Inherited or Preventable? The Role of Genetics in Spine Health

Inherited or Preventable? The Role of Genetics in Spine Health The spine is one of the most crucial structures in the human body, supporting the entire weight of the body and enabling movement. While most people are aware that external factors like posture and injury can affect spine health, fewer realize that genetics—the DNA we inherit from our parents—also plays a significant role. In this article, we’ll explore how genetics influences spine health, the specific conditions that are inherited, and how they may affect future generations. What is the Role of Genetics in Spine Health? Genetics refers to the information contained in our DNA that influences everything from eye colour to susceptibility to diseases. In terms of spine health, genetic factors control the growth, structure, and function of the spine. This includes the bones (vertebrae), discs between the vertebrae, spinal ligaments, and muscles that support the spine. Genetic Factors Influencing Spine Health 1. Bone Development and Strength: One of the most direct ways genetics influences spine health is through the development of bone strength and density. Bone health is largely determined by the production of collagen and other proteins, which are encoded by genes. If a person inherits a genetic makeup that results in weaker bones or lower bone density, they may be more susceptible to spinal fractures or degenerative conditions as they age. Example: A person with a family history of osteoporosis (a condition in which bones become fragile and more prone to fractures) may inherit genes that make them more likely to develop this condition, leading to problems like spinal compression fractures in the vertebrae. 2. Spinal Alignment and Scoliosis: Scoliosis, an abnormal curvature of the spine, can often run in families. Certain genetic variations are linked to an increased likelihood of developing scoliosis, particularly during adolescence when growth spurts occur. Example: If a parent has idiopathic scoliosis (a form of scoliosis with no known cause), there is a slightly higher chance that their child may also develop it, though environmental factors and lifestyle also play a role. Some genetic syndromes, such as Marfan syndrome or Ehlers-Danlos syndrome, which are inherited, can cause spinal curvature or hypermobility in the joints, leading to scoliosis or other spinal problems. 3. Genetic Conditions Leading to Spinal Problems: Several genetic disorders specifically affect spine health. These conditions usually arise due to mutations or inherited traits that affect the structure of connective tissues or bones, making the spine more prone to issues. Ankylosing Spondylitis (AS): A type of arthritis that primarily affects the spine, AS causes inflammation in the vertebrae, leading to pain and stiffness. Over time, the inflammation can cause the spine to fuse, reducing flexibility. AS is strongly linked to the HLA-B27 gene, and individuals who inherit this gene from their parents have a much higher risk of developing AS. Example: A child whose parent has ankylosing spondylitis may be genetically predisposed to develop the condition. However, not all people with the HLA-B27 gene will develop AS, suggesting that environmental factors, such as infections, also contribute to its onset. 4. Degenerative Disc Disease: Degenerative Disc Disease (DDD) occurs when the intervertebral discs, which cushion the spine, begin to break down. This condition is linked to aging, but genetics also plays a significant role in how quickly the discs degrade. Certain genetic markers have been identified that predict an individual’s risk for developing DDD at an earlier age. Example: If both parents suffer from early-onset degenerative disc disease, their children might inherit a genetic tendency for faster disc degeneration, making them more likely to experience back pain and reduced mobility in their 40s or 50s. Will Children Definitely Have Spine-Related Issues from Their Parents? While there is a genetic influence on spine health, children will not necessarily develop the same spinal issues as their parents, even if there is a family history. Here’s why: 1. Genetic Risk Does Not Mean Certainty: Just because a parent has a certain spinal condition doesn’t mean the child will automatically develop it. While some conditions have a genetic component, many also depend on other factors like environment, lifestyle, and overall health. For instance, conditions like osteoarthritis or scoliosis may develop more strongly due to factors like injury, lifestyle choices (e.g., physical activity level), or even diet. 2. Multifactorial Inheritance: Many spinal conditions are influenced by multiple genes and their interaction with environmental factors. This means that even if a child inherits some of the risk genes from their parents, the condition may not manifest unless certain environmental triggers (like posture problems or excessive physical strain) are present. 3. Genetic Variability: Even siblings who share the same parents may not inherit the same set of genes in the same way, leading to differences in their risk for spinal conditions. For example, one child may inherit a gene linked to weak collagen, making them more prone to spinal issues, while another child may not inherit the same gene or may inherit a different combination of genes that confer more robust spine health. 4. Preventive and Lifestyle Factors: Even with a genetic predisposition, children can often reduce their risk by maintaining a healthy lifestyle. Proper posture, regular physical activity, a balanced diet rich in calcium and vitamin D, and avoiding excessive strain on the spine can help prevent or delay the onset of many spine-related issues, even if they have a genetic risk. Conclusion In summary, genetics plays a vital role in the development and health of the spine, influencing conditions such as scoliosis, degenerative disc disease, osteoarthritis, and ankylosing spondylitis. However, having a genetic predisposition to these conditions does not guarantee their development. Environmental factors, lifestyle choices, and preventive care can significantly affect the outcomes. Understanding the role of genetics in spine health can help individuals make informed decisions about their health and take proactive steps to maintain a strong and healthy spine. By being aware of family history and engaging in healthy habits, individuals can reduce their risks and take control of their spine health, even when genetics may be working against them. Please enable JavaScript in your browser to complete this form.Please enable JavaScript in your browser to complete this form.Full Name *Email *Phone Number *
Revolutionizing Spine Surgery in 2025: How Robotics and Augmented Reality Are Changing the Game

Revolutionizing Spine Surgery in 2025: How Robotics and Augmented Reality Are Changing the Game In 2025, spine surgery has entered a groundbreaking era, thanks to the integration of cutting-edge technologies like robotics and augmented reality (AR). These innovations are not just enhancing the precision and efficiency of spinal procedures, but they’re also revolutionizing patient care, leading to faster recoveries and better outcomes. Traditional, invasive spinal surgeries are being replaced by minimally invasive, highly accurate procedures that allow patients to get back on their feet in record time. In this blog, we’ll dive into how these advanced technologies are transforming the landscape of spine surgery and what it means for both surgeons and patients alike. The Rise of Robotics in Spine Surgery Robotic-assisted spine surgery has come a long way since its inception. Instead of replacing surgeons, robots now assist in performing complex procedures with remarkable precision, offering several advantages for both the surgeon and the patient. How Robotics Work in Spine Surgery: Robotic systems such as Mazor X, ExcelsiusGPS, and ROSA Spine are equipped with advanced sensors and 3D imaging systems. These systems help surgeons plan and execute surgeries with millimetre-level precision. Here’s how it generally works: Pre-Surgical Planning: Surgeons use 3D imaging technology (CT scans or MRIs) to create a virtual model of the patient’s spine. Surgical Execution: Once the plan is set, the robotic system takes over the precise execution of the surgery. For example, when placing screws or implants, the robot guides the surgeon with accuracy based on the pre-planned images. Key Benefits of Robotics: Higher Precision: In complex spinal anatomies or deformities, robotic assistance ensures screws and implants are placed accurately. For instance, Mazor X has been shown to reduce pedicle screw misplacement from 13% in traditional surgeries to less than 