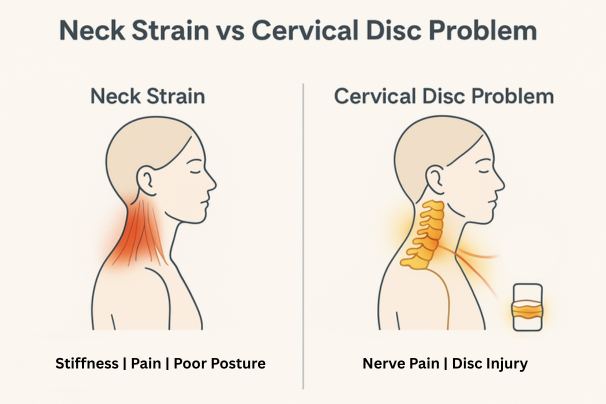
Neck Strain vs Cervical Disc Problem: How to Tell the Difference Neck pain is one of the most common health complaints in modern life. For some, it’s a dull stiffness after a long day at the desk. For others, it’s a sharp pain that radiates down the arm, making even simple tasks unbearable. Two conditions that often get confused are neck strain (a soft tissue injury) and cervical disc problems (a spine-related condition such as herniation or degeneration). At first glance, both cause discomfort in the neck region, but they are not the same. Misunderstanding the difference can delay proper treatment and sometimes worsen the problem. This blog will take you through: What neck strain is and how it happens What cervical disc problems are and their causes The key differences between the two conditions Symptoms you should watch out for When to seek medical help Treatment options (home-based and clinical) Preventive strategies to protect your neck A patient-friendly FAQ section And a practical table summarizing differences at a glance By the end, you’ll have a clear, evidence-based understanding of neck strain vs cervical disc problem, helping you make informed decisions about your health. Understanding the Basics What is Neck Strain? A neck strain is an injury to the muscles or tendons in the cervical (neck) region. It usually occurs when the neck muscles are overstretched or torn due to: Poor posture (slouching at a desk, hunching over a phone) Sleeping in an awkward position Sudden movements or whiplash injuries Carrying heavy bags on one shoulder Sports injuries or overuse Key point: Neck strain is typically soft tissue–related and often temporary. What is a Cervical Disc Problem? The cervical spine consists of seven vertebrae (C1–C7) separated by intervertebral discs that act as cushions. These discs can undergo changes due to wear and tear, trauma, or disease. Common cervical disc issues include: Herniated disc (slipped disc): When the soft nucleus of the disc pushes out through its outer layer, pressing on nearby nerves. Degenerative disc disease: Natural age-related breakdown of discs, leading to stiffness and chronic pain. Disc bulge: Less severe than herniation but can still cause nerve compression. Key point: Cervical disc problems are structural issues of the spine and may require medical intervention. Causes: Why They Happen Neck Strain Causes Poor ergonomics (long hours at computer) Overexertion during exercise Carrying uneven weight (e.g., heavy backpacks) Sudden jerks or accidents Stress-induced muscle tightness Cervical Disc Problem Causes Natural aging (disc dehydration, loss of elasticity) Repetitive strain injuries (desk jobs, driving long hours) Sudden trauma (accidents, falls) Genetic predisposition Smoking (which accelerates disc degeneration) Common Symptoms of Neck Strain Localized neck pain or stiffness Pain that worsens with movement Muscle spasms or tightness Limited range of motion Headaches at the base of the skull Important: Neck strain usually improves within days to weeks with rest and conservative care. Common Symptoms of Cervical Disc Problems Neck pain radiating to the shoulders, arms, or hands Numbness, tingling, or weakness in the arms Shooting or burning pain (nerve involvement) Reduced neck flexibility In severe cases: difficulty with coordination, grip strength, or walking (if spinal cord compression occurs) Important: Cervical disc problems often persist or worsen without treatment and may require medical evaluation. Key Differences Between Neck Strain and Cervical Disc Problems Feature Neck Strain Cervical Disc Problem Cause Muscle/tendon overstretching Structural disc damage (herniation, degeneration) Onset Sudden after overuse or awkward posture Gradual due to aging or sudden trauma Pain Location Localized to neck, sometimes mild headache Neck + radiating pain to shoulders/arms Associated Symptoms Stiffness, spasms Tingling, numbness, weakness Duration Usually resolves in 1–3 weeks Often chronic or recurrent Treatment Rest, physiotherapy, posture correction May require medication, injections, or surgery Urgency Usually mild, self-limiting Can be serious, needs medical attention if nerve compression Diagnostic Approaches For Neck Strain Physical examination: Checking tenderness, range of motion, and muscle strength Imaging (rarely needed): X-rays/MRIs usually not required unless symptoms persist For Cervical Disc Problems MRI: Gold standard for visualizing discs and nerve compression X-ray: Shows spinal alignment and degeneration CT scan or Myelogram: In special cases Neurological exam: Reflexes, muscle strength, sensation Treatment Options Treating Neck Strain Rest (but not complete immobilization) Cold/heat therapy – ice packs first 48 hours, then heat to relax muscles Over-the-counter medication (NSAIDs like ibuprofen) Physiotherapy exercises – gentle stretches, strengthening Posture correction – ergonomic workstations, supportive pillows Treating Cervical Disc Problems Conservative care: Physical therapy to strengthen neck muscles Anti-inflammatory medications Epidural steroid injections for nerve pain Advanced interventions: Surgery in severe cases (discectomy, fusion, or artificial disc replacement) Minimally invasive spine surgery options available in India Lifestyle management: Quit smoking Maintain healthy body weight Regular low-impact exercise (walking, swimming, yoga) Prevention: Protecting Your Neck Ergonomics: Adjust screen height, keep spine neutral Frequent breaks: Stretch every 30–45 minutes while working Correct lifting techniques: Use both hands, avoid sudden jerks Strengthening exercises: Focus on neck, shoulders, and core Sleep support: Use a cervical pillow; avoid sleeping on stomach Hydration and nutrition: Keep discs healthy with good hydration and calcium-rich diet When to See a Doctor Immediately Severe neck pain that doesn’t improve in 1–2 weeks Pain radiating to arms or legs Weakness, numbness, or tingling in hands/fingers Loss of balance or bladder/bowel issues (signs of spinal cord compression) FAQs Can neck strain turn into a disc problem?Not directly. But repeated strain and poor posture can contribute to disc degeneration over time. Do I always need an MRI for neck pain?No. Most neck strains heal without imaging. MRIs are usually recommended if symptoms persist or there are nerve-related signs. Is surgery always required for cervical disc problems?No. Over 80% of patients improve with conservative treatments. Surgery is reserved for severe or progressive cases. How long does recovery take?-Neck strain: 1–3 weeks with proper care.-Cervical disc issues: Several weeks to months, depending on severity. Role of Physiotherapy Physiotherapy plays a critical role in both conditions: For neck strain: restoring flexibility, reducing stiffness For cervical disc issues: strengthening muscles, improving posture, preventing recurrence Techniques include manual therapy, traction, ultrasound therapy, and guided exercises. Trusted Spine Care at We Are Spine If you are struggling to figure out whether your neck pain is a simple muscle strain or a
Is Neck Pain Linked to Migraines? Causes and What Science Says