2% in robotic surgeries. Less Tissue Damage: Traditional surgeries required large incisions, which often resulted in significant muscle and tissue damage. Robotic systems can plan a minimally invasive pathway that minimizes collateral damage to the muscles, tissues, and nerves around the spine. Reduced Surgical Time: The robot aids in speeding up the surgery by eliminating human error and providing precise guidance, reducing the time spent on each step of the operation. Lower Revision Rates: Robotic guidance means fewer mistakes during surgery, which leads to a lower chance of requiring corrective procedures. Improved Patient Outcomes: Less invasive procedures result in shorter recovery times, reduced postoperative pain, and patients often leave the hospital the same day. Example: ExcelsiusGPS, used in hospitals like the Mayo Clinic, allows surgeons to plan and guide their procedures accurately, ensuring that the surgery is performed as per the patient-specific anatomy with minimal complications. The Role of Augmented Reality (AR) in Spine Surgery AR in spine surgery is another groundbreaking development. With AR, surgeons can overlay 3D images of the spine onto the patient’s body, creating an immersive experience that allows them to “see through” layers of muscles and tissues. How AR Works in Spine Surgery: Surgeons wear AR headsets, like the xVision platform developed by Augmedics. The headset displays a real-time 3D hologram of the patient’s spine, mapped out in alignment with their body. This hologram is based on pre-surgical imaging data (CT or MRI scans). Surgeons can see the spine, vertebrae, and surrounding structures (nerves, blood vessels) in 3D while performing the surgery without having to look away to consult separate monitors. Key Benefits of AR: Real-time Anatomical Guidance: Surgeons get an interactive view of the anatomy while operating. This ability allows them to make precise decisions during minimally invasive surgeries. Improved Accuracy: Even when working with small or hard-to-see areas, AR provides a detailed view of the spinal anatomy, enhancing accuracy in placing screws, performing fusions, or correcting deformities. Better Ergonomics: Surgeons no longer need to frequently turn away from the patient to check images on a monitor. This reduces eye strain and fatigue, making it easier to focus on the procedure. Training and Education: AR allows medical students and surgical trainees to observe live surgeries with anatomical overlays, helping them learn faster and with more clarity. Example: xVision by Augmedics is already in use in several leading hospitals globally, offering surgeons the ability to perform surgery with enhanced visibility and precision. It helps surgeons maintain focus on the patient without the need to look at separate screens for guidance. When Robotics Meets AR: A Powerful Combination The integration of robotics and AR represents the cutting edge of spine surgery. When these technologies are used together, they allow surgeons to not only perform the surgery with robotic precision but also visualize the spine in 3D in real time, effectively combining the strengths of both. How Robotics and AR Work Together: Enhanced Spatial Awareness: The surgeon uses AR to visualize the spine in 3D while the robotic system guides the tools with extreme precision. Less Reliance on X-Rays: AR helps surgeons navigate without the need for constant X-ray imaging, reducing radiation exposure for both the surgeon and the patient. Speedier Procedures: The combination of robotic precision and AR visualization speeds up surgeries by reducing uncertainty and the need for corrective actions. Real-World Use Cases: Minimally Invasive Spinal Fusions: Robotic systems can place screws with precision, and AR provides a visual map of the vertebrae, ensuring minimal damage to surrounding tissue. Herniated Disc Repairs: The surgeon can use the AR headset to accurately identify the herniated disc and the robotic system can perform the repair with precision, ensuring the disc is removed without damaging the surrounding area. Spinal Deformity Corrections: For conditions like scoliosis or kyphosis, AR helps the surgeon visualize the exact correction needed, while the robot ensures the screws and implants are placed accurately. Example: The ROSA Spine robotic system, which is being used at hospitals like the Cleveland Clinic, integrates AR to give surgeons a live, enhanced view of the spine. This helps in performing highly complex procedures like scoliosis correction with improved results and lower risks. Global Adoption and Future Trends The integration of robotics and AR is happening worldwide. Notably: Apollo Hospitals and Medanta in India are
Spinal Nerves Explained: How Your Spine Powers Every Move You Make

Spinal Nerves: Functions, Types and How They Work We often hear the phrase “get to the root of the problem,” but when it comes to your body, the root of almost everything — movement, sensation, even basic survival functions like breathing — lies in your spinal nerves. Your spine is not just a structural pillar. It’s a superhighway of communication between your brain and the rest of your body, orchestrating a complex symphony of physical, autonomic, and sensory functions every second of the day. In this blog, we’ll take a deep dive into the spinal nerves, exploring their structure, purpose, and why even the tiniest damage to these nerves can result in life-altering consequences. Let’s journey down the spine — from the top of your neck to the base of your tailbone — and understand how these nerves shape your daily life. What Are Spinal Nerves? Your spinal nerves are part of the peripheral nervous system. You have 31 pairs of spinal nerves, and they branch off from the spinal cord through spaces between the vertebrae. These nerves are responsible for sending motor, sensory, and autonomic signals to and from your brain. Each nerve pair exits from a specific part of the spine and serves a specific area of the body, known as a dermatome (for sensory) or myotome (for muscle movement). The 31 pairs are divided into regions based on where they exit the spinal cord: 8 cervical nerves (C1–C8) 12 thoracic nerves (T1–T12) 5 lumbar nerves (L1–L5) 5 sacral nerves (S1–S5) 1 coccygeal nerve (Co1) The Cervical Region (C1–C8): The Brain’s Direct Line The cervical nerves, located at the top of the spinal column in the neck region, are crucial for upper-body movement and vital functions like breathing and heart rate regulation. Key Functions: C1–C4: Control the diaphragm, aiding breathing. Damage here can affect respiratory ability and may require ventilation support. C2: Governs head and neck movement, allowing nodding and turning. C3–C5: Support the phrenic nerve, directly linked to breathing. C4–C6: Influence the heart rate through autonomic control. C5: Controls movement in the shoulders, biceps, and elbows. C6–C8: Enable wrist extension, hand grip, and finger movements. Real Life Impact: Ever had your arm “fall asleep”? That’s temporary interference with these nerves. But permanent damage (like in a spinal injury) can result in partial or total paralysis of arms and hands — known as quadriplegia. The Thoracic Region (T1–T12): The Body’s Protective Core These nerves emerge from the mid-back and govern torso stability, organ control, and autonomic functions like temperature regulation and sweating. Key Functions: T1–T12: Control sympathetic tone — essential for functions like blood pressure, temperature regulation, and fight-or-flight responses. T2–T12: Support trunk stability, especially the intercostal muscles (between ribs). T11–L2: Involved in ejaculation and some bladder function. Real Life Impact: Damage to thoracic nerves is less common than cervical or lumbar injury but can affect balance, posture, and internal organ regulation. Even something like digestion or sweating might get disrupted. The Lumbar Region (L1–L5): Movers of the Lower Body This is where the power of movement shifts from upper to lower limbs. These nerves support walking, running, and posture. Key Functions: L2: Affects hip motion. L3: Responsible for knee extension. L4: Controls ankle dorsiflexion (lifting the foot). L5: Governs toe extension and knee flexion. Real Life Impact: Herniated discs or spinal stenosis often affect lumbar nerves, leading to sciatica — a radiating pain down the leg. Damage to these nerves can impair mobility and cause chronic pain or muscle weakness in the legs. The Sacral Region (S1–S5): Control Center of the Pelvis These nerves manage complex lower-body tasks like bowel, bladder, and sexual functions — tasks we don’t often think about until they don’t work properly. Key Functions: S1: Enables ankle movement and plantar flexion (pointing toes). S2–S3: Essential for bowel and bladder activity. S2–S4: Involved in sexual function. S5: Additional support for bowel/bladder control. Real Life Impact: Injuries here can result in incontinence, sexual dysfunction, or numbness in the pelvic area — all of which deeply impact quality of life and mental well-being. The Coccygeal Nerve (Co1): The Tail End There’s just one tiny coccygeal nerve, but it plays a role in pelvic floor support. Innervates coccyx and nearby muscles, including the levator ani — a key pelvic muscle for continence and posture. Real Life Impact: Though less commonly injured, issues here can result in coccygodynia (tailbone pain) or difficulty sitting for long periods. The Domino Effect of Nerve Damage Because spinal nerves are so specialized, injury to even a single one can throw off multiple systems. Depending on the location, nerve damage can lead to: Loss of sensation Paralysis Organ dysfunction Chronic pain (neuropathy) Muscle atrophy That’s why spinal injuries — whether from trauma, disc issues, or tumors — require immediate and specialized spinal cord injury treatment to prevent permanent nerve damage. Common Disorders and Conditions Involving Spinal Nerves Herniated Disc – A bulging disc compresses nearby nerves, causing pain, tingling, or weakness. Spinal Stenosis – Narrowing of the spinal canal puts pressure on nerves. Sciatica – Compression of the sciatic nerve (often from L4–S1 roots). Cauda Equina Syndrome – Emergency condition involving sacral nerve roots, resulting in loss of bladder/bowel control. Multiple Sclerosis – An autoimmune disease where the body attacks myelin around spinal nerves. Protecting Your Spinal Health It’s not just athletes or the elderly who need to watch their back — literally. Daily habits go a long way in keeping your spinal nerves healthy. Tips to Protect Your Spine: Maintain good posture Stretch and stay flexible Lift heavy objects with your legs, not your back Stay active — core strength = spinal support Avoid smoking — it restricts blood flow to spinal discs Invest in ergonomic furniture if you sit long hours Technology and the Future of Spinal Health With advances in neuroscience, treatment options for spinal nerve injuries are rapidly evolving. From nerve regeneration therapies to robotic exoskeletons and spinal cord stimulators, the future holds promise for those suffering from spinal damage. Research is even exploring brain-spine interfaces that can rewire communication between the brain and body using AI and implants. Final Thoughts We often underestimate the silent strength of the spinal cord and its nerves. They don’t demand your attention — until something goes wrong. But the more we understand this intricate network, the more we realize: your spine isn’t just your backbone, it’s the lifeline of your body’s every move, every feeling, and every function. Take care of your spine — because from head to toe, it has your back. Please enable JavaScript
Understanding Cervical Spondylosis: ICD-10

Understanding Cervical Spondylosis: ICD-10 Cervical Spondylosis ICD-10 is a cervical spine disorder that describes wear and tear in the bones, discs, and joints of the neck (cervical spine) due to aging. Patients diagnosed under this classification can explore appropriate cervical spondylosis treatment options based on clinical findings. Also called cervical osteoarthritis or degenerative disc disease of the neck, it is a common cervical spine disorder that can result in stiffness, pain, and other symptoms as the spinal elements degenerate. ICD-10 Code for Cervical Spondylosis ICD-10 refers to International Classification of Diseases, 10th Revision. It is a set of codes applied by physicians, hospitals, and insurers to identify and document diseases, conditions, and procedures. For cervical spondylosis, the ICD-10-CM code is M47. The specific code is based on whether the condition is due to nerve compression or other complications: 1) M47.812 – Cervical Spondylosis without Nerve Involvement a) It is utilized when there is degeneration in the neck but no significant effect on the nerves or spinal cord. b) Typical symptoms: Neck pain, stiffness, decreased flexibility. 2) M47.22 – Cervical Spondylosis with Radiculopathy a) Radiculopathy is when spinal nerves are compressed, resulting in pain, weakness, or numbness in the hands and arms. b) Symptoms: Pain shooting down the arms, tingling feelings, muscle weakness. 3) M47.12 – Cervical Spondylosis with Myelopathy a) Myelopathy occurs when the spinal cord is pressed on, impacting movement and coordination. b) Symptoms: Walking difficulties, loss of balance, hand and foot numbness. 4) M47.892 – Other Spondylosis in an Unspecified Region a) Applied if the particular location within the spine isn’t clearly defined. 5) M47.9 – Unspecified Spondylosis a) Applied when the precise details of the condition are not recorded. The Purpose of ICD-10 Codes ICD-10 codes are a standardized classification and coding system for diseases, medical conditions, and health disorders. The World Health Organization (WHO) developed the codes, which assist in providing a uniform language for healthcare providers, insurance organizations, and researchers globally. Key Purposes of ICD-10 Codes: 1. Proper Disease Classification: Aids physicians and medical coders in classifying diseases correctly depending on severity and symptoms. It ensures healthcare providers employ uniform terminology throughout various medical records. 2. Medical Diagnosis & Treatment Planning: Legal & Administrative Uses : Enables doctors to document a patient’s state accurately, ensuring the right treatment plan. Facilitates experts in recognizing the stage or severity of an illness while referring patients. 3. Insurance & Billing Processes: Used by hospitals and clinics to bill accurately for treatments from insurance claims. Helps insurane carriers determine coverage eligibility from the diagnosis of the patient. 4. Medical Research & Public Health Data Collection: Aids health organizations on both global and national levels in disease and outbreak monitoring trends. Enables policymakers to provide resources for disease prevention and healthcare improvement. 5.Legal & Administrative Uses: ICD-10 codes are typically needed in medicolegal reports in the event of insurance claims or malpractice suits. Used in healthcare systems to track mortality and morbidity rates. Importance of Cervical Spondylosis ICD-10 Codes in Healthcare ICD-10 codes play a crucial role in the smooth functioning of the healthcare system. Without these codes, medical diagnosis, treatment, billing, and research would be inconsistent and inefficient. 1. Improves Communication in Healthcare Standardized codes guarantee easy and clear communication between physicians, hospitals, insurance organizations and public health authorities. This also prevents misinterpretation of disease in various languages and medical systems. 2. Enhances Patient Care & Treatment Accurate coding guarantees the right diagnosis and treatment of patients and also assists in recording a patient’s medical history, thus making subsequent treatments more effective. 3. Ensures Smooth Insurance Processing & Billing Inaccurate or omitted ICD-10 codes may cause insurance claim denials or delays in insurance payment. Accurate coding minimizes administrative mistakes, allowing hospitals and clinics to be paid appropriately for services rendered. 4. Helps in Medical Research & Health Statistics Applied in epidemiology studies to monitor disease spread around the world. Helps governments develop healthcare policies and resources depending on disease rates. 