Is Neck Pain Linked to Migraines? Causes and What Science Says Almost everyone has experienced neck stiffness after a long day of working at a desk or scrolling on a phone. But for millions of people, that neck pain isn’t just discomfort — it’s a possible trigger for migraines, one of the world’s most disabling neurological conditions. Migraines affect over 1 billion people globally, making them the second leading cause of disability worldwide, according to the World Health Organization (WHO). In India, studies by the Indian Council of Medical Research (ICMR) estimate that nearly 150 million people suffer from migraines, with women three times more likely to be affected than men. At the same time, neck pain ranks among the top musculoskeletal problems, with research suggesting that 20–30% of adults experience neck pain at any given time. Prolonged sitting, poor posture, stress, and screen-heavy lifestyles make this an everyday issue for students, working professionals, and older adults alike. But here’s the pressing question: is neck pain really linked to migraines, or do they just happen to occur together? Scientific research over the past two decades suggests a strong connection between the two. Neck pain may act as a trigger, a symptom, or even a warning sign for migraine attacks. Understanding this relationship can help patients seek the right treatment earlier, reduce suffering, and improve quality of life. This article explores the science behind the connection between neck pain and migraines, the causes, real-world statistics, diagnostic challenges, and evidence-based treatments — all in a way that’s clear, relatable, and actionable. Understanding Migraines What Are Migraines? Migraines are neurological disorders, not just “bad headaches.” They involve abnormal brain activity that affects nerves, blood vessels, and chemicals in the brain. Key features include: Throbbing or pulsating head pain, usually on one side Pain lasting 4 to 72 hours if untreated Accompanied by nausea, vomiting, light and sound sensitivity Sometimes preceded by an aura (visual changes, tingling, or speech disturbances) The Global Burden of Disease Study (2019) ranked migraines among the top 10 most disabling medical conditions, often interfering with work, family, and social life. Types of Migraines Migraine with aura – visual or sensory disturbances before the headache Migraine without aura – the most common type Chronic migraine – headaches on 15 or more days a month for over 3 months Understanding Neck Pain Why Is Neck Pain So Common? The cervical spine is a delicate yet powerful structure. It consists of 7 vertebrae (C1–C7), intervertebral discs, muscles, ligaments, and nerves that support the head and allow movement. However, this region is vulnerable to strain and injury. Common causes of neck pain include: Prolonged sitting and forward head posture Muscle tension from stress Degenerative changes (cervical spondylosis, disc herniation) Injuries or whiplash Poor ergonomics at work or while using digital devices Research in the Indian Journal of Orthopaedics (2017) reported that up to 34% of Indian IT professionals complain of chronic neck pain, highlighting the scale of the problem in a digital economy. The Science of the Neck-Migraine Connection The connection between neck pain and migraines is both neurological and musculoskeletal. 1. Shared Nerve Pathways The trigeminocervical complex (TCC) is a hub of nerve fibers that receive signals from both the trigeminal nerve (responsible for facial sensation and migraines) and the upper cervical spinal nerves (C1–C3). When the neck is strained or irritated, these signals can “cross-talk” and the brain may interpret the pain as coming from the head — triggering or worsening a migraine. 2. Muscle Tension and Blood Flow Tight neck muscles, such as the trapezius and suboccipital muscles, can restrict blood flow and irritate nerves, leading to headache or migraine-like pain. 3. Posture as a Trigger Poor posture, especially forward head posture, increases stress on cervical structures. This chronic strain sensitizes the TCC, making individuals more vulnerable to migraines. 4. Overlapping Symptoms Both migraines and neck pain can cause stiffness, fatigue, and restricted movement. Up to 75% of migraine patients report neck pain during or before attacks (Cephalalgia, 2018). What Research Says Mayo Clinic reports that people with chronic neck dysfunction have a higher frequency of migraines. A PubMed study (2018) found that treating cervical muscle tension reduced migraine intensity in many patients. Harvard Health emphasizes posture correction and physiotherapy as effective preventive strategies. AIIMS Delhi (2020): Patients undergoing cervical spine strengthening exercises reported significant reductions in migraine frequency and severity. Signs That Neck Pain Is Linked to Migraines Warning Signs to Watch For Headache worsens with neck movement Pain begins in the neck and radiates to the head Stiffness is present during migraine attacks Relief when neck muscles are stretched or massaged Migraine triggers include prolonged sitting or posture strain Diagnosis – How Do Doctors Differentiate? Key Steps in Diagnosis Medical history and symptom diary Physical exam – posture, cervical spine range of motion, muscle tenderness Neurological tests – checking reflexes, coordination, sensory function Imaging (MRI or CT) if disc herniation, nerve compression, or other pathology is suspected Differentiating between cervicogenic headache and migraine is crucial since treatment differs. Treatment Options 1. Medical Approaches Triptans for acute migraine relief Preventive medications like beta-blockers or anti-seizure drugs Muscle relaxants if cervical spasm is contributing Botox injections in chronic migraine cases 2. Physiotherapy and Exercise Chin tucks to correct posture Neck stretches for trapezius and levator scapulae Strengthening deep cervical flexors Manual therapy for muscle release 3. Ergonomic Adjustments Keep screen at eye level Use a chair with cervical support Take micro-breaks every 30 minutes 4. Lifestyle Changes Consistent sleep schedule Stay hydrated Stress management with yoga or meditation Prevention Strategies Posture checks every hour Stretching routine for neck and shoulders Ergonomic setup at work and study stations Balanced diet and hydration Early medical consultation when symptoms persist When to Seek Medical Help Seek urgent care if: Migraines occur more than 15 days/month Pain is accompanied by vision problems or weakness Neck pain worsens with tingling or numbness in arms OTC painkillers stop working The Role of We Are Spine At We Are Spine, specialists understand the complex overlap between neurological conditions like migraines and musculoskeletal issues like cervical pain. The team combines neurology, physiotherapy, and spine care expertise to create individualized treatment plans. Whether it’s posture training, non-surgical management, or guided rehabilitation, WeAreSpine helps patients reduce pain and reclaim quality of life. Conclusion Neck pain and migraines are not isolated problems — they are closely linked through shared nerve pathways, posture issues, and
10 Best Exercises for Neck Pain Relief That Actually Work
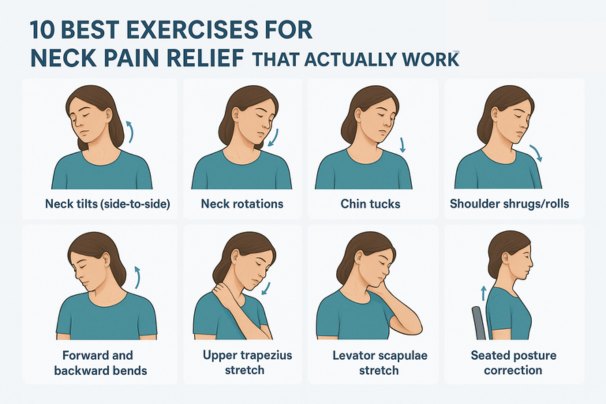
10 Best Exercises for Neck Pain Relief That Actually Work If you’re reading this while rubbing your neck or shifting in your chair, you’re not alone. Neck pain has become one of the most common musculoskeletal complaints worldwide. The World Health Organization (WHO) recognizes neck pain as a major contributor to disability, and research published in The Lancet ranks it among the leading causes of years lived with disability (YLDs) globally. In India, neck pain is especially prevalent among office professionals, IT employees, call-center workers, students, and homemakers who spend long hours in front of screens or doing repetitive tasks. According to an ICMR (Indian Council of Medical Research) report, nearly 30–35% of working professionals in urban India report chronic or recurring neck pain, often linked to poor posture and prolonged sitting. The good news is that regular exercise and stretching can significantly reduce neck pain, improve flexibility, and restore spinal health. Unlike painkillers, which only mask symptoms, exercise addresses the root cause — muscle weakness, poor posture, and joint stiffness. In this article, we’ll explore 10 best exercises for neck pain relief that are: Backed by science Easy to perform at home or in the office Safe for most people when done correctly We’ll also look at posture tips, lifestyle habits, and when to seek medical help. Why Exercise Helps with Neck Pain Before we dive into the exercises, let’s understand why movement is medicine for neck pain. Improves blood circulation → Supplies oxygen and nutrients to tight muscles and stiff joints. Releases muscle tension → Reduces stiffness caused by prolonged screen time. Strengthens stabilizer muscles → Supports cervical vertebrae and prevents future strain. Enhances posture → Counteracts forward head posture (common with phone/laptop use). Reduces nerve compression → By keeping discs and joints flexible. A study published in the Journal of Orthopaedic & Sports Physical Therapy (JOSPT) found that targeted neck exercises combined with postural correction significantly reduced chronic neck pain within 6 weeks. The 10 Best Exercises for Neck Pain Relief Below are 10 proven, easy-to-do exercises. Each is explained with step-by-step instructions, benefits, and safety notes. 1. Neck Side-to-Side Stretch (Lateral Flexion) How to do it: Sit or stand upright with shoulders relaxed. Slowly tilt your head to the right, bringing your ear closer to your shoulder. Hold for 20–30 seconds, feeling the stretch along the opposite side of the neck. Return to center and repeat on the other side. Perform 3–5 repetitions per side. Benefits: Stretches the upper trapezius and scalene muscles, which are commonly tight in desk workers. Relieves stiffness from prolonged sitting. Scientific note:A workplace trial in Sweden (2016) showed that simple side flexion stretches performed thrice daily reduced reported neck discomfort among office staff by 35%. 2. Neck Rotation (Side-to-Side Turns) How to do it: Sit tall with chin level. Slowly turn your head to the right as if looking over your shoulder. Hold 20 seconds. Return to center and repeat left side. Do 5–6 repetitions each side. Benefits: Improves cervical spine mobility. Helpful for drivers, bikers, or anyone with difficulty turning the head. Tip: Move slowly; avoid jerky motions. 3. Chin Tucks (Cervical Retractions) How to do it: Sit upright with your back supported. Gently pull your chin straight back, creating a “double chin” effect. Hold 5 seconds, then relax. Repeat 10–12 times. Benefits: Strengthens deep neck flexor muscles. Corrects forward head posture caused by mobile/laptop use. Reduces disc pressure on cervical spine. Evidence:Endorsed by the American Physical Therapy Association (APTA) as one of the most effective posture-correcting exercises. 4. Shoulder Rolls How to do it: Sit or stand tall. Lift shoulders upward, roll them backward, then drop down. Perform 10–15 rolls. Repeat rolling forward as well. Benefits: Relieves tension in the upper trapezius and rhomboids. Improves shoulder-neck coordination. Pro tip: Pair with deep breathing for added stress relief. 5. Levator Scapulae Stretch How to do it: Sit tall. Place right hand behind your head. Tilt head down and to the left, like looking into your armpit. Hold 20–30 seconds. Repeat on other side. Benefits: Stretches the levator scapulae muscle, often strained by phone cradling or hunching. Evidence:A physiotherapy study in Manual Therapy Journal found levator scapulae stretching reduced pain intensity in office workers by up to 40% in 4 weeks. 6. Upper Trapezius Stretch How to do it: Sit on a chair, holding the edge with your right hand. Tilt head to the left, bringing ear toward shoulder. Gently apply pressure with left hand on the head. Hold 20–30 seconds. Repeat other side. Benefits: Releases tightness in trapezius, a common stress-related muscle. Reduces tension headaches linked to neck strain. 7. Cat-Cow Stretch (Yoga for Spine & Neck) How to do it: Get on all fours, hands under shoulders, knees under hips. Inhale → arch your back, lift head & chest (cow pose). Exhale → round spine, tuck chin to chest (cat pose). Repeat 8–10 times. Benefits: Mobilizes entire spine, including cervical region. Relieves stiffness in neck and shoulders. Evidence:Yoga-based stretches like Cat-Cow are proven in multiple RCTs to reduce musculoskeletal pain. 8. Wall Angels How to do it: Stand with back flat against wall, arms at 90°. Slowly raise arms overhead while keeping elbows/wrists against wall. Lower back down. Repeat 10–12 times. Benefits: Strengthens postural muscles (rhomboids, rear deltoids). Corrects rounded shoulders and forward neck posture. 9. Isometric Neck Strengthening How to do it: Place palm on forehead, gently push head into palm (without moving). Hold 5 seconds. Repeat with palm on back of head, then sides. Do 5–8 repetitions per direction. Benefits: Strengthens stabilizing muscles. Safe for those with limited mobility, as no actual neck movement occurs. 10. Thoracic Extension Stretch How to do it: Sit on a chair with firm backrest up to mid-back. Place hands behind head, arch backward gently. Hold 10–15 seconds. Repeat 5–8 times. Benefits: Restores thoracic mobility. Reduces compensatory strain on cervical spine. Putting It Together: A Sample Neck Relief Routine Here’s a 10-minute daily routine combining the above: Side-to-side stretch – 30 sec each side Chin tucks – 10 reps Neck rotation – 5 reps each side Shoulder rolls – 15 reps Levator scapulae stretch – 20 sec each side Cat-Cow stretch – 8 reps Wall angels – 10 reps Isometric strengthening – 5 reps per direction Upper trapezius stretch – 20 sec each side Thoracic extension – 5 reps Done in 10–12 minutes, this routine can be performed at your
Early Signs of Cervical Spondylosis You Should Never Ignore
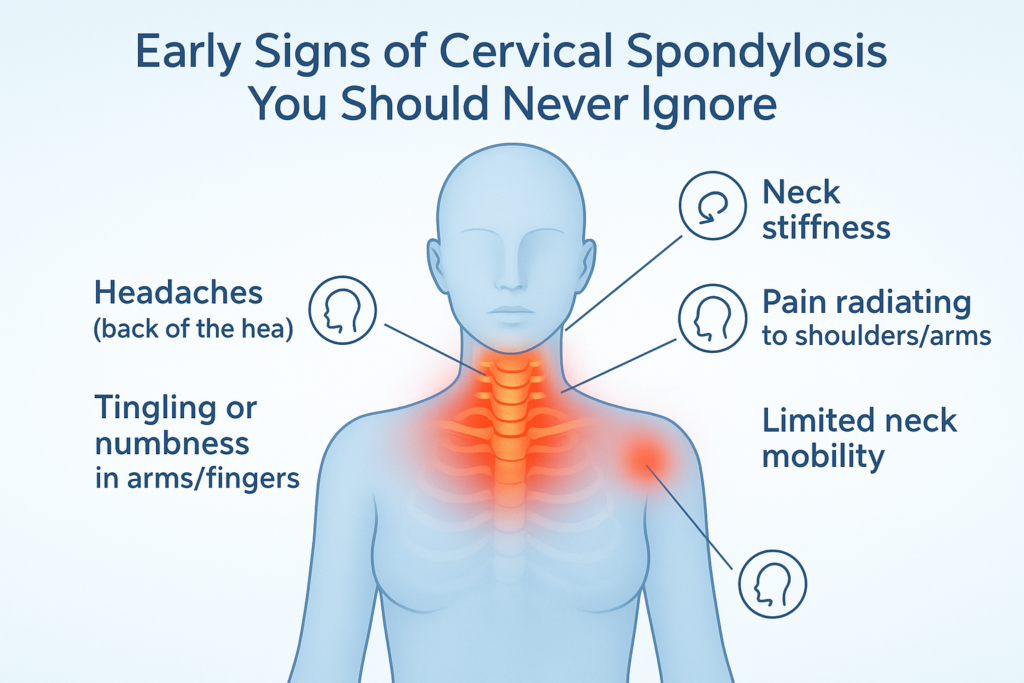
Early Signs of Cervical Spondylosis You Should Never Ignore Neck pain has silently become one of the most common health complaints of the modern era. With the surge in desk jobs, smartphone usage, and screen-based lifestyles, more people are reporting stiffness, aches, and recurring discomfort in the neck. What often begins as a minor inconvenience is sometimes a sign of a more serious spinal condition known as cervical spondylosis. Cervical spondylosis refers to the wear and tear of the bones, discs, and joints of the neck (cervical spine). While it is primarily age-related, lifestyle factors have accelerated its onset. According to the Mayo Clinic, more than 85% of people over 60 years show signs of cervical spondylosis on imaging. But in India, studies have revealed that young professionals in their late 20s and 30s are increasingly being diagnosed due to prolonged screen exposure, poor posture, and lack of spinal care. Why is this concerning? Because ignoring the early signs allows the condition to progress silently. Over time, it may lead to nerve compression, spinal cord involvement, and significant disability. Recognizing the early red flags and acting upon them is key to prevention and management. This blog will explore the science, symptoms, diagnosis, and treatments of cervical spondylosis, with practical lifestyle and ergonomic advice, and highlight why Indians in particular must take this condition seriously. Understanding Cervical Pain Cervical spondylosis, also called cervical osteoarthritis or neck arthritis, is a degenerative condition of the cervical spine. The cervical spine consists of: Seven vertebrae (C1–C7): The bones forming the neck portion of the spine. Intervertebral discs: Soft cushions between vertebrae acting as shock absorbers. Facet joints and ligaments: Supporting structures that allow movement and stability. Over time, these structures undergo degeneration due to aging, repetitive strain, or injury. Key changes include: Disc dehydration and shrinkage, reducing cushioning. Bone spurs (osteophytes) developing as a compensatory response. Ligament stiffening, which reduces flexibility. Joint cartilage wear, leading to stiffness and inflammation. While mild degeneration is considered a part of aging, when it progresses to symptoms such as pain, nerve compression, or restricted mobility, it is clinically diagnosed as cervical spondylosis. Why Early Recognition is Crucial Cervical spondylosis often develops slowly. At first, symptoms may appear mild or intermittent, such as neck stiffness after a long day at work. Many people dismiss these as “normal” aches. However, untreated spondylosis may worsen, leading to complications such as: Cervical radiculopathy: Pinched nerve causing pain, tingling, or weakness in arms/hands. Cervical myelopathy: Compression of the spinal cord leading to balance problems, coordination issues, or even bladder/bowel dysfunction. Chronic disability: Severe stiffness and mobility restriction. Early identification and management — often with non-surgical treatments like physiotherapy and ergonomics — can stop progression and restore quality of life. Early Signs of Cervical Spondylosis You Should Never Ignore Here are the most common warning signals backed by medical literature (NIH, Mayo Clinic, PubMed): 1. Persistent Neck Stiffness A hallmark symptom. Patients describe it as difficulty moving the head freely. Worse in mornings or after long sitting sessions. 