5. Supports Standardization & Legal Compliance Most healthcare policies and laws mandate the utilization of ICD-10 codes in medical documentation. It ensures consistency in electronic health records (EHRs) for smooth patient care transitions. Causes of Cervical Spondylosis Aging: Natural wear and tear over time. Dehydrated Spinal Discs: Loss of cushioning between vertebrae. Bone Spurs: Excessive bone growth can put pressure on nerves. Herniated Discs: Bulging discs that press on surrounding structures. Previous Neck Injuries: Trauma can accelerate degeneration. Poor Posture & Lifestyle: Long hours of sitting, looking down at screens. Symptoms Persistent neck pain and stiffness. Headaches, especially at the back of the head. Tingling or numbness in arms and hands. Weakness in the arms. Difficulty with coordination and balance (if the spinal cord is involved). Treatment Options Cervical spondylosis management varies with symptom severity and ICD-10 classification. Non-Surgical (Conservative) Management: Physical Therapy: Posture-improving exercises and neck muscle strengthening Pain Management: NSAIDs, muscle relaxants, or corticosteroid injections Lifestyle Modifications: Correct ergonomics, avoidance of long periods of screen time, regular exercise Neck Braces: Support for temporary relief from neck strain Surgical Management (In Severe Cases): Decompression Surgery: To decompress the spinal cord or nerves Spinal Fusion: Stabilization of the cervical spine Disc Replacement: Replacing faulty discs with artificial devices Conclusion Cervical spondylosis is a prevalent yet controllable disease of the spine and neck. ICD-10 coding is crucial in diagnosing, managing, and recording it. Irrespective of whether the condition is mild (M47.81) or severe, myelopathy (M47.82) or radiculopathy (M47.22), prompt diagnosis and management will help to avert long-term complications. Knowledge of cervical spondylosis and ICD-10 coding guarantees that patients get right medical care, correct treatment, and insurance coverage. At We Are Spine, we promote healthy spines and urge people to come in early for any spinal or neck pain. Addressing issues today can help make your future healthy and pain-free. At We Are Spine, we believe in spinal health and early detection. Our mission is to make people aware of spinal diseases such as cervical spondylosis and offer professional advice on preventive management and treatment. With awareness, research, and cutting-edge medical interventions, we enable patients to enjoy a pain-free, active life. Please enable JavaScript in your browser to complete this form.Please enable JavaScript in your browser to complete this form.Full Name *Email *Phone Number * Submit
Spine Specialist in Borivali: Your Guide to Expert Care

Spine Specialist in Borivali Do you or your loved one experience chronic back pain, neck pain, or spinal disorders? Getting the proper spine specialist in Borivali can be the key to a successful journey towards recovery. Spine health is vital for overall health, and early intervention helps in avoiding complications. In this guide, we are going to discuss everything you need to know about spine specialists in Borivali, their specialty, and how to select the finest care for your spine health. Do you or your loved one experience chronic back pain, neck pain, or spinal disorders? Consulting a reputed spine surgeon in Borivali can be the key to a successful journey towards recovery. Understanding Spine Specialists: Who Are They? A spine specialist is a medical practitioner qualified to diagnose, treat, and manage different spinal disorders. The professionals may be orthopaedic surgeons, neurosurgeons, physiotherapists, or pain management physicians who specialize in spine issues. They employ advanced medical technology to address ailments such as: Herniated discs Sciatica Scoliosis Spinal stenosis Chronic back and neck pain Spinal injuries and fractures Degenerative disc disease Why You Need a Spine Specialist Spinal problems can drastically affect your daily life, hindering mobility, posture, and overall well-being. A specialist physician will offer a thorough diagnosis, customized treatment protocols, and, if required, surgical procedures. Early visits to a spine specialist ensure that you: Accurate diagnosis through imaging and clinical evaluation Minimally invasive treatment options Effective pain management Faster recovery and rehabilitation Preventing long-term complications Services Offered by Spine Specialist in Borivali 1. Diagnosis Borivali spine experts provide precise diagnoses of spine issues like herniated discs, scoliosis, and spinal stenosis through sophisticated imaging methods like MRI or CT scans. 2. Non-Surgical Treatments Choices that are not surgical include physical therapy, pain medication, and procedures like epidurals and nerve blocks, which are commonly described as minimally invasive treatment options. The objectives of such procedures are pain management and improvement of physical mobility. 3. Surgical Interventions Spine specialists would turn to spinal surgery like spinal fusion, disc replacement, or endoscopic spine surgery whenever surgery would best benefit the quality of life for patients. 4. Rehabilitation Post-therapeutic rehabilitation will assist in regaining strength and mobility. Individualized treatment schedules and exercise routines are formulated to enhance flexibility and increase muscle strength for rapid recovery. Why Choose We Are Spine? At We Are Spine, we are dedicated to providing world-class spine care with a patient-first approach. Here’s why you should choose us: 1. Expert Team of Spine Specialists Our experts possess great expertise in managing complicated spinal disorders. With a team of orthopaedic surgeons, neurosurgeons, and rehabilitation specialists, we provide holistic spine management. 2. Cutting-Edge Technology and Advanced Treatment Methods We make use of advanced diagnostic equipment and cutting-edge surgery, such as minimally invasive spinal surgery, robotic surgery, and advanced pain treatment therapies. Our state-of-the-art imaging systems and innovative surgeries assist in delivering accurate diagnoses and successful treatments, with little time for recovery and better outcomes for patients. 3. Personalized Patient Care Each patient is provided with a tailored treatment program specific to their individual condition and requirements. We favor non-surgical treatment and lifestyle changes first before resorting to surgery. Each patient is ensured to fully understand their condition and treatment options through our team, which promotes confidence and ease during their recovery process. 4. Holistic and Multidisciplinary Approach Our professionals work closely with physiotherapists, pain management professionals, and rehab specialists to give a well-rounded recovery plan to ensure long-term spinal wellness. We practice treating the cause, not the symptom, and merge several therapeutic methods like chiropractic practice, yoga, and posture correction to foster complete wellness. 5. Proven Success and High Patient Satisfaction We are proud of our excellent success rates and patient success stories. Our care and excellence have earned us the reputation as one of the most reliable names in spine care in Borivali. Our patients who undergo treatment at We Are Spine see enhanced mobility, less pain, and a better quality of life, thanks to our devoted staff and patient-friendly services. Our Spine Specialists in Borivali Every spine specialist at We Are Spine brings extensive experience and unwavering commitment to patient care. Dr. Aaditya Kashikar Dr. Aaditya Kashikar is a distinguished spine surgeon practicing in Mumbai and Thane, India, with over 14 years of experience. He specializes in addressing various spinal conditions, including back pain, sciatica, neck pain, radiating limb pain, walking difficulties, limb weakness, claudication, and bowel-bladder issues related to the spine. His holistic approach enables him to distinguish between spine-related and non-spine-related issues, often treating patients through conservative, non-surgical methods. Educational Background MBBS: Completed at Maharashtra University of Health Sciences (MUHS), Nashik. DNB in Orthopaedics: Achieved at Bangalore Baptist Hospital, affiliated with Christian Medical College (CMC), Vellore. Fellowships & Educational Background: Spine Foundation Fellowship, Mumbai, under Dr. Shekhar Bhojraj, focusing on comprehensive spine surgeries and conservative treatments. International Fellowship in Minimally Invasive Spine Surgery at Rush University Medical Center, Chicago, USA. Short-term fellowships under Dr. Saumyajit Basu (Park Clinic, Kolkata), Dr. Sajan Hegde (Apollo Hospital, Chennai), and Dr. S.R. Rajasekaran and Dr. Ajoy Shetty (Ganga Hospital, Coimbatore). Professional Experience Dr. Kashikar has served as an associate spine surgeon at several renowned hospitals in Mumbai, including Lilavati Hospital, VN Desai Hospital, Breach Candy Hospital, and Wockhardt Hospital. He has also been the chief spine surgeon at Wockhardt Hospital, North Mumbai, and is affiliated with other corporate hospitals in Mumbai and Thane for consultations and surgeries. Areas of Expertise Minimally Invasive Spine Surgery (MISS): Dr. Kashikar has undergone advanced training in MISS at Rush University Medical Center in Chicago, USA. This technique involves smaller incisions, leading to reduced postoperative pain, shorter hospital stays, and quicker recovery times for patients. Endoscopic Spine Surgery: He specializes in endoscopic procedures, utilizing small cameras and instruments to address spinal issues with minimal disruption to surrounding tissues. This approach is particularly beneficial for conditions like herniated discs and spinal stenosis. Comprehensive Spine Care: Dr. Kashikar manages a wide spectrum of spinal conditions, including: Degenerative
Transform Your Back Pain: Discover the Ultimate 30-Minute Yoga Asana Routine for Sciatica!