2. Frequent Headaches (Cervicogenic Headaches) Originating from neck strain. Pain radiates from base of skull to forehead. Often misdiagnosed as migraines or tension headaches. 3. Shoulder and Arm Pain Pain radiating from the neck to shoulder/arm. Suggests nerve root irritation. Sometimes sharp, sometimes dull ache. 4. Tingling or Numbness in Hands and Fingers Indicates nerve compression. May affect grip strength and fine motor skills. 5. Grinding or Popping Sounds (Crepitus) Audible clicks or grinding with neck motion. Sign of cartilage wear and bone spur friction. 6. Reduced Neck Mobility Difficulty turning head sideways. Restricted motion during driving or looking up/down. 7. Muscle Weakness Weak grip, dropping objects. Caused by long-standing nerve impingement. 8. Dizziness and Balance Issues Less common but significant. Related to cervical myelopathy or vascular compromise. 9. Fatigue and Sleep Disturbances Chronic pain disrupts sleep cycles. Leads to daytime tiredness and reduced productivity. Risk Factors According to Harvard Health, WHO, and NIH, key risk factors include: Age: Most common over 40–50 years. Occupation: IT professionals, drivers, teachers, students with long screen hours. Posture: Slouching, forward head posture, prolonged laptop/mobile use. Smoking: Accelerates disc degeneration. Genetics: Family history of osteoarthritis. Injuries: Previous trauma to the neck. Lack of exercise: Weak supporting muscles worsen degeneration. Diagnosis If symptoms persist, medical evaluation is essential. Standard diagnostic tools include: Physical examination: Testing reflexes, muscle strength, range of motion. X-rays: Reveal bone spurs, disc height loss. MRI: Shows disc bulges, nerve or spinal cord compression. CT scans: For detailed bone structure. Electromyography (EMG): Measures nerve electrical activity. Treatment Options Non-Surgical Approaches (First Line) Physiotherapy: Stretching, strengthening, posture retraining. Medications: NSAIDs, muscle relaxants. Heat/Ice therapy: Relieves stiffness. Cervical collars (short-term): For acute pain flare-ups. Lifestyle modifications: Ergonomic seating, screen breaks. Surgical Approaches (For Severe Cases) Discectomy: Removal of herniated disc. Laminectomy: Decompression by removing bone. Spinal fusion: Stabilization of vertebrae. Surgery is rare and reserved for severe neurological impairment. Lifestyle and Self-Care for Prevention Ergonomic Practices Keep screens at eye level. Use chairs with proper lumbar and neck support. Take 5-minute breaks every 30–40 minutes. Exercises (Medically Recommended) Neck stretches: Side bends, rotations. Chin tucks: To correct forward posture. Shoulder blade squeezes: Strengthen upper back. Nutrition Calcium and Vitamin D for bone strength. Omega-3 fatty acids (flaxseeds, walnuts) for anti-inflammatory effect. Magnesium and protein for muscle and disc health. Sleep Hygiene Use orthopedic pillows. Avoid sleeping on stomach. Keep neck aligned with spine. Cervical Spondylosis in India: An Emerging Epidemic A study conducted at AIIMS, New Delhi found a significant increase in cervical spondylosis cases among IT professionals under 40 years. Prolonged sitting, poor ergonomics, and mobile phone use were key contributors. Additionally: Rural women carrying heavy loads on their heads experience accelerated cervical degeneration. Drivers and manual laborers face repetitive neck strain. This dual urban-rural burden highlights the urgent need for awareness, preventive physiotherapy, and workplace ergonomics in India. Myths vs Facts Myth 1: Only old people get cervical spondylosis.Fact: Younger adults are increasingly being diagnosed due
Physiotherapy for Cervical Pain: Effective Techniques and Benefits
Physiotherapy for Cervical Pain: Effective Techniques and Benefits Neck pain has quietly become one of the most common health challenges of modern times. If you live in a city, you’ve probably seen colleagues rubbing their necks after long meetings, friends complaining of stiffness after late-night phone scrolling, or even family members struggling to turn their heads in the morning. In fact, cervical pain — often linked to cervical spondylosis, cervical disc issues, or muscle strain — is now considered a global musculoskeletal concern. According to the World Health Organization (WHO), musculoskeletal conditions are among the leading causes of disability worldwide, and neck pain is consistently reported as one of the top contributors. A large population-based study published in The Lancet revealed that neck pain affects more than 20% of people at some point in their lives. In India, urban professionals are particularly vulnerable due to long desk hours, while manual workers in rural areas develop cervical problems from repetitive strain and heavy lifting. This growing burden of cervical pain highlights the importance of safe, effective, and sustainable solutions. While medications can reduce pain temporarily, they rarely fix the root cause. Surgery, although necessary in some advanced cases, is invasive and not always required. Physiotherapy, on the other hand, has emerged as one of the most evidence-backed, non-invasive, and patient-friendly approaches for cervical pain management. In this article, we’ll take a deep dive into: What cervical pain really is and why it happens. The science of physiotherapy for cervical spine problems. Evidence-based physiotherapy techniques and their benefits. Exercises, ergonomic tips, and preventive strategies. The role of physiotherapy in India’s growing cervical pain epidemic. When to seek professional help. Our aim is to make this a comprehensive, factual, and actionable guide for anyone struggling with cervical discomfort or looking to protect their neck health for the future. Understanding Cervical Pain What is Cervical Pain? The cervical spine is the uppermost part of the spinal column, consisting of seven vertebrae (C1–C7). This region supports the skull, allows head movement, and protects vital nerves that connect the brain to the rest of the body. Because of its flexibility and constant use, the cervical spine is highly prone to wear and tear, postural strain, and injury. Cervical pain typically refers to: Localized pain in the neck region. Stiffness or reduced range of motion. Pain radiating to shoulders, arms, or upper back. In severe cases, nerve compression symptoms like tingling or numbness. Common Causes of Cervical Pain Medical literature highlights several causes, many of which overlap due to lifestyle and ageing factors: Poor Posture Forward head posture from laptops and phones. Slouching during long desk hours. Muscle Strain Prolonged sitting without breaks. Heavy lifting or sudden jerks. Degenerative Changes Cervical spondylosis (age-related disc and joint wear). Osteoarthritis of the neck joints. Disc Problems Herniated or bulging cervical discs pressing on nerves. Trauma or Accidents Whiplash injuries from car accidents. Sports injuries. Lifestyle Factors Stress and anxiety leading to neck muscle tension. Lack of physical activity. Other Medical Conditions Infections, inflammatory disorders, or tumors (rare but important). Symptoms to Watch Out For Persistent neck stiffness. Sharp or aching pain in the neck. Radiating pain to shoulders or arms. Tingling or numbness in fingers. Weakness in grip strength. Headaches starting from the base of the skull. Dizziness or balance issues in severe cervical spondylosis. Understanding these causes and symptoms is the first step before exploring how physiotherapy can help. Why Physiotherapy is Essential for Cervical Pain Physiotherapy stands out for one main reason: it treats the root cause rather than masking symptoms. Evidence-Based Benefits of Physiotherapy According to the National Institute for Health and Care Excellence (NICE, UK) and multiple studies indexed on PubMed, physiotherapy is highly effective for non-specific neck pain, cervical spondylosis, and disc-related conditions. Key advantages include: Non-invasive: Avoids risks of surgery. Drug-free: Reduces dependency on painkillers. Personalized: Tailored programs for each patient. Restorative: Improves function and mobility. Preventive: Reduces risk of recurrence. How Physiotherapy Works Physiotherapy combines manual therapy, exercises, ergonomic advice, and patient education to: Reduce pain and inflammation. Restore range of motion. Strengthen supporting muscles. Correct postural imbalances. Relieve pressure on nerves. Improve blood flow and tissue healing. Instead of offering just short-term comfort, physiotherapy focuses on long-term recovery and prevention. Physiotherapy Techniques for Cervical Pain Here’s a detailed look at evidence-based techniques: 1. Manual Therapy Hands-on mobilization to restore normal movement and reduce stiffness. Joint Mobilization – Gentle oscillations applied to stiff cervical joints. Soft Tissue Manipulation – Massage to reduce muscle tightness. Myofascial Release – Targets deep connective tissue. 2. Exercise Therapy Central to every physiotherapy program. Range of Motion Exercises – Neck rotations, side bends. Strengthening Exercises – Chin tucks, isometric holds, scapular retractions. Stretching – Trapezius and levator scapula stretches. Postural Training – Reversing forward head posture. 3. Electrotherapy Machines that stimulate muscles and nerves. TENS (Transcutaneous Electrical Nerve Stimulation). Ultrasound Therapy – Promotes deep tissue healing. Interferential Therapy (IFT) – Pain modulation. 4. Heat and Cold Therapy Moist Heat Packs – Increase circulation and relax muscles. Cold Packs – Reduce inflammation in acute injuries. 5. Cervical Traction Gentle pulling force that relieves nerve compression by creating space between vertebrae. 6. Ergonomic Guidance Advice on correct sitting posture, workstation setup, and sleeping habits. 7. Neurodynamics Special mobilizations for compressed or irritated nerves. 8. Relaxation and Breathing Exercises Stress management reduces muscle tension and prevents flare-ups. Benefits of Physiotherapy for Cervical Pain Short-Term Benefits Pain reduction. Relief from stiffness. Muscle relaxation. Improved neck mobility. Long-Term Benefits Strengthened neck and shoulder muscles. Corrected posture. Reduced recurrence. Improved daily functioning. Psychological Benefits Reduced fear of chronic pain. Empowerment through self-care strategies. Exercises You Can Try at Home Always consult a physiotherapist first. Chin Tucks – Gently pull chin backward. Neck Rotations – Slowly look left and right. Upper Trapezius Stretch – Tilt head sideways. Scapular Retractions – Pinch shoulder blades together. Isometric Neck Exercises – Press head against hand without moving. Consistency is key. Doing these daily can significantly reduce cervical pain risk. Ergonomics & Lifestyle Modifications Desk Setup Screen at eye level. Chair with lumbar and cervical support. Keyboard and mouse at comfortable height. Daily Habits Take breaks every 30–45 minutes. Avoid long hours on smartphones (“tech neck”). Use
Acute vs Chronic Back Pain: Key Differences You Need to Know
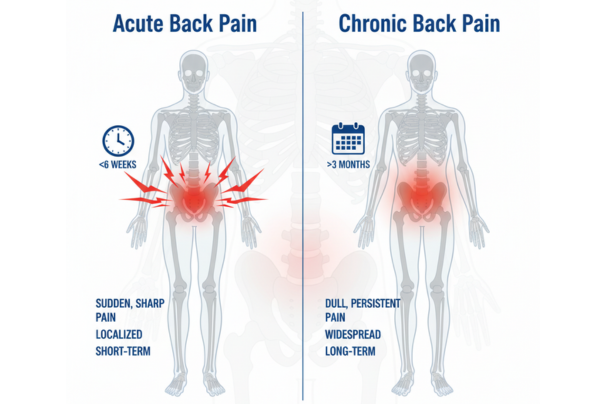
Acute vs Chronic Back Pain: Key Differences You Need to Know Back pain is one of the most common reasons people visit a doctor or physiotherapist. According to the World Health Organization (WHO), nearly 80% of adults experience back pain at least once in their lifetime. In India, lifestyle shifts — from sedentary desk jobs in urban areas to heavy physical labor in rural regions — have made back pain a widespread issue across all age groups. But not all back pain is the same. Some cases resolve within days or weeks, while others persist for months or even years, affecting daily life and work. Medical experts categorize back pain into two main types: acute back pain and chronic back pain. Understanding the differences between these two is crucial because their causes, treatment approaches, and long-term management strategies can vary significantly. Misunderstanding or ignoring these differences may lead to delayed recovery or worsening of the condition. This blog breaks down everything you need to know about acute and chronic back pain — their key differences, causes, symptoms, diagnostic methods, treatment options, and preventive measures — using real, evidence-based medical facts. What is Back Pain? Back pain refers to discomfort, stiffness, or aching in the spine and surrounding muscles. It can affect any region, but the lower back (lumbar spine) is the most common site because it bears much of the body’s weight and is involved in almost every movement. Types of Back Pain Based on Duration Acute Back Pain: Lasts less than 6 weeks. Subacute Back Pain: Lasts between 6–12 weeks. Chronic Back Pain: Persists for 12 weeks or longer, even after the initial injury or underlying cause has been treated. This time-based classification is endorsed by the American College of Physicians (ACP) and the National Institutes of Health (NIH). Acute Back Pain Definition Acute back pain is short-term pain that comes suddenly and usually improves within a few days to weeks. It is often the result of a specific event or injury. Common Causes Muscle strain or ligament sprain. Lifting heavy objects improperly. Sudden awkward movement. Sports injuries. Minor disc irritation. Postural stress after prolonged sitting or standing. Symptoms Sharp, stabbing pain localized in one area. Muscle spasms. Pain that improves with rest. Stiffness or difficulty bending. Prognosis Most cases of acute back pain improve significantly within 2–6 weeks with proper self-care, rest, and sometimes physiotherapy. Chronic Back Pain Definition Chronic back pain is defined as pain that lasts 12 weeks or longer, often continuing despite initial treatments. It may start as acute pain but persist due to underlying causes. Common Causes Degenerative disc disease. Herniated or bulging discs. Spinal stenosis (narrowing of spinal canal). Osteoarthritis of the spine. Poor posture and sedentary lifestyle. Previous injuries that did not heal completely. Conditions like ankylosing spondylitis or osteoporosis. Symptoms Dull, aching pain that may radiate to hips or legs. Stiffness and limited mobility. Pain worsens with prolonged sitting or standing. Numbness or tingling if nerves are involved. Episodes of flare-ups and remissions. Prognosis Chronic back pain often requires long-term management rather than quick fixes. It may not always be curable but can be controlled with physiotherapy, lifestyle modifications, medications, and sometimes surgery. Acute vs Chronic Back Pain – Key Differences Feature Acute Back Pain Chronic Back Pain Duration Less than 6 weeks 12+ weeks Onset Sudden, after injury or strain Gradual or persistent Cause Often identifiable (lifting, twisting, fall) Often degenerative or multifactorial Symptoms Sharp, stabbing, improves with rest Dull, aching, persists, may radiate Treatment Rest, short-term physiotherapy, pain relief Long-term rehab, posture correction, medication, surgery if severe Prognosis Resolves with conservative care Requires ongoing management Diagnosis of Back Pain Healthcare providers use: Physical Examination – Posture, range of motion, neurological checks. Imaging (if needed):-X-rays for bone changes.-MRI/CT for discs and nerves. Blood Tests if systemic disease suspected. Diagnosis is essential to differentiate between simple acute pain and more complex chronic conditions. Treatment Approaches Acute Back Pain Treatment Rest (short-term only). Ice/heat therapy. Over-the-counter pain relievers (paracetamol, NSAIDs). Physiotherapy for guided exercises. Gradual return to activity. Chronic Back Pain Treatment Physiotherapy and exercise therapy (core strengthening, flexibility training). Posture correction & ergonomics. Pain management: medications, nerve blocks, or injections. Cognitive-behavioral therapy (CBT) to cope with chronic pain. Surgical options (for severe cases like herniated disc or spinal stenosis). Physiotherapy’s Role in Both Physiotherapy is vital for both acute and chronic back pain: Restores mobility. Strengthens supporting muscles. Improves posture. Prevents recurrence. Provides patient education for long-term management. Prevention Tips for Back Pain Maintain healthy posture at desk and while standing. Take regular breaks during long sitting. Practice core strengthening exercises (planks, bridges). Lift objects properly (bend knees, not waist). Maintain healthy body weight. Ensure ergonomic furniture. Avoid prolonged inactivity. Back Pain in India – An Alarming