Transform Your Back Pain: Discover the Ultimate 30-Minute Yoga Asana Routine for Sciatica! Sciatica is a painful condition that radiates from the lower back down the legs, causing tingling, numbness, or stinging pain. A herniated disc, tense muscles, or prolonged sitting can all cause pain that interferes with daily activities. The centuries-old practice of yoga is a natural and effective remedy for sciatica, even though painkillers and medical interventions can lessen the pain. However, if symptoms persist or worsen, consulting a reputed spine hospital in Mumbai can help diagnose the underlying cause and ensure safe, comprehensive care. Yoga improves spinal alignment, increases circulation, and encourages relaxation in addition to strengthening and stretching the muscles that surround the sciatic nerve. Yoga helps the body heal from within by releasing tension, reducing inflammation, and restoring mobility through mindful movement and deep breathing. This 30-minute yoga routine for sciatica relief offers a progressive flow of stretches, strength-building poses, and relaxation techniques that are specifically crafted to address the underlying causes of sciatic pain. These poses will assist you in regaining ease and comfort in your everyday movements, regardless of your level of experience. Here’s a comprehensive guide to 10 yoga poses that can help with sciatica pain, as well as a planned 30-minute workout that keeps things interesting and productive. Yoga Routine for Sciatica Relief (30-Minute Flow) Duration: 30 minutesFrequency: 4-5 times per weekBest Time: Morning or evening Warm-Up (5 minutes) Cat-Cow Pose (1-2 minutes) Child’s Pose (1 minute) Downward Dog (30-60 seconds) Strengthening & Stretching (20 minutes) Cobra Pose – 3 rounds (20-30 sec each) Pigeon Pose – Hold for 30-60 sec per side Bridge Pose – 2-3 rounds (30-45 sec each) Supine Spinal Twist – Hold for 30-60 sec per side Reclining Hand-to-Big-Toe Pose – 30 sec per leg Seated Forward Bend – Hold for 30-60 sec Relaxation & Cool Down (5 minutes) Legs Up the Wall – 3-5 minutes All the yoga poses mentioned in the routine are further explained, including detailed instructions on how to perform them. How to Make This Routine Fun & Engaging Create a Sciatica-Healing Playlist – Soft instrumental, yoga beats, or even your favorite calm songs. Use Essential Oils – Try lavender or peppermint for an added sensory experience. Practice in a Cozy Space – Dim the lights, light a candle, and make it your moment of peace. Track Your Progress – Note how you feel before and after. Small wins add up! Do It with a Friend – Yoga is even better with a buddy! Use Props – Yoga blocks, cushions, or straps for comfortEnd with Deep Breathing – Helps calm the nervous system This isn’t just a yoga routine—it’s self-care for your spine. After one session: You’ll feel looser and more relaxed. After a week: You’ll notice reduced stiffness and pain. After a month: Your flexibility, strength, and mobility will improve significantly 10 Best Yoga Asanas for Sciatica Relief 1. Downward-Facing Dog (Adho Mukha Svanasana) Releases tension along the sciatic nerve by stretching the lower back, hamstrings, and calves. How to do it:• Begin on your hands and knees at a tabletop position.• Raise your hips, straighten your legs, and tuck your toes.• Keep your heels slightly raised or in contact with the floor while pressing your palms into the mat.Hold for 30 to 60 seconds while taking deep breaths. Adjustment: Bend your knees a little if your hamstrings feel too tight. 2. Child’s Pose (Balasana) A gentle pose that relaxes the nervous system and relieves tension in the lower back. How to do it: Sit with your knees wide apart on your heels. Place your forehead on the mat and extend your arms forward.Hold for one to two minutes while taking deep breaths. Adjustment: If your hips don’t reach your heels, place a cushion beneath them. 3. Cobra Pose (Bhujangasana) Reduces nerve compression by opening up the spine and strengthening the lower back. How to do it: Place your hands beneath your shoulders while lying on your stomach. Maintaining a slight bend in your elbows, press into your hands and raise your chest. Repeat two or three times while holding for 20 to 30 seconds. Adjustment: Maintain the elbows in a low cobra position on the mat if you experience lower back pain. 4. Pigeon Pose (Eka Pada Rajakapotasana) Stretches the piriformis muscle, which can compress the sciatic nerve, and opens the hips. How to do it: • First sit in a downward dog position.• Place your right knee behind your right wrist and bring it forward.• Lower your torso over your right leg by extending your left leg back.• After 30 to 60 seconds of holding, switch sides. Adjustment: If it feels too strenuous, put a cushion beneath your hip. 5. Bridge Pose (Setu Bandhasana) Enhances spinal alignment by strengthening the hamstrings, glutes, and lower back. How to do it: Keep your feet hip-width apart, bend your knees, and lie on your back. Lift your hips towards the ceiling while pressing into your feet. Hold for 30 to 45 seconds, then do this two or three times. Adjustment: For a supported bridge, place a yoga block beneath your sacrum. 6. Reclining Hand-to-Big-Toe Pose (Supta Padangusthasana) Reduces sciatic nerve pain by gently stretching the lower back and hamstrings. How to do it:• Raise one leg while lying on your back.• Use a strap around your foot or hold your big toe.• For 30 seconds, hold the opposing leg grounded.• Change sides. Adjustment: Wrap a strap around your foot if you are unable to reach it. 7. Supine Spinal Twist (Supta Matsyendrasana) Decompresses the lower back and eases spinal stiffness. How to do it: Raise your right knee to your chest while lying on your back While keeping your shoulders grounded, drop it across your body. After 30 to 60 seconds of holding, switch sides. Adjustment: If the knee does not touch the floor, place a pillow beneath it. 8. Cat-Cow Pose (Marjaryasana-Bitilasana) Promotes better circulation and spinal mobility. How to do it: Start in a tabletop position Take a breath, raise your head, and arch your back (Cow Pose). Exhale, tuck your chin into Cat Pose, and round your spine. Repeat in a slow, flowing motion
Spine Tumor: A Curse or a Call to Action?