Trend Studies in India have shown: Up to 60% of the Indian population suffers from back pain at some point. IT professionals are at particularly high risk. Women in rural areas often face chronic back pain from carrying heavy loads. This highlights the urgent need for awareness and preventive strategies. When to See a Doctor Pain persists beyond a few weeks. Weakness, numbness, or tingling in legs. Loss of bladder or bowel control (medical emergency). Pain following major trauma. The Role of We Are Spine At We Are Spine, back pain is addressed through comprehensive diagnosis and personalized care. The team emphasizes: Advanced physiotherapy techniques. Ergonomic corrections. Preventive lifestyle advice. Minimally invasive interventions when necessary. The goal is not just short-term relief but sustainable spinal health for the long term. Conclusion Back pain may be universal, but its types — acute and chronic — are very different in how they start, progress, and require treatment. Acute pain often resolves quickly with simple measures, while chronic pain demands consistent, multi-faceted care. By understanding these differences, patients can seek the right help at the right time. Physiotherapy, posture correction, and healthy lifestyle habits remain the backbone of both prevention and recovery. Whether you’re an
Is Sciatica the Same as Lower Back Pain? Understanding the Connection
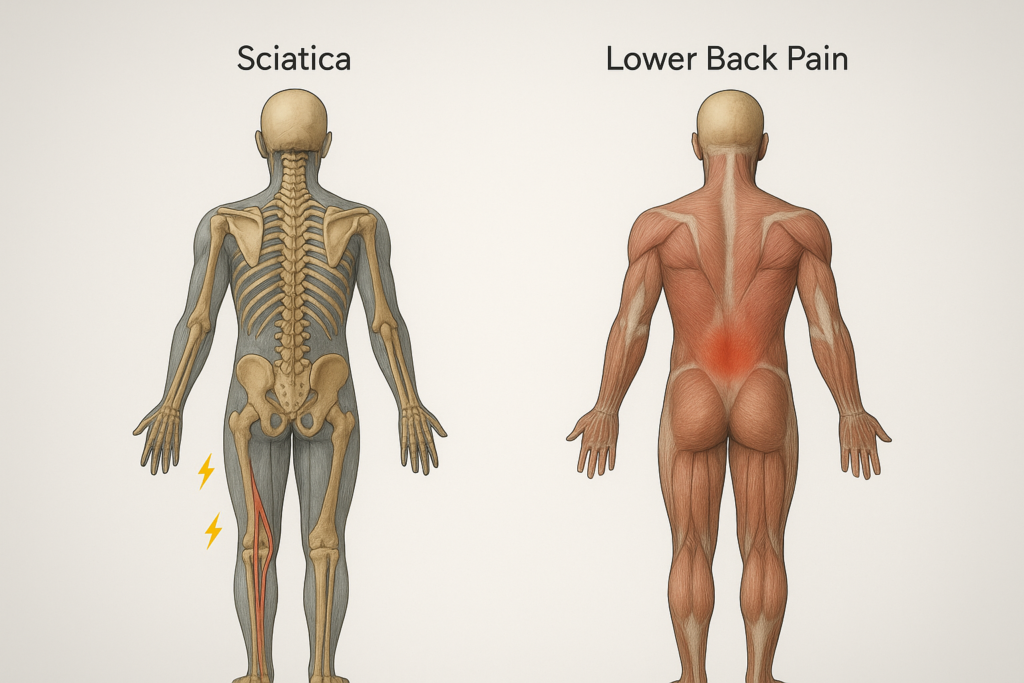
Is Sciatica the Same as Lower Back Pain? Understanding the Connection If you’ve ever felt a nagging ache in your lower back after hours of sitting, or a sharp, shooting pain that travels down your leg, you might have wondered if they’re the same problem. Many people lump both experiences under the umbrella of “back pain.” In reality, lower back pain and sciatica are related but distinct conditions. This confusion is widespread. Both affect the same region, both can make even simple activities — like bending, sitting, or walking — difficult, and both are increasingly common in India’s working population. However, knowing the difference between the two is critical, because the underlying causes and treatment approaches often differ. In this blog, we’ll explore what sciatica and lower back pain actually mean, how to tell them apart, why they sometimes overlap, and the best ways to manage and prevent them. By the end, you’ll have the clarity you need to better understand your spine health and when to seek medical help. Understanding Lower Back Pain What Is Lower Back Pain? Lower back pain (LBP) is one of the most common health complaints globally. The World Health Organization (WHO) estimates that up to 70% of adults will experience back pain at some point in their lives. In India, studies show that nearly one in five adults suffer from chronic low back pain. Lower back pain is not a disease in itself; rather, it is a symptom that can result from multiple underlying issues. It can range from mild stiffness to severe, disabling pain. Types of Lower Back Pain Medical professionals usually divide lower back pain into categories: Mechanical Back Pain – Stemming from muscles, ligaments, joints, or spinal structures. This is the most common type. Inflammatory Back Pain – Associated with autoimmune conditions like ankylosing spondylitis. Referred Pain – When pain from another organ (like the kidneys or pancreas) is felt in the lower back. Common Causes Some of the most frequent triggers of lower back pain include: Muscle or ligament strain due to heavy lifting or awkward movement. Degenerative disc disease and age-related changes. Herniated discs, which may or may not cause nerve symptoms. Spinal stenosis, a narrowing of the spinal canal. Poor posture and prolonged sitting. Fractures due to osteoporosis in older adults. Symptoms of Lower Back Pain Dull or aching pain localized to the lumbar area. Stiffness, especially after rest. Pain that worsens with sitting or standing for long periods. Limited flexibility. Muscle spasms. Understanding Sciatica What Is Sciatica? Sciatica refers to pain caused by irritation or compression of the sciatic nerve — the longest nerve in the body, running from the lower spine down through the buttocks, thighs, calves, and feet. Unlike generalized back pain, sciatica follows a clear nerve pathway and is usually one-sided. Causes of Sciatica Herniated or slipped disc pressing on the nerve. Lumbar spinal stenosis narrowing nerve spaces. Bone spurs due to arthritis. Spondylolisthesis (vertebral slippage). Piriformis syndrome, where a small muscle in the buttocks irritates the sciatic nerve. Symptoms of Sciatica Sharp, shooting pain radiating down one leg. Tingling, pins-and-needles sensation. Numbness or weakness in the leg or foot. Pain aggravated by coughing, sneezing, or long sitting. Typically affects only one side of the body. Symptoms often worsen when sitting, bending, or coughing, and may improve when lying down. Diagnosis: How Doctors Confirm a Herniated Disc Diagnosis combines medical history, physical exam, and imaging tests: 1. Physical Examination Checking reflexes, muscle strength, walking ability, and sensation. Straight leg raise test for lumbar herniation. 2. Imaging Tests MRI: Gold standard for identifying herniation and nerve compression. CT Scan: Helpful when MRI isn’t possible. X-ray: Rules out other spine problems but doesn’t show discs. 3. Nerve Tests Electromyography (EMG): Measures electrical activity of muscles. Nerve conduction studies: Show how well electrical signals travel. Sciatica vs. Lower Back Pain: Key Differences Feature Lower Back Pain Sciatica Location Centralized in lumbar spine Radiates down buttock, thigh, leg Pain Type Dull, aching, stiff Sharp, shooting, burning Nerve Involvement Not always Always involves sciatic nerve Laterality Can be both sides Usually one side Additional Symptoms Stiffness, muscle spasm Numbness, tingling, weakness Summary: All sciatica involves back pain, but not all back pain is sciatica. Why People Confuse the Two Both start in the lower back region. Both can make walking or sitting painful. Disc problems can cause either or both. In early stages, pain may feel similar before radiation sets in. The Impact of Lifestyle on Both Sedentary Jobs Office workers sitting for 8–10 hours a day are at high risk. Poor ergonomics and lack of movement weaken spinal muscles and increase disc pressure. Heavy Physical Labor In rural India, farmers and laborers often develop back pain or disc injuries due to repetitive heavy lifting. Obesity Excess body weight adds load to the lumbar spine, worsening both conditions. Vitamin D Deficiency Widespread in India, this weakens bones and contributes to disc problems. How Sitting Too Long Affects the Spine Increases spinal disc pressure by up to 40% compared to standing. Weakens core muscles. Stiffens hip flexors, pulling on the spine. Increases risk of disc herniation. A Harvard Health study shows that microbreaks and movement reduce back pain by improving circulation and reducing muscle fatigue. Diagnosis: How Doctors Differentiate Physical Examination Straight Leg Raise (SLR) Test for sciatica. Palpation of muscles and movement tests for general back pain. Imaging X-rays to rule out fractures. MRI for disc herniation or stenosis. CT scan if MRI isn’t possible. Nerve Tests Electromyography (EMG) can confirm nerve irritation in sciatica. Treatment Approaches Conservative Treatments (Both Conditions) Rest (short term only). Heat or ice therapy. NSAIDs (non-steroidal anti-inflammatory drugs). Physiotherapy and guided exercise. Ergonomic corrections at workplace/home. Sciatica-Specific Treatments Epidural steroid injections. Nerve mobilization techniques. Surgery (like microdiscectomy) for severe cases. Lower Back Pain-Specific Treatments Core strengthening for stabilization. Lifestyle modification (weight loss, posture training). Alternative therapies (yoga, acupuncture, though evidence varies). Prevention Strategies At Work Take a break every 30–45 minutes. Adjust chair height so feet rest flat. Keep screens at eye level. At Home Sleep on a medium-firm mattress. Exercise regularly (swimming, walking, yoga). Avoid lifting with the back — bend at the knees instead. Nutrition Adequate calcium
What causes a Herniated Disc and how is it treated?
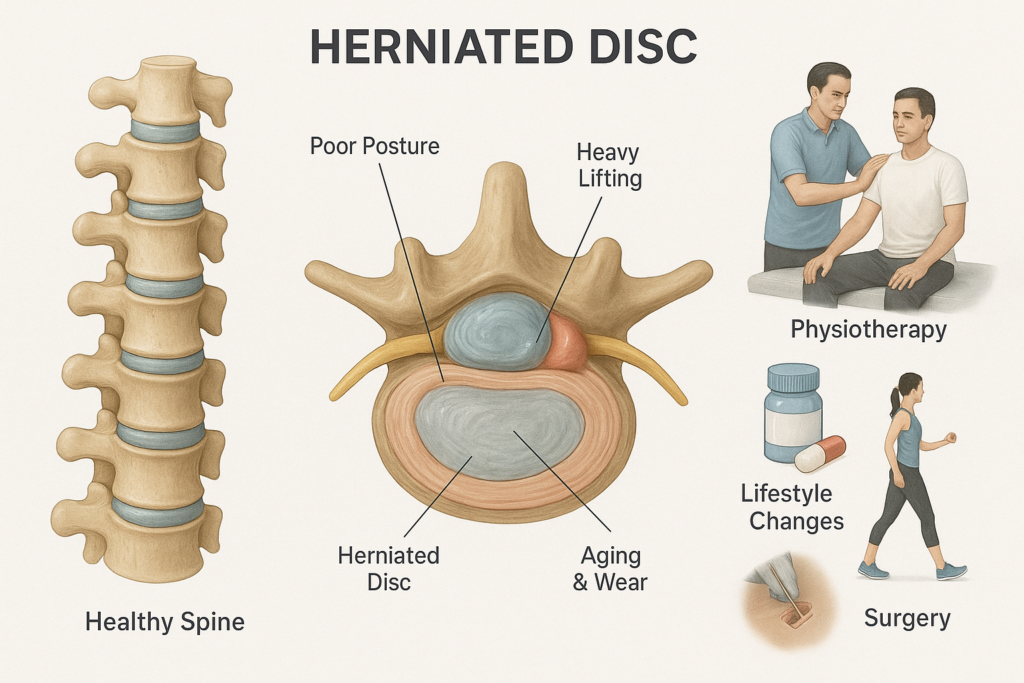
What causes a Herniated Disc and how is it treated? Why Herniated Discs Are So Common Today Back pain is one of the most widespread health problems worldwide, and a leading cause of missed work. Among its many causes, one condition stands out as both common and often misunderstood — the herniated disc (also known as a slipped or ruptured disc). A herniated disc occurs when the soft, gel-like center of a spinal disc pushes out through a tear in its tough outer layer. This can irritate or compress nearby spinal nerves, leading to pain, numbness, tingling, or weakness in the back, neck, arms, or legs. According to the National Institutes of Health (NIH), herniated discs are most common in people aged 30 to 50, but they can occur at any age depending on lifestyle and risk factors. With the rise of sedentary desk jobs, long screen hours, and poor posture habits, cases of spinal disc problems are increasing, especially in countries like India. This blog explains the condition in detail: What a herniated disc is What causes it Symptoms and risk factors How doctors diagnose it Treatment options (both non-surgical and surgical) Recovery and long-term prevention All information here is strictly factual, based on trusted medical organizations like the World Health Organization (WHO), Mayo Clinic, Cleveland Clinic, and peer-reviewed studies. Understanding the Spine and Spinal Discs To understand how and why discs herniate, it helps to first look at the spine’s structure. The human spine is made up of 33 vertebrae stacked on top of each other. Between most of these bones lie intervertebral discs, which act like cushions or shock absorbers. Each disc has two parts:-Nucleus pulposus: A soft, gel-like center that provides flexibility and cushioning.-Annulus fibrosus: A tough, fibrous outer ring that keeps the nucleus in place. These discs allow the spine to bend, twist, and absorb everyday forces from walking, lifting, or even sitting. A herniated disc happens when part of the nucleus pulposus pushes through a crack in the annulus fibrosus. This protrusion can: Compress spinal nerves Cause local inflammation Lead to symptoms ranging from mild discomfort to severe pain and weakness What Causes a Herniated Disc? 1. Age-Related Degeneration The most common cause is natural aging. As people grow older: Discs lose water content, becoming less flexible. The annulus fibrosus weakens, making tears more likely. Even minor stresses (bending, twisting, coughing) can trigger herniation. This process is called degenerative disc disease, and it explains why herniated discs are common after age 30. 2. Repetitive Strain and Poor Posture Modern desk jobs put enormous stress on spinal discs. Prolonged sitting increases lumbar disc pressure by 40% compared to standing (Nachemson’s biomechanical study, 1970s). Poor posture — slouching, hunching, forward head tilt — makes it worse. Over time, this continuous strain weakens discs, setting the stage for herniation. 3. Heavy Lifting or Sudden Strain Lifting heavy objects incorrectly (bending at the waist instead of the knees) is a major cause. The sudden load on the lumbar spine can tear the annulus and push the nucleus outward. 4. Obesity Excess body weight adds constant pressure on the lumbar spine. According to the Mayo Clinic, obesity is a significant risk factor for disc herniation, especially in the lower back. 5. Sedentary Lifestyle Lack of physical activity weakens the core and back muscles that support the spine. Weak support means more stress falls on the discs, making them vulnerable. 6. Smoking Studies in Spine Journal show smoking reduces oxygen supply to discs, accelerating degeneration and slowing healing. 7. Genetics Some people inherit weaker disc structures, making them prone to herniation earlier in life. 8. Occupational Risks Jobs involving repetitive lifting, twisting, driving, or vibration (e.g., truck driving, construction work) increase risk. On the other hand, long hours of office work without movement also contribute to disc damage. 9. Pregnancy During pregnancy, hormonal changes loosen ligaments, while added weight and posture shifts increase spinal stress, raising the risk of disc problems. Symptoms: How to Recognize a Herniated Disc Not everyone with a herniated disc has symptoms. But when nerves are compressed, typical signs include: 1. Pain Lumbar herniation (lower back): Pain radiates to buttocks, thighs, and legs (sciatica). Cervical herniation (neck): Pain spreads to shoulders, arms, and hands. 2. Numbness or Tingling Affected nerves may cause sensations of pins and needles in arms, hands, legs, or feet. 3. Muscle Weakness Compression reduces nerve signals, making it hard to lift objects, grip firmly, or walk steadily. 4. Worsening with Movement Symptoms often worsen when sitting, bending, or coughing, and may improve when lying down. Red Flags (Seek Immediate Medical Help): Loss of bladder or bowel control Severe weakness in legs Numbness in the inner thighs or around the anus (cauda equina syndrome — a medical emergency) Diagnosis: How Doctors Confirm a Herniated Disc Diagnosis combines medical history, physical exam, and imaging tests: 1. Physical Examination Checking reflexes, muscle strength, walking ability, and sensation. Straight leg raise test for lumbar herniation. 2. Imaging Tests MRI: Gold standard for identifying herniation and nerve compression. CT Scan: Helpful when MRI isn’t possible. X-ray: Rules out other spine problems but doesn’t show discs. 3. Nerve Tests Electromyography (EMG): Measures electrical activity of muscles. Nerve conduction studies: Show how well electrical signals travel. Treatment: How Is a Herniated Disc Managed? Most patients improve without surgery. The American Association of Neurological Surgeons (AANS) notes that 90% of herniated disc cases improve within 6 weeks with conservative treatment. Non-Surgical Treatments 1. Rest and Activity Modification Avoid heavy lifting and bending. Bed rest is discouraged; light activity aids recovery. 2. Medications NSAIDs (ibuprofen, naproxen): Reduce pain and inflammation. Muscle relaxants: For spasms. Nerve pain drugs (gabapentin, pregabalin): For radiating pain. Corticosteroid injections: Provide temporary relief. 3. Physical Therapy Supervised exercises help: Strengthen core muscles. Improve flexibility. Correct posture and body mechanics. Relieve nerve pressure. 4. Heat and Cold Therapy Cold packs reduce inflammation; heat relieves stiffness. 5. Lifestyle Modifications Weight management. Quitting smoking. Ergonomic workstations. Regular stretching
Spine-Friendly Diet: What to Eat for Bone and Disc Health