Spine Tumor: A Curse or a Call to Action? The Day Everything Changed For many people, a spine tumor diagnosis is one of the most terrifying phrases they’ll ever hear. It imagine images of wheelchairs, intense pain and worst-case scenarios. It’s the kind of news that silences a room, sends hearts racing and minds spiralling into a pit of “what ifs.” But here’s the truth—yes, a spine tumor is serious, but it’s not always a death sentence. It’s not always cancer. And it’s certainly not the end of the road. In fact, for many, it becomes a wake-up call—a reason to slow down, pay attention, seek clarity, and take control of their health. In this blog, we’re going to humanize the journey, bust the myths, and remind you that knowledge is power. Let’s step into the story not just with fear, but with facts, science, and strength. What Is a Spine Tumor? A Quick Overview A spine tumor is an abnormal growth of tissue within or surrounding the spinal column and spinal cord. These tumors can be: Primary (originating in the spine or spinal cord) or Metastatic (spreading from cancers elsewhere in the body) Benign – non-cancerous, but potentially harmful if they press on nerves or spinal tissue Malignant – cancerous and potentially life-threatening Spinal tumors are uncommon, but when they do happen, the effects can be subtle or catastrophic. And though the medical jargon sounds hard and clinical, behind each diagnosis is a very personal experience—filled with fear, hope, decision, and resilience. 5 Common Myths About Spine Tumors—and the Real Truth Behind Them Despite medical advances, spine tumors remain clouded in fear and misconception. Let’s clear the fog with some truth. Myth 1: “All Spine Tumors Are Cancerous” The Truth: This is among the most frequent and most frightening misconceptions. The term tumor doesn’t necessarily indicate cancer. Most spinal tumors are benign, that is, they don’t spread to other parts of the body. Examples include: Meningiomas – often benign and slow-growing, more common in women Schwannomas – nerve sheath tumors that rarely turn cancerous Hemangiomas – vascular tumors usually found incidentally during scans While benign tumors can still press on nerves and cause pain or weakness, they are often treatable, and the prognosis is usually very good. It’s not the label that determines danger—it’s the location and impact on your spinal cord and nerves. Myth 2: “Spine Tumors Are Always Primary (Start in the Spine)” The Truth: In fact, most tumors of the spine are metastatic, i.e., they’ve spread from cancers in other parts of the body—most often the breast, lung, prostate, or kidney. The spine is actually one of the most common locations for cancer metastasis. If a person with a history of cancer begins to develop chronic back pain, numbness, or weakness in the legs, it may be a warning sign that the cancer has spread. Early detection helps to prevent spinal cord compression and permanent neurological damage that can occur. But here’s the opposite: even people without a history of known cancer can get primary spine tumors such as chordomas or astrocytomas, although these are less common. Myth 3: “Spine Tumors Are Always Fast-Growing and Deadly” The Truth: Many people hear the word “tumor” and imagine something that’s aggressively multiplying and out of control. But the truth is, many spinal tumors grow slowly—sometimes over months or even years—and some may never grow at all. Examples of slow-growing tumors include: Schwannomas Ependymomas Hemangioblastomas These tumors can be followed routinely by imaging and don’t always need immediate surgery or treatment. Not all tumors are ticking time bombs. With routine monitoring and informed medical advice, many patients can live comfortably and safely with a spinal tumor for years. Myth 4: “Once You Have a Spine Tumor, You’ll Be Disabled for Life” Truth: This fear, while deeply emotional, is often unfounded. Thanks to minimally invasive spine surgery, neuronavigation, and microsurgical techniques, many patients recover well and go back to living fully active lives. Disability depends more on the tumor’s location and how early it’s treated than the diagnosis itself. Physical rehabilitation post-treatment can restore strength, mobility, and confidence in many cases. Myth 5: “Imaging Scans Like MRI Are Dangerous or Painful” Reality: MRI (Magnetic Resonance Imaging) is safe, painless, and non-invasive. It uses magnetic fields—not radiation—to produce detailed images of soft tissues, spinal cord, and nerves. The machine may look intimidating and feel noisy, but it’s completely painless and crucial for spine tumor diagnosis. MRI provides: Detailed images of soft tissue Clear visuals of the spinal cord and nerve roots Early detection of even tiny tumors MRI is the gold standard for spine tumor diagnosis. Delaying a scan out of fear can lead to worse outcomes. The test is usually over in 30–45 minutes, and early detection through imaging often saves function—and lives. Recognizing the Signs: When Should You Be Concerned? Spine tumors can present subtly at first. Symptoms may mimic everyday spine issues like a slipped disc or nerve compression. But some red flags include: Persistent back pain, especially at night Unexplained weakness or numbness in arms or legs Difficulty walking or balancing Loss of bowel or bladder control Tingling, burning, or shooting pain in the limbs If these symptoms persist or worsen, especially without a clear cause, they warrant urgent medical evaluation. Diagnosis: From Doubt to Clarity A comprehensive diagnosis typically involves: Neurological examination MRI scan – for soft tissue visualization CT scan – to assess bone involvement Biopsy – to determine the tumor’s exact nature An early, accurate diagnosis is the bridge between uncertainty and hope. It helps doctors choose the most effective treatment path—whether surgical, radiological, or medical. Treatment: Modern Medicine Has Changed the Game Treatment today is not what it was 10–15 years ago. Here’s what’s possible now: Surgery: Often minimally invasive, aimed at removing the tumor with precision Radiation therapy: Targeted radiation for malignant or inoperable tumors Chemotherapy: Used in cases of metastatic or systemic cancer Rehabilitation: To restore function and quality of life post-treatment Patients who once faced a grim outlook now have the chance to recover and thrive, thanks to medical innovation. Emotional Impact and the Power of Support The journey doesn’t
Say Goodbye to Neck Pain: 15 Must-Try Exercises for Cervical Spondylosis and a Game-Changing Workout Routine!

Say Goodbye to Neck Pain: 15 Must-Try Exercises for Cervical Spondylosis and a Game-Changing Workout Routine! Cervical spondylosis, also known as cervical osteoarthritis, occurs due to age-related wear and tear of the neck’s bones and discs. Poor posture, excessive screen time, and a sedentary lifestyle can accelerate this process, leading to symptoms like stiffness, pain, reduced mobility, and even nerve compression. But don’t worry! The right combination of stretching, strengthening, mobility, and postural exercises can work wonders for your neck health. These exercises are most effective when included as part of a structured cervical spondylosis treatment plan tailored to the severity of the condition. Dealing with cervical spondylosis doesn’t mean you have to live with constant neck pain and stiffness. The good news is that with the right exercises and an engaging workout routine, you can improve your neck mobility, strengthen your muscles, and reduce discomfort—all while making your fitness journey enjoyable. Instead of letting stiffness take control, why not take charge of your well-being with a simple yet effective workout? That’s why this guide not only provides 15 highly effective exercises but also introduces an interesting workout routine designed to keep things fresh and engaging. This structured workout will help you stay consistent, enjoy the process, and maximize the benefits without feeling overwhelmed. By dedicating just a few minutes daily to these exercises, you’ll experience improved flexibility, better posture, and stronger neck muscles—all while reducing the risk of further complications. Let’s get started and make your journey to a pain-free neck both effective and enjoyable! Workout Routine for Cervical Spondylosis Frequency: Daily or at least 4–5 times per weekDuration: 15–20 minutes yoga routine for sciatica relief Warm-Up (3–5 minutes) Shoulder Rolls – 10 reps forward, 10 reps backward Neck Side Tilt – Hold each side for 10 seconds Neck Rotation – 5 reps each side Main Routine (10–12 minutes) Chin Tucks – 10 reps Neck Retractions – 10 reps Upper Trapezius Stretch – Hold for 10 seconds per side Isometric Neck Press – Hold for 5–10 seconds (3 reps) Isometric Side Resistance – Hold for 5–10 seconds per side (3 reps) Wall Angels – 10 reps Scapular Squeeze – 10 reps Cool-Down (2–3 minutes) Seated Cat-Cow Stretch – 5 reps Thoracic Extension – Hold for 10 seconds Deep Breathing – Inhale for 4 sec, exhale for 6 sec This structured workout routine can help manage cervical spondylosis effectively while improving neck flexibility, strength, and posture. Stay active and take care of your spine! Detailed Explanation of Each Exercises for Cervical Spondylosis Each of these exercises helps improve flexibility, strength, and posture while relieving neck stiffness and pain. Here’s a step-by-step breakdown of how to perform them correctly: While home exercises are highly effective, combining them with physiotherapy for cervical pain ensures proper technique, faster recovery, and personalized care based on the severity of cervical spondylosis. Stretching Exercises Neck Flexion (Chin to Chest) Sit or stand with your back straight. Slowly lower your chin towards your chest until you feel a gentle stretch at the back of your neck. Hold this position for 10 seconds. Slowly return to the starting position. Repeat 5–10 times. Benefit: Stretches the muscles at the back of the neck, relieving tension and reducing stiffness. Neck Extension (Look Up) Sit or stand with a straight posture. Slowly tilt your head backward, looking up at the ceiling. Hold this position for 10 seconds. Return to the starting position slowly. Repeat 5–10 times. Benefit: Stretches the front of the neck and strengthens the supporting muscles, improving mobility. Neck Side Tilt (Ear to Shoulder) Sit or stand with your head in a neutral position. Slowly tilt your head to one side, bringing your ear toward your shoulder. Keep your opposite shoulder relaxed. Hold for 10 seconds, then switch sides. Repeat 5 times on each side. Benefit: Loosens tight neck muscles and improves side-to-side flexibility. Neck Rotation Sit upright and slowly turn your head to one side as far as comfortable. Hold this position for 10 seconds. Return to the center, then rotate to the opposite side. Repeat 5 times per side. Benefit: Enhances flexibility, range of motion, and reduces stiffness. 5. Upper Trapezius Stretch Sit in a chair and hold onto the seat with one hand. Tilt your head in the opposite direction, bringing your ear toward your shoulder. Hold for 10 seconds, feeling the stretch in your upper shoulder and neck. Switch sides and repeat.Benefit: Relieves tension in the upper trapezius muscles, reducing neck and shoulder discomfort. Strengthening Exercises Chin Tucks Sit or stand tall. Pull your chin straight back (as if making a double chin) while keeping your head level. Hold for 5 seconds, then relax. Repeat 10 times. Benefit: Strengthens deep neck muscles, improves posture, and alleviates neck strain. Isometric Neck Press Place your palm on your forehead. Gently press your head forward while resisting the movement with your neck muscles. Hold for 5–10 seconds, then relax. Repeat 3–5 times. Benefit: Strengthens the front neck muscles without excessive movement, helping stabilize the cervical spine. Isometric Side Resistance Place your palm against the side of your head. Press your head into your hand while resisting the movement with your neck muscles. Hold for 5–10 seconds, then switch sides. Repeat 3–5 times per side. Benefit: Strengthens the side neck muscles, improving stability and support for the head. Neck Retractions Sit with your head in a neutral position. Pull your head straight back while keeping your chin level (as if making a double chin). Hold for 5 seconds, then return to the starting position. Repeat 10 times. Benefit: Corrects forward head posture and relieves tension. Wall Angels Stand with your back against a wall, feet slightly away from the wall. Keep your lower back, upper back, and head in contact with the wall. Raise your arms to form a 90-degree angle, then slowly move them up and down like making a snow angel. Perform 10 reps. Benefit: Improves posture, strengthens the upper back, and prevents neck strain. Mobility & Postural Exercises Shoulder Rolls Sit or stand tall. Roll your shoulders forward in a circular motion 10 times. Then roll them backward 10 times. Benefit: Releases tension, improves blood
Cervical Spondylosis: Symptoms, Causes, and the Latest Innovations in Treatment!
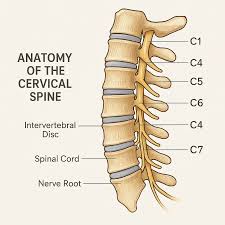
Cervical Spondylosis: Symptoms, Causes, and the Latest Innovations in Treatment! Cervical spondylosis is a degenerative joint disease and if you’re seeking expert diagnosis and care, a trusted spine clinic in Mumbai can guide you from evaluation to recovery. The condition is largely caused by age-related wear and tear but can also be the result of lifestyle factors, trauma, and genetics. Let us discuss the condition in detail. Depending on the severity of symptoms, patients may require medical, physiotherapy-based, or advanced cervical spondylosis treatment. Understanding the Cervical Spine The cervical spine contains seven vertebrae (C1 to C7) which support the head and facilitate movement of the neck. Between vertebrae lie intervertebral discs which are cushion-like and shock-absorbing. They consist of a tough outer cover (annulus fibrosus) and a soft, gelatinous core (nucleus pulposus). Ligaments also support it, and spinal nerves travel in small holes, transmitting impulses to the arms and upper limb. As we get older, these structures start breaking down, and this results in cervical spondylosis. What Causes Cervical Spondylosis? a. Aging and Wear & Tear Intervertebral discs lose water and elasticity over time, so they are not as good at shock absorption. Disc height decreases, which means vertebrae rub against each other more. The body attempts to compensate by developing bone spurs (osteophytes), which can compress nerves and result in pain b. Herniated Discs Small cracks may develop in the outside covering of discs, letting the inner gel escape. This irritates surrounding nerves, causing pain, numbness, or tingling. c. Ligament Stiffness Spinal ligaments can thicken and become less flexible with age, limiting neck motion. d. Past Neck Injuries Injury from falls, accidents, or overuse can accelerate disc deterioration. e. Lifestyle Habits Slouching, excessive screen time, inadequate exercise, and bad posture may add unnecessary stress to the neck, resulting in premature degeneration. f. Genetic Factors An inherited family history of arthritis or spinal disease might enhance your likelihood of experiencing cervical spondylosis. On the left, a healthy cervical spine with thick discs and wide spinal canal. On the right, signs of cervical spondylosis are visible—disc degeneration, bone spurs, and nerve compression. Identifying the Symptoms The symptoms differ from individual to individual, some individuals never feel any pain, while others experience continuous discomfort. Following are some of the common symptoms. Many of these symptoms can be managed with physiotherapist-guided neck exercises for cervical spondylosis, depending on severity:: Neck stiffness and pain, usually more severe after extended periods of immobility. Headaches, typically from the back of the skull. Sensation of numbness or tingling in arms and hands (indicative of nerve compression). Weakening of arm and shoulder muscles, impairing grip strength. Crackling or grating sensation with neck movement owing to joint wear and tear. Severe Symptoms (Spinal Cord Compression): Loss of balance and walking difficulty. Bladder or bowel dysfunction (Seek medical attention at once). Diagnosing Cervical Spondylosis Physicians employ a variety of means to diagnose the disorder: Physical Examination Assessing neck flexibility, muscle power, and reflexes. Examining nerve function using sensation tests. Imaging Tests X-rays: Show bone spurs and alignment problems. MRI (Magnetic Resonance Imaging): Gives a detailed picture of discs, nerves, and soft tissues. CT Scan: Assists in detecting bone defects. Nerve Function Tests Electromyography (EMG): Assesses muscle electrical activity. Nerve conduction studies: Assess how well nerves conduct signals. How is Cervical Spondylosis treated? The majority of cases don’t need surgery and can be treated with the following methods: Medications NSAIDs or painkillers reduce pain and inflammation. Muscle relaxants relieve spasms and stiffness. Corticosteroid injections offer relief from acute pain. Medications for nerve pain such as gabapentin may relieve nerve-related