Spine-Friendly Diet: What to Eat for Bone and Disc Health The human spine is an engineering marvel — 33 vertebrae stacked in perfect alignment, cushioned by discs, connected by ligaments, powered by muscles, and guarding the spinal cord. But what happens when that silent, dependable structure starts to send signals of distress? That dull ache in your lower back after a long day, or the stiffness you feel getting out of bed, could be more than just a sign of aging. They could be your spine’s way of telling you its building blocks are weakening. While posture, exercise, and ergonomics play important roles in spine health, nutrition is the foundation. The quality of your spinal structure depends directly on the fuel you give it. A well-balanced diet rich in the right nutrients can: Strengthen spinal bones Maintain disc hydration and flexibility Reduce inflammation and pain Support faster recovery after injury This in-depth guide — backed by WHO, Indian Council of Medical Research (ICMR), and peer-reviewed studies — will take you through: Nutrients essential for spinal bones and discs Best Indian diet sources for each nutrient Foods to limit or avoid Hydration’s role in spine health Vegetarian & vegan adaptations Detailed 7-day spine health meal plan with recipes Nutrient-to-food reference chart Why Diet Matters for Spine Health The spine’s bones (vertebrae) require dense mineralization to handle weight-bearing loads. The intervertebral discs — soft cushions between vertebrae — are mostly water, collagen, and proteoglycans, which rely on a constant supply of amino acids, vitamins, and minerals. Deficiencies can cause: Osteoporosis: Weak, brittle vertebrae prone to fractures Disc degeneration: Loss of cushioning and flexibility Inflammation: Chronic pain and stiffness Scientific insight: ICMR (2020) reports that calcium and vitamin D deficiencies are prevalent in both rural and urban India, contributing to poor bone health. WHO guidelines emphasize the role of balanced micronutrient intake for musculoskeletal longevity. Key Nutrients for Bone & Disc Health Calcium – The Bone Builder -Role: Structural backbone of bones; essential for vertebral strength. -RDA: 1000 mg/day for adults (ICMR). -Indian sources: Dairy: Milk (240 mg/cup), curd (200 mg/100 g), paneer (208 mg/100 g) Plant-based: Ragi (344 mg/100 g), sesame seeds (975 mg/100 g), amaranth leaves (215 mg/100 g), drumstick leaves (440 mg/100 g) Fortified options: Fortified soy/almond milk (~300 mg/cup) -Recipe idea: Ragi malt with jaggery and milk — calcium + iron combo. Vitamin D – The Calcium Absorption Key – Role: Enables intestinal absorption of calcium. – RDA: 600–800 IU/day. – Sources: Sunlight: 15–20 min, 3–4 times/week (mid-morning or late afternoon) Foods: Sardines (272 IU/100 g), mackerel (360 IU/100 g), egg yolk (37 IU), fortified milk (100 IU/cup) – Note: A 2019 study in Indian Journal of Endocrinology and Metabolism found over 70% of Indians have low vitamin D. Magnesium – The Bone & Muscle Relaxant – Role: Works with calcium to form bone; prevents muscle cramps. – RDA: 320 mg/day for women, 420 mg/day for men. – Sources: Pumpkin seeds (262 mg/100 g), almonds (270 mg/100 g), spinach (79 mg/100 g), bajra (137 mg/100 g). Protein – The Structural Support – Role: Builds muscle tissue that supports the spine and repairs ligaments/discs. – RDA: 0.8–1 g/kg body weight. – Sources: Lentils, chickpeas, kidney beans, eggs, lean meats, paneer, soy products. Omega-3 Fatty Acids – The Anti-Inflammatory Ally – Role: Reduce inflammation in spinal joints and discs. – Sources: Non-veg: Sardines, mackerel, salmon Veg: Flaxseeds (2.35 g ALA/1 tbsp), chia seeds (1.75 g ALA/1 tbsp), walnuts (2.5 g ALA/28 g) Vitamin C – The Collagen Maker – Role: Essential for collagen synthesis in discs, ligaments, and tendons. – Sources: Amla (600 mg/100 g), guava (228 mg/100 g), orange (53 mg/100 g), capsicum (80 mg/100 g). Zinc – The Repair Agent – Role: Tissue healing and immunity. – Sources: Pumpkin seeds, cashews, chickpeas, oysters, chicken. Quick Nutrient-to-Food Reference Chart Nutrient Role Indian Veg Sources Indian Non-Veg Sources Calcium Bone strength Ragi, sesame, drumstick leaves Milk, paneer, curd Vitamin D Calcium absorption Fortified plant milk Sardines, mackerel, egg yolk Magnesium Bone/muscle health Nuts, spinach, bajra Fish Protein Muscle & tissue repair Lentils, soy, chickpeas Chicken, eggs Omega-3 FA Anti-inflammatory Flaxseeds, walnuts Sardines, mackerel Vitamin C Collagen formation Amla, guava, citrus Liver, fish roe Zinc Tissue repair Nuts, seeds, pulses Meat, seafood Foods to Limit or Avoid The following foods can actively work against your spine’s health. Limiting or avoiding them can be as important as eating the right foods. Sugary drinks & sweets: The Inflammation Accelerators. Excessive sugar intake can cause systemic inflammation throughout your body, including in your spinal discs and joints. This chronic inflammation can lead to increased pain and stiffness, and it also hinders your body’s ability to heal and repair tissue. High-salt foods: The Calcium Thieves. A diet high in salt forces your kidneys to excrete more sodium, and unfortunately, calcium often gets flushed out with it. This process can contribute to bone density loss over time, weakening your vertebrae and increasing the risk of osteoporosis. Refined grains: Empty Calories & Missing Magnesium. Foods like white bread and polished rice have been stripped of their nutritional value, including fiber and key minerals like magnesium. Replacing them with whole grains (e.g., bajra, ragi, brown rice) ensures you get a steady supply of nutrients essential for bone health. Excessive caffeine: A Calcium Compromise. While a morning cup of coffee is fine, consuming too much caffeine (more than 2–3 cups per day) can interfere with your body’s ability to absorb calcium and may contribute to its excretion. Alcohol & smoking: Accelerated Degeneration. Both alcohol and smoking have been shown to accelerate disc degeneration. They impair blood flow to the spine, depriving the discs of the oxygen and nutrients they need to stay hydrated and healthy. Hydration & Spine Health Discs are 70–90% water. Even mild dehydration can reduce disc height and flexibility. Daily goal: 2–3 litres of water Add coconut water, lemon water, and high-water fruits like watermelon and cucumber Vegetarian & Vegan Tips for Spine Health For calcium: Ragi porridge, sesame laddoos, drumstick leaf curry For vitamin D: Fortified plant milks, mushrooms exposed to sunlight For omega-3: Ground flaxseed in rotis or smoothies Protein: Soy chunks curry, lentil soups, chickpea salads