pain. Physical Therapy Exercises to strengthen the neck and shoulders. Techniques to correct posture. Flexibility exercises through stretching routines. Heat and Cold Therapy Cold packs: Reduce swelling and numb pain. Heat therapy: Relaxes muscles and enhances blood flow. Changes in Lifestyle Monitor posture—sit straight and do not slouch. Take breaks from the screen to minimize neck strain. Purchase ergonomic chairs and workstations. Exercise regularly and include neck-friendly exercises. Alternative Therapies Chiropractic adjustments can improve mobility. Acupuncture has been shown to manage chronic pain. Yoga and stretching enhance flexibility and diminish stiffness. When Surgery is Necessary Surgery is only considered if conservative measures are not effective, or if compression of the nerve results in severe symptoms. The most common operations are: Laminectomy: Removing part of the vertebra to decompress. Discectomy: Removing a ruptured disc compressing nerves. Spinal Fusion: Joining two vertebrae to stabilize the spine. How to Prevent Cervical Spondylosis? Growing old is unavoidable, but you can retard spinal degeneration by adopting small but significant lifestyle changes: Maintain good posture: Sit and stand with straight back to prevent unnecessary strain. Remain active: Exercise regularly strengthens muscles of the neck and back. Take breaks from screens: Avoid leaning forward to look at phones or computers for extended periods. Employ ergonomic furniture: A good monitor and chair arrangement can make a huge difference. Drink plenty of water: Keeps intervertebral discs healthy and in good working condition. Quit smoking: Enhances blood flow, keeping spinal structures in good condition. By doing this, you are able to keep your neck in good health and minimize discomfort to the maximum! Exploring New and Evolving Treatments for Cervical Spondylosis Though conventional treatments such as medications, physical therapy and lifestyle modifications continue to help in the treatment of cervical spondylosis but the spine care world is not static. In recent years, newer and more sophisticated treatment methods have begun to gain popularity. Some of these new treatments are already in practice where as others are still under research for long-term efficiency. It’s always best to consult with your doctor to determine which treatment may be suitable for your particular condition. But to give you an idea of what’s available, here are some of the newer and upcoming treatments for cervical spondylosis: 1. Interventional Procedures Radiofrequency Ablation (RFA): This minimally invasive treatment employs heat to “turn off” the nerves that
Transform Your Sleep: The Essential 5 Slip Disc Sleeping Positions for Ultimate Relief

Transform Your Sleep: The Essential 5 Slip Disc Sleeping Positions for Ultimate Relief A herniated or prolapsed disc, sometimes referred to as a slipped disc, can be extremely uncomfortable, particularly when you’re trying to fall asleep. Sleeping in the right positions can help to reduce pain, spinal alignment and in healing. The best sleeping positions for people with a slipped disc will be covered in this guide, along with advice on how to improve sleep. Understanding a Slipped Disc When the soft, gel-like core of an intervertebral disc pushes through its outer layer and presses against surrounding nerves, it is known as a slipped disc. Pain, numbness, tingling and weakness are possible side effects of this condition, especially in the neck, lower back, or in limbs. A good night sleep and less strain on the spine depend on choosing the correct sleeping position. 5 Best Sleeping Positions for Slip Disc Recovery 1. Sleeping on Your Back with Knee Support Why it helps: It reduces pressure on the damaged disc, this position preserves the spine’s natural curvature. How to do it: Lie flat on your back. To reduce the pressure on your lower back, place a pillow under your knees. Support your head and neck with a pillow. Additional tip: The best spinal support comes from a mattress that is medium-firm. 2. Side Sleeping with a Pillow Between the Knees Why it helps: This position keeps the spine aligned and prevents unnecessary twisting How to do it: Lie in a foetal position on your side. To maintain the alignment of your hips and lower spine, place a pillow between your knees. To keep your neck in alignment, place a supportive pillow under your head. Additional tip : Try sleeping on the other side to relieve pressure if one side hurts more. 3. Fetal Position (Curled-Up) Why it helps: By creating space between vertebrae, the fetal position can lessen the pressure on the slipped disc. How to do it: The first step is to lie on your side. Bring your knees up to your chest. For additional support, place a pillow between your knees. Additional tip: People with lumbar disc herniation benefit most from this position. 4. Sleeping on Your Stomach with a Pillow Under the Hips (For Select Cases) Why it helps: Although it is not advised for most people, this position can help people with a particular kind of disc herniation by relieving pressure on their spine. How to do it: Place yourself on the stomach. To keep your spine aligned, place a pillow beneath your hips. Place a thin pillow beneath your head, or none at all. Additional tip: Try a different position if this one makes your symptoms more worse. 5. Reclined Sleeping Position (Using a Recliner or Adjustable Bed) Why it helps: Particularly for those with lumbar disc problems, a reclining position can relieve spinal compression. How to do it: Make use of a recliner or an adjustable bed. Keep your knees slightly bent and raise your upper body. To maintain appropriate spinal posture, make sure you have lumbar support. Additional tip: By simulating the zero-gravity posture, this position may help decompress the spine. What to Avoid When Sleeping with a Slipped Disc 1. Sleeping on Your Stomach Without Support Without the proper support, lying flat on your stomach can put too much strain on your spine, which can increase your symptoms. Avoid: Using a thick pillow under your head, as it may strains your neck and back. Alternative: Use a thin pillow beneath your head and a pillow beneath your hips if you have to sleep on your stomach. 2. Sleeping in a Twisted Position Rotating your spine while sleeping can increase pain and put uneven pressure on the disc. Avoid: Sleeping with one leg stretched out and the other bent, as it causes spinal misalignment. Alternative: Keep your legs aligned or use a pillow between your knees when side sleeping. 3. Sleeping on a Soft Mattress Poor spinal alignment results from a mattress that is too soft or sagging to offer sufficient support. Avoid: Sleeping on a very soft mattress that lets your hips sink too much. Alternative: Opt for a medium-firm or firm mattress that supports spinal alignment. 4. Using an Unsupportive Pillow An incorrect pillow height can strain the neck and contribute to spinal misalignment. Avoid: Using a very high or very low pillow that tilts the head unnaturally. Alternative: Choose a supportive pillow that keeps your neck in a neutral position. Additional Sleep Tips for Slipped Disc Recovery 1. Choose the Right Mattress Since it strikes a balance between comfort and support, a medium-firm mattress is typically advised. Mattresses that are too hard or too soft should be avoided as they can increase spinal misalignment. 2. Use Proper Pillows A contoured memory foam pillow can support your neck and keep the spine aligned. A wedge pillow can be helpful for those who benefit from a reclined position. Avoid very thick pillows or multiple pillows as they can strain your neck. 3. Maintain a Consistent Sleep Routine Try to go to bed and wake up at the same time every day. Establish a relaxing bedtime routine, such as gentle stretching or meditation. Avoid screens and caffeine close to bedtime. 4. Apply Heat or Ice Before Bed Before going to bed, put an ice pack or heating pad to the affected area can help reduce pain and inflammation and enhance the quality of your sleep. 5. Perform Gentle Stretching Before Sleep Before bed, you can improve spinal alignment, ease stiffness, and relax your muscles with some light yoga or stretches. When to See a Doctor In rare cases where conservative treatments fail and symptoms continue to worsen, surgical intervention may be recommended. If surgery becomes necessary, understanding the spine surgery cost in Maharashtra can help patients and families plan informed and stress-free treatment decisions.See a healthcare provider if pain doesn’t go away after trying different types of sleeping positions.

